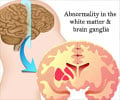
Study identifies mutations in many other genes that could possibly contribute to trimethylaminuria.

- Mutations in a single gene, FM03, has been atrributed to the cause of trimethylaminuria (TMAU), which is characterized by fish-like odor symptoms.
- But some people who report fish-like odor symptoms, do not have severely disruptive mutations in the FMO3 gene.
- New study has found that mutations in genes other than FMO3 may contribute to TMAU.
TOP INSIGHT
The new genes that have been identified to contribute to trimethylaminuria, may help in better understanding of the underlying biology of the disorder and perhaps even identify treatments.
"Our findings may bring some reassurance to people who report fish-like odor symptoms but do not have mutations in the FMO3 gene," said Monell behavioral geneticist Danielle R. Reed, PhD, a senior author on the study.
Trimethylaminuria
TMAU is classified as a rare disease that affects less than 200,000 people in the United States. However, its actual incidence remains uncertain, due in part to inconclusive diagnostic techniques.
The distressing symptoms of TMAU result from the buildup of trimethylamine (TMA), a chemical compound produced naturally from many foods rich in the dietary constituent, choline. Such foods include eggs, certain legumes, wheat germ, saltwater fish and organ meats.
People with TMAU who have defects in the underlying FMO3 gene are unable to metabolize TMA, that results in accumulation of TMA, along with its associated unpleasant odor, and is excreted from the body in urine, sweat, saliva, and breath.
In some people who report having the fish odor symptoms of TMAU do not have severely disruptive mutations in the FMO3 gene which led the researchers to suspect that other genes may also contribute to the disorder.
New Study
In the new study, to identify additional genes that contribute to TMAU, the research team combined a gene sequencing technique known as exome analysis with sophisticated computer modeling.
The sensory, metabolic and genetic data from ten individuals randomly selected from 130 subjects previously evaluated for TMAU at the Monell Center was compared.
Sensory evaluation of each individual's body odor was done in the laboratory by a trained sensory panel before and after a metabolic test to measure production of TMA over 24 hours following ingestion of a set amount of choline.
None of the individuals had mal-odor during sensory evaluation.
Though the diagnosis of TMAU was confirmed by choline challenge test which revealed a high level of urinary TMA in all 10 subjects, genetic analyses revealed that the FMO3 gene appeared to be normal in four of the 10 individuals.
On the other hand, defects in several other genes were detected, that could also hamper the ability to metabolize the odorous TMA.
"We now know that genes other than FMO3 may contribute to TMAU. These new genes may help us better understand the underlying biology of the disorder and perhaps even identify treatments," said Reed.
Conclusion
Monell analytical organic chemist George Preti, PhD, also a senior author, commented on the diagnostic implications of the combined findings, "Regardless of either the current sensory presentation TMAU or the FMO3 genetics, the choline challenge test will confirm the accumulation of TMA that reveals the presence of the disorder."
Researchers would like to repeat the genetic analyses in a larger cohort of TMAU patients without FMO3 mutations to confirm which other genes are involved in the disorder.
"Such information may identify additional odorants produced by TMAU-positive patients, and inform the future development of gene-based therapies" said Preti.
The study is published in the open access journal BMC Medical Genetic.
Reference
- Danielle R. Reed et al. Genetic analysis of impaired trimethylamine metabolism using whole exome sequencing. BMC Medical Genetic; (2017) DOI: 10.1186/s12881-017-0369-8
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email