- Christianson AL, Howson CP, Modell B. White Plains. New York, USA: March of Dimes Birth Defects Foundation; 2006. [Last accessed on 2016 Oct 7]. March of dimes global report on birth defects: The hidden toll of dying and disabled children. Available from: http://www.marchofdimes.com.
- Updated National Birth Prevalence Estimates for Selected Birth Defects in the United States, 2004-2006 - (http://www.cdc.gov/ncbddd/birthdefects/features/birthdefects-keyfindings.html)
- What are Birth Defects? - (http://www.cdc.gov/ncbddd/birthdefects/facts.html)
- Sharma R. Birth defects in India: Hidden truth, need for urgent attention. Indian J Hum Genet. 2013 Apr-Jun; 19(2): 125–129.
- Birth defects SIXTY-THIRD WORLD HEALTH ASSEMBLY 1 April 2010.
- What are the types of birth defects? - (https://www.nichd.nih.gov/health/topics/birthdefects/conditioninfo/pages/types.aspx)
- Birth defect - (https://en.wikipedia.org/wiki/congenital_disorder)
- Obican SG,, Jahnke GD, Soldin OP, and Scialli AR. Teratology Public Affairs Committee Position Paper: Iodine Deficiency in Pregnancy. Birth Defects Res A Clin Mol Teratol. 2012 Sep; 94(9): 677-682.
- Parker SE, Mai CT, Canfield MA, Rickard R, Wang Y, Meyer RE, Anderson P, Mason CA, Collins JS, Kirby RS, and Correa A. Updated National Birth Prevalence Estimates for Selected Birth Defects in the United States, 2004–2006. Birth Defects Research (Part A) 88:10.
- Pregnancy care - (https://medlineplus.gov/ency/article/007214.htm)
- Intellectual disability - (https://en.wikipedia.org/wiki/intellectual_disability #signs_and_symptoms)
- Liu S, Joseph KS, Lisonkova S, Rouleau J, Van den Hof M, Sauve R, Kramer MS; Association between maternal chronic conditions and congenital heart defects: a population-based cohort study. Circulation. 2013 Aug 6;128(6):583-9.
- Lobo I. (2008) Birth Defects: Prevention and Treatment. Nature Education 1(1):19.
- GBD 2013 Mortality and Causes of Death, Collaborators (17 December 2014)."Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013." Lancet. 385 (9963): p117-171.
What are Birth Defects?
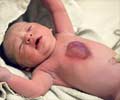
Birth defects are abnormalities that occur in babies which affect how the body looks, works or both. They usually happen during the first three months of pregnancy. They can be identified prenatally, at the time of birth or later in infancy.
Birth defects are also called congenital anomalies, congenital disorders or congenital malformations. They can cause long-term disabilities and have a significant impact on the affected individuals, their families, the society in general and health-care systems. They sometimes impact the survival of the child.
The risk of having a child with a birth defect continues to be significant. Individuals of all age groups, races, education levels and socio-economic backgrounds are affected by birth defects. The most common severe congenital defects are Down’s syndrome, neural tube defects and congenital heart defects. Teratology is the branch of medicine that specializes in the study of congenital defects.
Some important facts of birth defects are:
- 7.9 million births with serious birth defects due to genetic or partial genetic cause occur every year, according to the March of Dimes (MOD) Global Report on Birth Defects published in 2006.
- Among those born with some kind of congenital birth defect, 303,000 die within 4 weeks of life every year worldwide.
- Birth defects account for 7% of all neonatal mortality and 3.3 million deaths that occur in children under five years of age every year.
- 94% of severe congenital anomalies occur in low and middle-income countries possibly due to lack of nutritious foods, infections and lack of proper healthcare and screening tests.
- Congenital heart disease and neural tube defects are common causes of deaths due to birth defects.
- The first-ever World Birth Defects day was observed on 3 March, 2015 to create awareness of birth defects.
- The prevalence of birth defects in India is between 61 and 69.9 per 1000 live births.
It is a general notion that birth defects are a lifelong liability. Though this may be true in some cases, the truth is that many of the birth defects can be treated successfully. Some of them can even be prevented by appropriate protective measures.
What are the Types of Birth Defects?
Birth defects are mostly classified into two types - Structural and Functional.
