- Nipah virus infection - World Health Organization (2018) - (http://www.who.int/csr/disease/nipah/en/)
- Nipah virus - Centers for Disease Control and Prevention - (https://www.cdc.gov/vhf/nipah/pdf/factsheet.pdf)
- Nipah R&D - World Health Organization (2018) - (http://www.who.int/blueprint/priority-diseases/key-action/nipah/en/)
- Nipah virus outbreaks in the WHO South-East Asia Region - World Health Organization (2018) - (http://www.searo.who.int/entity/emerging_diseases/links/nipah_virus_outbreaks_sear/en/)
What is Nipah Virus (NiV) / Hendra Virus?
Nipah Virus (NiV) derives its name from a village called Kampung Sungai Nipah in Malaysia, where it was first isolated from an infected person in 1998, who succumbed to the infection. NiV is an RNA (ribonucleic acid) virus, belonging to the Family Paramyxoviridae and Genus Henipavirus. NiV is closely related to the Hendra virus, which was previously known as Equine morbillivirus. This virus causes pneumonia and acute respiratory infection in horses as well as humans and has been reported mainly from Australia.
NiV infection, also known as NiV encephalitis, is an important emerging viral zoonotic disease that affects both humans and animals. NiV is spread by fruit bats (also known as ‘flying foxes’), which belong to the Family Pteropodidae and Genus Pteropus. These bats are the natural reservoir host of NiV. Currently, NiV encephalitis is on the WHO list of Blueprint priority diseases.
History and Origin of Nipah Virus
History of Nipah Virus
The history of NiV goes back to the year 1998, when the first outbreak of NiV occurred in peninsular Malaysia during the period between September 1998 and April 1999. A total of 265 cases of NiV encephalitis were reported from Malaysia, among those who had close contact with infected pigs or had physical contact with NiV infected patients. Importantly, the disease has devastating zoonotic potential, which is reflected by the fact that over 1 million pigs were culled and destroyed to control the disease in Malaysia, causing huge economic losses and adverse social disruption. In March 1999, 11 abattoir workers in Singapore became infected after handling imported pigs from Malaysia. It is interesting to note that NiV infections can cause high mortality, such as in the Malaysian outbreak, or low mortality as in the Singapore outbreak where the abattoir workers primarily presented with neurological complications and pneumonia. Since May 1999, no new NiV outbreaks have been reported from Malaysia and Singapore till date. However, evidence of the virus, without clinical disease, has been found in fruit bats in Madagascar, Cambodia, Thailand, Timor-Leste, and Indonesia.
Origin of Nipah Virus
Since there have been no reports of circulation of NiV prior to 1998, scientists have hypothesized that the virus remained largely within the fruit bat population in the tropical forests of Malaysia. However, due to mass deforestation activities to develop settlements, farming and rearing of domestic animals including pigs for food production, the natural habitat of the fruit bats was encroached by humans. Consequently, pigs became infected with NiV from the urine and feces of these bats. The virus replicated rapidly within the pigs, as a result of which the virus became amplified and eventually spilled-over to the farmers rearing the pigs, who become infected by animal to human transmission. Eventually, more and more people became infected by human-to-human transmission and when it reached the “tipping-point”, the explosive Malaysian outbreak occurred.
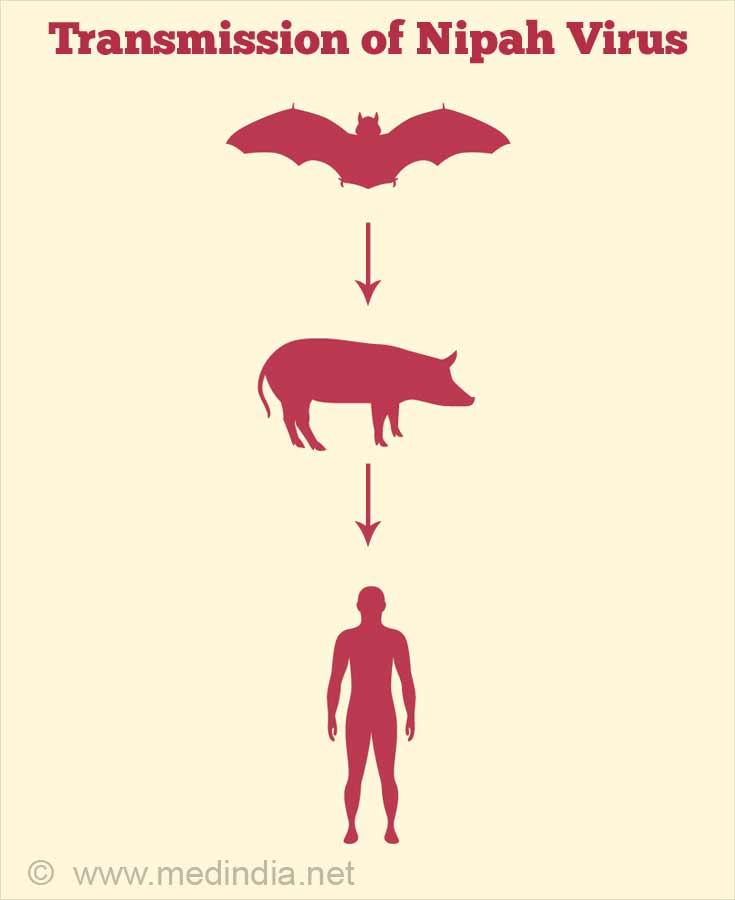
Transmission of Nipah Virus
Nipah virus is carried by fruit bats, which are the natural reservoir hosts. The virus is present in bat urine, feces, and saliva. It has been reported that fruit bats can infect date palm sap, while being extracted from palm trees. Upon consumption of raw sap, the infection can spread to humans. Likewise, fruits bitten by fruit bats can become infected, which upon consumption can cause NiV infection in humans.
