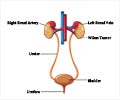
What is Nephrectomy?
Nephrectomy or kidney removal surgery is a procedure where the entire kidney or a part is surgically removed.
Surgical Anatomy of the Kidney: The kidneys are paired, bean-shaped organs that are located on either side of the backbone below the chest, between the 12th thoracic (T12) and 3rd lumbar (L3) vertebrae. The left kidney is normally positioned slightly higher than the right kidney. The kidneys are approximately 10-12 cm in length, 5-7 cm in width, and 2-3 cm in thickness. The adrenal or suprarenal glands are small glands located on the top of each kidney. Exteriorly, the kidneys and adrenal glands are covered by the renal fascia or Gerota’s fascia, below which is the adipose or fat capsule of the kidney. The kidney is divided into two layers – the outer cortex and the inner medulla. The renal artery, renal vein and ureter enter and leave the kidney from its medial or inner aspect called the hilum. The renal artery is a branch of the aorta while the renal vein is connected to the inferior vena cava. The urine formed by the kidney passes out through the ureter, which carries it to the urinary bladder for temporary storage prior to excretion.
What are the Types of Nephrectomy?
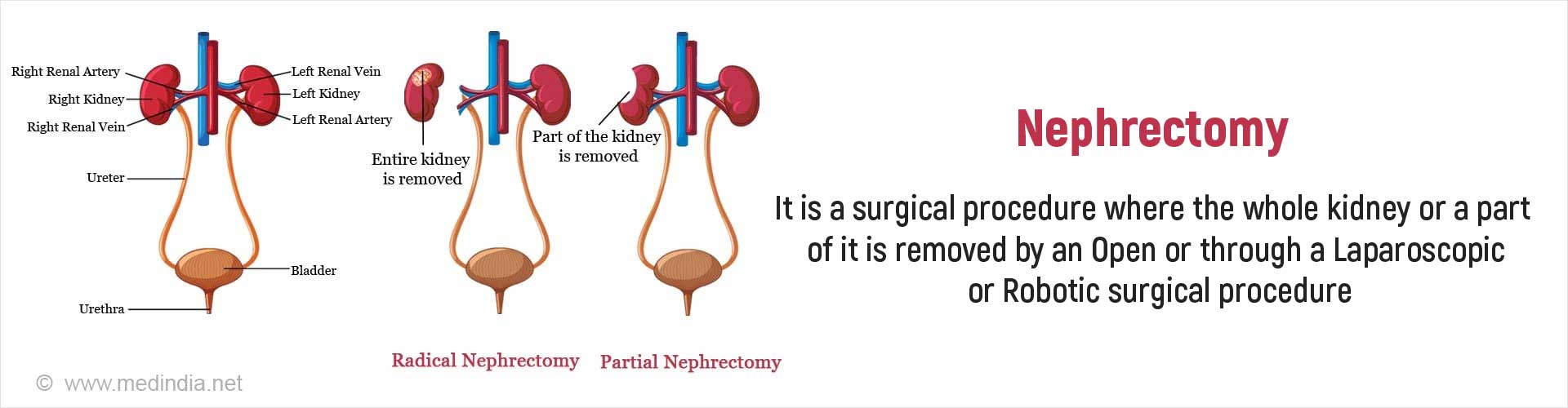
Based on the extent of removal of the kidney, nephrectomy can be of two types:
- Complete Nephrectomy: This is also known as radical nephrectomy. In this type of nephrectomy, the entire kidney is removed, along with a section of the ureter (the tube connecting the kidney to the urinary bladder), as well as the adrenal gland and the fatty tissue surrounding the kidney. When both kidneys are removed at the same time, the procedure is called bilateral nephrectomy.
- Partial Nephrectomy: In this type of nephrectomy, a part of the kidney that is diseased is surgically removed, leaving the healthy tissue intact.
Why is Nephrectomy done?
Nephrectomy is usually done for the following purposes:
- Treatment of Kidney Cancer: Cancer of the kidney such as renal cell carcinoma in adults or Wilms’ tumor in children can be treated by surgically removing the cancerous tissue either by partial or radical nephrectomy.
- Excision of Damaged or Diseased Kidney: Removal of a seriously damaged, scarred or non-functioning kidney due to traumatic injury can be carried out by radical nephrectomy. Also, diseased kidney tissue can be selectively removed by partial nephrectomy.
- Kidney Transplantation: Nephrectomy is carried out for harvesting a healthy kidney from a donor for transplantation into a patient with kidney failure. A healthy person with a good functional kidney without hypertension (high blood pressure) or diabetes or at a risk from suffering these in the future is an ideal candidate for donating a kidney to a patient who needs a transplant.

Who should not Undergo Nephrectomy? / What are the Contraindications for Nephrectomy?