- Structural birth defects are those that affect the development of body parts like the skeleton and certain organs. Examples are neural tube defects and congenital heart defects.
- Functional or Developmental Birth Defects affect how a body part functions or works. They often lead to intellectual and developmental disability (IDD). They include:
- Nervous disorders like Down’s syndrome and other chromosomal disorders, speech and movement disabilities, behavioral problems.
- Sensory problems like blindness and deafness.
- Metabolic disorders like Phenylketonuria (increased blood levels of phenylalanine which cause intellectual disability) and hypothyroidism (underactive thyroid that interferes with brain development).
- Degenerative disorders like Muscular dystrophy (muscle weakness) and X-linked Adrenoleukodystrophy (condition where the myelin covering of the brain is affected).
The type of birth defect and the cases per birth in the United States, 2004-2006 estimated by the CDC and National Birth Defect Project are as follows:
| Birth Defect | Description of the Condition | Cases per births |
| Central Nervous System Defects | ||
| Anencephaly | Absence of most part of head and brain. | 1 in 4859 |
| Spina bifida without Anencephaly | Gap in the backbone | 1 in 2858 |
| Encephalocele | Sac-like protrusion of the brain and its surrounding membranes through an opening in the skull. | 1 in 12235 |
| Other Nervous System Defects | ||
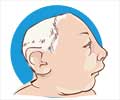
| Craniosynostosis | Early closure of head sutures. | 1 in 2500 |
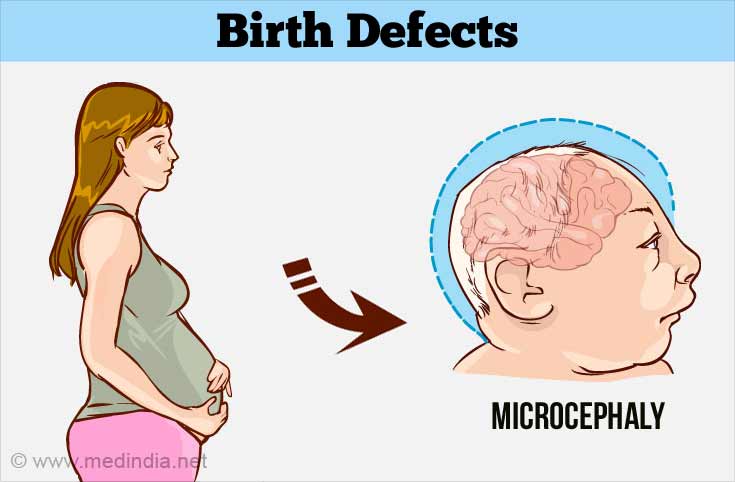
| Microcephaly | Small head size. | 1 in 1428 |
| Facial defects | ||
| Anopthalmia / Micropthalmia | Anopthalmia - Absence of one or both eyes. Micropthalmia - Small eye/eyes. | 1 in 5349 |
| Cardiovascular defects | ||
| Common truncus | Only a single common blood vessel comes out of the heart, instead of two - the main pulmonary artery and aorta. | 1 in 13876 |
| Transposition of great arteries | The main pulmonary artery and the aorta that carry blood out of the heart are switched in position or “transposed.” | 1 in 3333 |
| Tetralogy of Fallot | Four simultaneous heart defects that affect the blood flow through the heart. | 1 in 2518 |
| Atrioventricular septal defect | Presence of hole in the partition between the right and left chambers of the heart. | 1 in 2122 |
| Hypoplastic left heart syndrome | Underdeveloped left side of the heart. | 1 in 4344 |
| Orofacial defects | ||
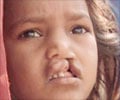
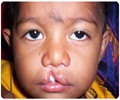
| Cleft palate without Cleft lip | Split in the roof of the mouth. | 1 in 1574 |
| Cleft lip with and without cleft palate | Split in the upper lip with or without a split in the roof of the mouth. | 1 in 940 |
| Musculoskeletal defects | ||
| Upper Limb Reduction defect | Absence of a part or a complete upper limb | 1 in 2869 |
| Lower Limb Reduction defect | Absence of a part or whole lower limb | 1 in 5949 |
| Gastroschisis | Defect in the abdominal wall with protrusion of intraabdominal organs. | 1 in 2229 |
| Omphalocele | Protrusion of abdominal organs from a hernia in the belly button region. | 1 in 5386 |
| Chromosomal Anomalies | ||
| Trisomy 13 | A full extra copy or a partial copy of chromosome number 13 that causes multiple and complex organ disorders | 1 in 7906 |
| Trisomy 21 (Down’s Syndrome) | An extra chromosome (chromosome 21) in babies that changes how they develop physically and mentally. | 1 in 691 |
| Trisomy 18 | An extra full or a partial copy of chromosome number 18 in babies that causes them to have a small head and heart defects. | 1 in 3762 |
What are the Main Causes of Birth Defects?