The intermediate hosts are usually pigs. Infected pigs can infect other pigs as well as domestic animals. This is an example of animal-to-animal transmission. Infected pigs can also transmit the disease to humans, especially to pig handlers or through consumption of pork. This is called animal-to-human transmission.
Importantly, the disease can also be spread between humans by nasal discharges and other body fluids. The virus can also be transmitted via fomites such as clothing, equipment and shoes. This transmission between humans is called human-to-human transmission.
What Causes Nipah Virus Infection?
NiV infections can be caused by various factors. These are briefly highlighted below:
- Close contact with the excretions and secretions of individuals potentially infected with the virus.
- Consumption of partially-eaten fruits by bats.
- Undercooked meat of infected animals.
- Drinking of raw date palm sap/juice/toddy, which may be infected.
- Uncovered containers used for collecting raw date palm sap can potentially cause NiV infection if the contents become infected by fruit bats.
What are the Symptoms & Signs of Nipah Virus Infection?
The initial presentation of NiV infection is non-specific. It is characterized by sudden onset of fever, often called ‘brain fever ’. This is accompanied by headache, drowsiness, nausea and vomiting. The patient can also experience photophobia (an aversion for sunlight). Neck rigidity and severe muscle pain/spasm can also occur. The patient’s condition deteriorates rapidly and is accompanied by mental confusion and disorientation, often leading to coma within a couple of days. In the absence of prompt supportive care, the patient may die.

What are the Consequences of Nipah Virus Infection?
The consequences of NiV infection can be very grave. Serious complications such as encephalitis, associated with ‘brain fever’ can occur, where there is inflammation of the brain. When these complications occur, control of NiV replication is not possible. A consequence of this is altered consciousness, sometimes even causing the patient to become unconscious. In very severe cases, the patient can slip into coma within a matter of 24 to 48 hours. The ultimate consequence of this is death!
How can you Diagnose Nipah Virus Infection?
The disease is very difficult to diagnose based on clinical symptoms alone. However, a definitive diagnosis can be made based on laboratory tests, which are briefly highlighted below:
ELISA: “ELISA” stands for “Enzyme-linked Immunosorbent Assay”. It is a very accurate and sensitive immunological test for detecting antigens or antibodies, depending upon the format of the ELISA technique used.
In case for NiV infection, antibodies will be generated against the virus surface proteins (antigens). These antibodies circulate within the patient’s blood. So, a small sample of blood can be used for detecting as well as quantifying the level of virus-specific antibodies in the patient’s body using the ELISA test. The level of these antibodies is technically termed as “titer”, which gives an idea of the amount of virus present in the body – the higher the titer, the higher the severity of the disease.
RT-PCR: “RT-PCR” stands for “Reverse Transcription-Polymerase Chain Reaction”. This is one of the most sensitive molecular tests currently available for detection of viral infections. Since NiV has an RNA genome, a minute sample of blood is taken from the patient, which will contain the viral RNA.
The RNA is unstable, so it has to be converted to DNA, which is more stable. This is done by “reverse transcription” of the RNA to produce complementary DNA (cDNA), which is subsequently amplified by PCR using a thermocycler to generate millions of copies of the DNA from even a single strand of DNA molecule. This DNA is quantified by a procedure called ‘agarose-gel electrophoresis’. A positive test indicates that virus is definitely present in the patient’s body.