Nephrectomy is contraindicated in the following conditions:
- Risk of Kidney Failure: A person who has only one healthy kidney should not be a kidney donor for transplantation purposes.
- Bleeding Disorders: If the patient has a serious bleeding disorder such as hemophilia, nephrectomy can cause severe uncontrollable bleeding. If unavoidable, the nephrectomy requires extensive planning and preparation, as well as provision for substitution therapy for the deficient coagulation factor (for example, factor IX or Christmas factor for hemophilia B). Such a surgery should only be performed by a multidisciplinary team in a comprehensive tertiary care center, which can handle any complication that may arise during the procedure.
- Decompensated Heart Failure (DHF): In this type of heart failure, there is a sudden deterioration of the pumping ability of the heart. Nephrectomy is contraindicated in patients with DHF.
- Decompensated Diabetes Mellitus: In this condition, the high blood sugar levels cannot be controlled by drugs, resulting in severe damage to the internal organs. Development of such a serious condition requires prompt medical attention. Nephrectomy is contraindicated in decompensated diabetes mellitus.
- Anticoagulation Medications: Nephrectomy is contraindicated if the patient is on blood thinners. Under such circumstances, the doctor will evaluate the condition and carefully weigh the risks (of stopping anticoagulation therapy) versus the benefits (of a nephrectomy), which could be a difficult decision to take. Based on this, the doctor will recommend when and how to discontinue the medications if he/she decides to go ahead with the surgery.
How do you Prepare Before Nephrectomy? What are the Tests Required Before Nephrectomy?
Routine Tests: Prior to nephrectomy, you will need to undergo some routine tests, which include the following:
- Urinalysis: In this test, your urine will be checked for the presence of pus cells, which indicate infection, and other abnormal constituents like glucose, protein, ketones, red blood cells and casts.
- Kidney Function Test (KFT): This blood test determines whether your kidneys are functioning optimally. The parameters that are measured include blood urea nitrogen (BUN), serum creatinine, serum electrolytes (sodium, potassium, chloride, bicarbonate), and estimated glomerular filtration rate (eGFR).
- Complete Blood Count (CBC): This blood test provides a complete blood picture. In this test, the common parameters measured include hemoglobin concentration, red blood cell (RBC) count, white blood cell (WBC) counts such as total count (TC) and differential count (DC), platelet count, and erythrocyte sedimentation rate (ESR).
- Blood Grouping, Cross-matching and Tissue Typing: Your blood group will be determined in case you require a blood transfusion. In case you are acting as a donor for transplantation, your blood will be cross-matched with that of the recipient. Tissue typing will also be done between your tissues and those of the recipient so that the tissues are compatible and there is a lesser chance of rejection of the kidney transplant.
- Coagulation Profile: You will undergo a blood test that provides information about blood clotting. The test measures parameters like the prothrombin time (PT), partial thromboplastin time (PTT), and international normalized ratio (INR).
- Chest X-ray: You will undergo a chest X-ray as part of the routine preoperative test.
- ECG (Electrocardiogram): You will undergo an ECG, which studies the electrical activity of your heart. A more detailed heart examination may be necessary if you are at an advanced age to make sure you are fit for the surgery.

Specific Tests: In addition to the above tests, you may also have to undergo some specialized tests:
- CT Scan: Computed tomography (CT) scan is very useful for the evaluation of kidney tumors. It gives accurate information about tumor size, location and signs of metastasis (spread) in cases of cancers. In this procedure, you will be asked to lie down still on a special table for a few minutes. A doughnut-shaped instrument will pass over the part to be screened, and images will be taken. A contrast dye may be injected into your vein; therefore you should inform the radiologist if you suffer from any allergies.
- MRI Scan: You may be subjected to a magnetic resonance imaging (MRI) scan if your doctor suspects a problem in the inferior vena cava (the blood vessel carrying deoxygenated blood to the heart). Magnetic resonance angiography (MRA) provides accurate images of vascular anatomy and helps in planning the surgery. In this procedure you will be placed inside a narrow tube, which can sometimes be claustrophobic, if you have a fear of enclosed spaces. The MRI machine makes loud clicking noises and it is advisable to ask for earplugs to help block these noises out.
What Happens During the Surgery?
Pre-operative Check-up: Routine tests as indicated above are ordered a few days before the surgery. Admission is required a day or two before the surgery. You will be advised to stop taking aspirin or blood thinners a few days before the procedure.
Fasting Before Surgery: Overnight fasting is required and occasionally intravenous (IV) fluid may be required to keep you well hydrated. Sedation is sometimes required for good overnight sleep before the surgery.
Type of Anesthesia: Nephrectomy is done under general anesthesia.