The main causes of birth defects include the following:
- Genetic factors like Chromosomal Disorders, Single Gene Defects and Multiple Gene Defects
- Consanguinity (when parents are related by blood) can cause rare genetic anomalies
- Advanced maternal age is a risk factor to get a child with Down’s syndrome

- Micronutrient Deficiencies
- Lack of Folic acid in pregnant women causes neural tube disorders.
- Lack of iodine in pregnant women causes maternal hypothyroidism that results in “cretinism” in babies characterized by mental retardation, dwarfed stature, bone dystrophy, and a low basal metabolism.
- Maternal Infections
- Rubella or German measles can cause abnormalities of the eye, inner ear and heart.
- Exposure to Zika virus has been linked to having a child with microcephaly.
- Maternal Alcohol consumption has been linked to craniofacial abnormalities, brain damage, intellectual disability, heart disease, kidney abnormality, skeletal anomalies and eye defects
- Exposure to Toxic Substances including certain medications and environmental chemicals. Substances that can cause birth defects are called teratogens.
- Isotretinoin used to treat severe acne can cause serious birth defects
- Vitamin A when consumed above 700 μg/day is a teratogen
- Trimethadione causes fetal trimethadione syndrome manifested as craniofacial, cardiovascular, kidney and spine malformations, as well as mental and physical developmental delay
- Valproate has anti-folate effects and can lead to neural tube closure-related defects
- Nitrate in drinking water causes CNS (Central Nervous System) disorders, musculoskeletal and heart defects
- Inhalation of carbon monoxide as first-hand or second-hand smoking causes stunted growth in babies
- Chronic Maternal Illness - There is an increased risk of congenital heart disease in the children borne by women having chronic medical conditions like diabetes mellitus, hypertension, connective tissue disorders and congenital heart disease.
- Exposure to High doses of Radiation can have an effect on the offspring like was seen after the Hiroshima attack
- Multifactorial or Unknown Causes - A combination of factors like genetics and environmental may be responsible where a single cause cannot be pinpointed. The specific cause for 50 % of birth defects is always difficult to identify
How are Birth Defects Diagnosed?
Prenatal tests refer to the use of tests for the diagnosis of certain birth defects before the child is born.
Screening Tests:
Towards the end of the first trimester between the 11th and the 13th week, two screening tests are done to check for chromosomal disorders.
- Maternal Blood Screen: This is a blood test that indicates a birth disorder if the levels of two proteins - human chorionic gonadotropin (hCG) and pregnancy associated plasma protein A (PAPP-A) – are abnormally low or high.
- Ultrasound: An ultrasound done in the first trimester is also called nuchal translucency screening. It measures the fluid at the back of the fetus’ neck. An abnormal reading indicates a chromosomal disorder or a physical defect of the heart.

During the second semester between the 15th and the 20 weeks, two screening tests are performed.
- Maternal Serum Screen: It is a simple blood test to check for neural tube defects and Down’s syndrome.
Depending on the number of proteins tested, it could also be called a r a “quad screen” (that tests the levels of 4 proteins alpha-fetoprotein, hCG, estriol, and inhibin-A.) or a “triple screen” (that tests for alpha-fetoprotein, hCG and estriol).
- Anomaly Ultrasound: A comprehensive ultrasound is done to check for structural anomalies (major physical defects in the brain and spine, facial features, abdomen, heart and limbs) as well as the size of the baby.
Diagnostic Tests:
Diagnostic tests are indicated in pregnant women with elevated levels of α -fetoprotein or other abnormal results on screening tests to confirm the possible diagnosis of a birth defect.
