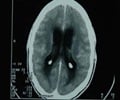
Acute encephalitis syndrome (AES) in Bihar, India has claimed the lives of 133 children so far. It is suspected that toxins present in litchi could be the cause of the illness.
- There is currently an outbreak of acute encephalitis syndrome (AES) that is ongoing in Bihar, India
- It has taken the lives of 133 children so far
- Toxins present in litchi are suspected to have caused the deaths
In fact, between 2008 and 2014, there have been over 44,000 cases and around 6,000 deaths from AES in India, especially in Uttar Pradesh and Bihar.
TOP INSIGHT
An outbreak of acute encephalitis syndrome (AES) is currently ongoing in Bihar, India, which has killed 133 children so far. Toxins present in litchi have been suspected to be the cause of death.
Read More..
Changing Landscape of Acute Encephalitis Syndrome (AES) in India
The patterns of AES in India, based on the causative agent, have changed appreciably over the years, which are briefly highlighted below:- Pre-1975: JEV was incriminated in only a few AES cases
- 1975-1999: Major cause of AES was JEV
- 2000-2010: Major causes of AES were Chandipura virus, Nipah virus and enteroviruses
- Post-2010: Major cause of AES has been litchi toxin, primarily in northern India
Acute Encephalitis Syndrome (AES) Outbreak in Bihar
In the current AES outbreak in Bihar, cases have been detected in 12 districts, including Muzaffarpur, East Champaran, and Vaishali, with Muzaffarpur being the worst affected. Poor children below the age of 10 years have been affected. They are usually fine while going to sleep, but wake up in the morning with high fever, vomiting, convulsions, and seizures, with one-in-three cases, resulting in death within 24 to 36 hours. Over the past decade, more than 1,350 children have died from AES in Bihar, with a record number of 355 in 2014. As of Friday 28th June, 2019, the death toll in Muzaffarpur stands at 133.Acute Encephalitis Syndrome (AES) in India – The Litchi Connection
AES is generally associated with JEV, which is spread by the bite of infected Culex mosquitoes. However, in the current outbreak in Bihar there is hardly any evidence that JEV was involved (only two cases of JEV have been detected). So, there has been a focus on litchis as a possible causative agent, based on circumstantial evidence.Outbreaks of AES are not new to the region. They have occurred since 1995 during the summertime in and around Muzaffarpur, which coincides with the litchi season. Muzaffarpur is sometimes regarded as India’s ‘Lichi Paradise’ as there are numerous litchi orchards in the region, producing huge quantities of the fruit. This is also one of the poorest regions in India. Therefore, it is highly likely that poor, malnourished, children could consume excess amounts of litchis on an empty stomach out of sheer hunger.
Where Else Has Litchi been Incriminated?
It is not just India, where litchi has been incriminated as a causative agent of AES. Outbreaks of AES have also been observed in litchi-growing regions of Bangladesh and Vietnam. For example, in 2012, a major outbreak was reported from Dinajpur district in northern Bangladesh. AES outbreaks have also been reported from the Bac Giang Province in northern Vietnam since the end of the 1990s, which coincided with the litchi harvesting season. Other countries where there is concern of AES arising from litchi toxicity include southern China, northern Thailand, the Terai of the Central and Eastern Development Regions of Nepal, and the Cordillera Autonomous Region of the Philippines.Mechanism of Action of Litchi Toxicity
A research study conducted in 2017 identified two toxins in litchi seed, called methylene cyclopropyl acetic acid (MCPA) and methylene cyclopropyl glycine (MCPG). Both toxins block a metabolic pathway called gluconeogenesis, which synthesizes glucose from non-glucose sources such as proteins and fats, thereby helping the body to maintain adequate blood sugar levels. However, since the toxins stop gluconeogenesis, blood sugar levels plummet, resulting in severe hypoglycemia. Hypoglycemia is accompanied by aminoacidemia, which results in brain damage due to the development of full-blown AES.Litchi – Just the ‘Tip of the Iceberg’
It should be noted that people residing in the litchi-growing areas of Bihar, such as Muzaffarpur – often called the ‘Litchi Bowl’ of India – live in abject poverty, often struggling to find two square meals a day. Under these circumstances, it is but natural that children of these families eat litchis on an empty stomach. Since these children are severely malnourished, their blood sugar levels are already low due to depletion of glycogen reserves in the liver, thereby necessitating gluconeogenesis. However, since the litchi toxins (MCPA and MCPG) block gluconeogenesis, it results in brain damage due to a condition called hypoglycemic encephalopathy – a manifestation of AES. This does not happen in healthy, well-nourished children, who have adequate glycogen reserves in the liver to replenish the low blood glucose levels. Therefore, it becomes apparent that it is not just the litchis, but also malnourishment arising from severe poverty that is responsible for the fate of these unfortunate children.Human Tragedy – More Than Meets the Eye!