Shift from the Ward or Room to the Waiting Area in the Operating Room: An hour or two before the surgery, you will be shifted to the operating room waiting area on a trolley. Once the surgical room is ready, you will be shifted to the operating room.
Shift to the Operating Room: The ambiance in the operating room can sometimes be very daunting and a small amount of sedation can help overcome your anxiety. From the trolley, you will be shifted on to the operating table. As you look up, you will see the operating light console and at the head end will be the anesthesia machine. There may also be monitors to check oxygen levels, heart activity (ECG machine) and other vital parameters. A constant beeping sound may be present from the monitors, which may sometimes be irritating.
Anesthesia Before Surgery: The anesthetist will inject drugs through an IV line and make you inhale some gases through a mask that will put you in deep sleep for anesthesia. Once you are in deep sleep, a tube will be inserted into your mouth and windpipe to administer the anesthesia gases to overcome pain and keep you comfortable. A catheter will be introduced to drain your urinary bladder.
Surgery may involve a complete (radical) nephrectomy if the whole kidney is damaged or diseased. Complete nephrectomy is also carried out if you are donating your kidney for transplantation purposes. Alternatively, a partial nephrectomy is done if the kidney is partially diseased, if a tumor is confined to a particular location, or if the patient has only one kidney that functions properly.
For the actual surgical procedure, the surgeon may choose to carry out a conventional open nephrectomy or opt for a less invasive technique such as laparoscopic nephrectomy.
- Open Nephrectomy: You will be made to lie down on your side in a slightly tilted position, exposing the area where the incision is to be made. A large incision (15-25 cm) is made on the skin between the lowermost ribs. The underlying tissues are separated and the kidney is exposed. The renal blood vessels entering the kidney are tied and cut. The ureter is also tied and cut between the kidney and the urinary bladder. The kidney is removed and the incision is sutured in layers. The adrenal gland may or may not be removed. The surgery can take up to 3 hours, depending on the type of nephrectomy (complete or partial) being performed.
- Laparoscopic Nephrectomy: You will be made to lie down on your back in a comfortable position. Four small incisions will be made in your abdomen through which an instrument called a laparoscope, with a video camera at its lower end, and surgical tools are inserted for viewing and excising the kidney respectively. The surgery is performed with the help of a video monitor. Carbon dioxide is pumped to inflate the abdominal cavity so that the images of the kidney appear clear and distinct. After the kidney is excised, it is pulled out through a fifth incision, approximately 8 cm wide, in the front of the abdominal wall below the navel. Some advantages of the laparoscopic surgery are that it promotes faster recovery, shorter hospital stays, and less post-operative pain.
Robotic surgery is sometimes performed, wherein the surgeon sits at the console and guides the robotic arms of the machine to carry out the surgery with precision.
What Happens after the Nephrectomy?
Waking up from Anesthesia: Once the surgery is over, you will wake up and the tube down the wind pipe will be removed. You will be asked to open your eyes before the tube is removed. You will be sedated and the voice of the anesthetist may be faint. Once the tube is out, you may have cough and sometimes nausea.
There may be a tube going into the stomach called a nasogastric or Ryle’s tube to keep it empty. There will also be an IV line and a catheter that drains your urinary bladder. You will remain on oxygen. Once fully awake, you will be shifted on the trolley and taken to the recovery room.
Recovery after Nephrectomy
Recovery Room: In the recovery room, a nurse will monitor your vitals and observe you for an hour or two before shifting you to the ward or your room. Painkillers may be prescribed depending on the extent of the pain.
Post-operative Recovery: You will remain in the hospital for a few days following the procedure. Normally, on the first day, you will not be allowed much to drink or eat. Once your bowels start recovering, you will be given fluids and a light diet. This may take one to three days.
Change of dressing will be done as required. The IV lines for fluids and drugs will continue for a few days till you start eating normally.
Chest physiotherapy may be started after 24 hours to prevent chest infection.
DVT Prophylaxis: Early movement of your legs and some mobilization prevents DVT or deep vein thrombosis, where a clot is formed in the deep veins of the legs. The clot can travel up to the lungs and even be fatal. Other measures like small dose of heparin and special stockings may also be used.
What are the Risks & Complications of Nephrectomy?
Short-term complications of nephrectomy include the following:
- Infections
- Bleeding or hemorrhage
- Post-operative pneumonia
Long-term complications of nephrectomy generally arise from the absence of two functional kidneys. Although one kidney is sufficient for leading a healthy life, the functional capacity decreases appreciably. There are two major long-term risks and complications of nephrectomy:
- Hypertension (high blood pressure)
- Chronic kidney disease (CKD)
It is therefore necessary to check for your kidney function on a regular basis if you have undergone nephrectomy for one kidney.
 MEDINDIA
MEDINDIA
 Email
Email