In any outbreak situation, these tests are generally carried out at the National Institute of Virology, Pune, which is the National Reference Laboratory for viral diseases in India.
How can you Treat Nipah Virus Infection?
These is no specific treatment for Nipah virus infection. Primary treatment involves intensive supportive care with continuous monitoring. The drug ribavirin has been shown to be effective against viruses in in vitro studies. However, its effectiveness in human clinical trials remains inconclusive and therefore lacks clinical applicability.
There is currently no vaccine available for preventing NiV infections. However, recent research has indicated that a subunit protein vaccine, using the Hendra virus G protein, produces cross-protective antibodies against Hendra virus as well as NiV. This experimental vaccine has been recently used in Australia to protect horses against Hendra virus infection. Importantly, this vaccine also has a great potential for protecting humans against NiV infection.
How can you Prevent Nipah Virus Infection?
You can prevent NiV infection by taking the following precautions:
- Avoid contact with sick people, infected animals such as pigs and horses, as well as the natural host, namely, the fruit bat.
- Do not drink raw date palm sap or toddy.
- Use netting on the opening of containers used to collect date palm sap, so that the fruit bats cannot cause contamination.
- Maintain personal hygiene and hand washing practices.
- Do not consume raw fruits.
- Eat cooked, homemade food until the outbreak passes away.
- Use personal protective equipment (PPE) like goggles, head covering and masks e.g. N95 mask while traveling and working in public areas to reduce the chances of human-to-human transmission.
- Immediately report to the nearest health facility if you develop symptoms of NiV infection.

Nipah Virus Outbreaks
Malaysia Outbreak: It is the first outbreak of Nipah in the world (discussed above). The disease was primarily spread by infected pigs. Besides pigs there is evidence of NiV infection in several species of domestic animals, including dogs, cats, goats, horses, and possibly also sheep. However, following the initial Nipah outbreaks, the virus has primarily affected human populations around the globe.
Meherpur (Bangladesh) Outbreak: NiV was isolated during an outbreak in April-May 2001 in Meherpur district of Bangladesh. In this Bangladesh outbreak, there were 13 cases and 9 deaths, with a case fatality rate of 69%. Since then, NiV encephalitis has been reported almost every year in many districts in Bangladesh.
Siliguri (West Bengal, India) Outbreak: The Siliguri outbreak is the first Nipah outbteak on Indian soil. It occurred from January to February in 2001. The patients presented with fever and neurological symptoms. Blood samples were obtained from the patients and analyzed by ELISA and RT-PCR. NiV-specific antibodies were detected in 9 out of 18 patients by ELISA. RT-PCR detected viral RNA in 5 patients. In this outbreak, there were 66 cases and 45 deaths, with a case fatality rate of 68%.
Nadia (West Bengal, India) Outbreak: This is the second Indian outbreak, which occurred in Nadia district of West Bengal. In this outbreak 30 patients initially presented with febrile illness, of which 5 were confirmed as Nipah cases. All 5 cases proved to be fatal. All the fatal cases tested positive for NiV by RT-PCR. Therefore, the case fatality rate in this outbreak was 100%.
Important Details in Nipah Outbreaks:
- In the outbreaks reported in Bangladesh and India, so far 263 NiV encephalitis cases and 196 deaths have been reported since 2001. NiV encephalitis exhibits a case fatality rate of 0-100%, with an average case fatality rate of 74.5%.
- In the Bangladesh and Indian outbreaks, there was no involvement of pigs in the transmission of NiV infection, unlike the Malaysian outbreak. Consumption of raw date palm sap infected by fruit bats was the primary cause of the spread of NiV.
Kozhikode (Kerala, India) Outbreak: This is the third outbreak to occur in India and is currently ongoing in Kozhikode district in Kerala. Of the 20 patients who had presented with symptoms of NiV infection, 12 have so far died, including a nurse who got infected while treating patients.
The Kerala government has assured the public that it is safe to travel to Kerala, but has nevertheless issued a travel advisory to preferably avoid 4 districts in Kerala, namely, Kozhikode, Malappuram, Wayanad and Kannur.
It is believed that the virus has the potential to spread to other states. One case of Nipah has already been detected from Mangalore in Karnataka, which has stepped-up surveillance and case detection efforts in the state as well as the neighboring states of Telangana and Tamil Nadu.
Experts from the National Center for Disease Control (NCDC), New Delhi and the All India Institute of Medical Sciences (AIIMS), New Delhi are currently in Kozhikode to assess the situation. The outbreak is presently under control and the Union Health Ministry has urged citizens to remain calm and not to panic.
 MEDINDIA
MEDINDIA

 Email
Email