There are multiple factors at play that are responsible for the deaths of 133 children in Muzaffarpur, so far. Litchi is just one factor that acted as a trigger, while the underlying causes are many, which have widespread ramifications. Some of these are highlighted below:- Poor Health Index: Bihar has the highest number (48.3%) of stunted children below 5 years in India. Moreover, almost 60 percent of children are anemic and 43 percent are underweight. This has resulted in an overall low malnutrition index for the state
- Poverty: Poverty is at the root of many social evils. For example, as per the 2018 Global Hunger Index, India ranked 103rd out of 119 qualifying countries, which is but a reflection of the level of poverty in the country
- Illiteracy: This is still a major problem in India, despite concerted efforts by the government and other agencies. As a result of illiteracy, parents can’t read or understand the information in pamphlets distributed by health workers
- Government Inaction: The Bihar Government carries out encephalitis awareness drives in Muzaffarpur and adjoining districts every year at this time, which has led to a significant reduction of AES cases in recent years. But this year the awareness campaign didn’t take place due to the General Elections, which has had a major negative impact on the outbreak
- Poor Healthcare Facilities: Many of the deaths could have been averted if there had been better health infrastructure. For example, at the Sri Krishna Medical College and Hospital (SKMCH), where most of the deaths occurred, there are not enough beds in the ICU, shortage of staff and equipment, as well as frequent power cuts. Importantly, there is also an acute shortage of dextrose solution, which is life-saving in cases of hypoglycemic encephalopathy
- Shortage of Doctors: Although the World Health Organization (WHO) recommends 1 doctor per 1,000 patients, the Indian average is 1 doctor per 11,082 patients, whereas in Bihar this stands at 1 doctor per 28,391 patients – the worst in India!
- Lack of Awareness: There is a lack of awareness among parents about the importance of balanced diets and general hygiene in disease prevention. This primarily arises from being illiterate
- Misinformation: A lot of confusion has been created due to the spread of misinformation about the outbreak among the families of the affected children, which has led to a public outcry
Should Economic Losses be Equated to Lives Lost?
In the midst of this grave human tragedy, there is talk of the loss to the litchi industry in Bihar. Market experts have estimated that the industry has suffered almost INR 1 billion in revenue this season, with litchi prices falling below 50 percent. They have also indicated that some countries like USA, UK, Australia, United Arab Emirates (UAE), and New Zealand have temporarily stopped importing litchi juice from India. However, it should be noted that financial losses are not permanent and can be recovered once again, but the loss of human lives is permanent, which cannot be brought back. Hence, it is rather inhuman to talk of economic losses when human lives are at stake.Conclusion
From the foregoing discussion, it is evident that there is a direct link between AES and litchis, as it is the toxins present in this fruit that are directly responsible for precipitating the condition. Nevertheless, there are also many other factors that indirectly contribute to the problem, with litchi merely acting as a trigger.References:
- Narain JP, Dhariwal AC, MacIntyre CR. Acute Encephalitis in India: An Unfolding Tragedy. Indian J Med Res. 2017; 145(5): 584-7 - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5644291/)
- Shrivastava A, Kumar A, Thomas JD, Laserson KF, Bhushan G, Carter MD, et al. Association of Acute Toxic Encephalopathy with Litchi Consumption in an Outbreak in Muzaffarpur, India, 2014: A Case-Control Study. Lancet Glob Health. 2017; 5(4): e458-66. - (http://dx.doi.org/10.1016/S2214-109X(17)30035-9)
- Ghosh S, Basu A. Acute Encephalitis Syndrome in India: The Changing Scenario. Ann Neurosci. 2016; 23(3): 131-3. - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5043220/)
- Asthana S, Dixit S, Srivastava A, Kumar A, Singh SP, Tripathi A, et al. Methylene Cyclopropyl Glycine, Not Pesticide Exposure as the Primary Etiological Factor Underlying Hypoglycemic Encephalopathy in Muzaffarpur, India. Toxicol Lett. 2019; 301: 34-41.- (https://www.sciencedirect.com/science/article/pii/S0378427418320423?via%3Dihub)
- Islam MS, Sharif AR, Sazzad HMS, Khan AKMD, Hasan M, Akter S, et al. Outbreak of Sudden Death with Acute Encephalitis Syndrome Among Children Associated with Exposure to Lychee Orchards in Northern Bangladesh, 2012. Am J Trop Med Hyg. 2017; 97(3): 949-57. - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5590581/)
- Paireau J, Tuan NH, Lefrançois R, Buckwalter MR, Nghia ND, Hien NT, et al. Litchi-associated Acute Encephalitis in Children, Northern Vietnam, 2004-2009. Emerg Infect Dis. 2012; 18(11): 1817-24. - (https://dx.doi.org/10.3201/eid1811.111761)
- Spencer PS, Palmer VS. The Enigma of Litchi Toxicity: An Emerging Health Concern in Southern Asia. Lancet Glob Health. 2017; 5(4): e383-4. - (http://dx.doi.org/10.1016/S2214-109X(17)30046-3)
- National Health Profile 2018 - Central Bureau of Health Intelligence, Ministry of Health & Family Welfare, Government of India - (https://www.cbhidghs.nic.in/index1.php?lang=1&level=2&sublinkid=88&lid=1138)
Source-Medindia
 MEDINDIA
MEDINDIA





 Email
Email