These tests may also be done:
- If the pregnant woman is above 35 years old
- Has had an earlier pregnancy affected by a birth defect
- Has a chronic disease like high blood pressure, diabetes, lupus or epilepsy
High Level Ultrasound or Level 2 Ultrasound: This ultrasound is done between 18 and 22 weeks of pregnancy to look more in detail for any sign of birth defects indicated in the screening tests.
Chorionic Villus Sampling (CVS): This is a diagnostic test done between 10 and 12 weeks of pregnancy for women having abnormal screening test in the first trimester. A tiny sample of the placenta, known as the chorionic villus is tested for chromosomal disorders.
Amniocentesis: Amniocentesis is done between 15 and 18 weeks of pregnancy. A sample of amniotic fluid, (the fluid which surrounds the baby), is obtained and analyzed for the following:
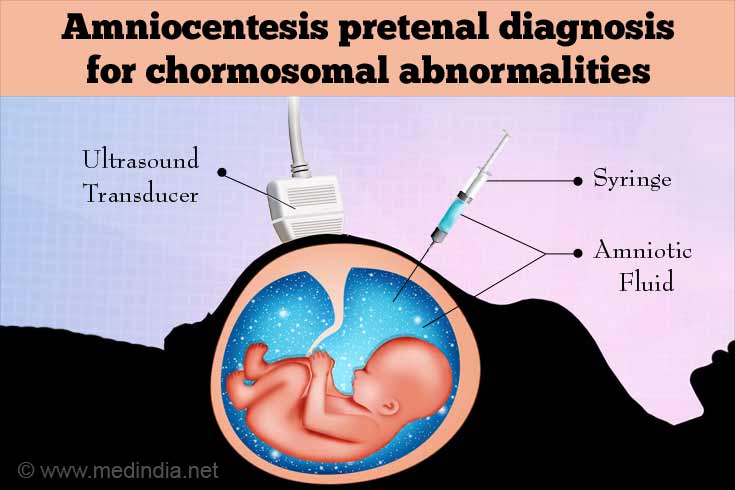
- Alpha-fetoprotein or AFP: The chemical α-fetoprotein is produced by the fetal liver but its function is unknown. It could be the fetal form of serum albumin.
Small amounts of α- fetoprotein are present in the amniotic fluid of normal fetuses. Higher than normal levels in the amniotic fluid indicates an opening in the tissue, such as a neural tube defect (spina bifida or anencephaly) or a body wall defect, such as omphalocele or gastroschisis.
However, a high level of α- fetoprotein does not always mean that the fetus is defective, because other reasons could be responsible for the same.
- Acetylcholinesterase or AChE: The presence of the enzyme acetylcholinesterase in the amniotic fluid indicates an opening in the neural tube.
Sometimes, birth defects are not diagnosed during pregnancy. Many of them are diagnosed at the time of delivery. Some congenital heart defects may be diagnosed only later in life.
What are the Pregnancy Care and Preventive Methods to be taken to Avoid Birth Defects?
- Take 400 micrograms of Folic acid every day to prevent neural tube disorders.
- A minimum dose of 250 microgram of iodine must be consumed through food and supplements daily during pregnancy to prevent maternal hypothyroidism.
- It is very important to visit your doctor on a regular basis. The number of visits depends on the trimester. Prenatal care has to be started as soon as you find out you are pregnant.
- Avoid alcohol at any point of time and at any dose during pregnancy. Alcohol consumption by pregnant women causes miscarriages, stillbirth and a wide range of physical, behavioral and intellectual disabilities collectively known as fetal alcohol spectrum disorders or FASDs.

- Avoid smoking during any point in the pregnancy as it can lead to preterm births and children with cleft lip or cleft palate.
- Avoid marijuana and other drugs strictly as they can have huge consequences on the baby.
- Keep infections at bay by washing hands regularly, cooking meat well and staying away from people with infections. Make sure that you are up-to-date with your vaccinations well before you plan to become pregnant.
- Keep diabetes under control during pregnancy.
- Maintain a healthy weight during pregnancy. Obese women tend to have complications during pregnancy and delivery
- Medications should be taken during pregnancy only after consultation with your doctor to find out if there is any link between them and birth defects.
- Vaccines that are safe to be taken during pregnancy can help prevent infections thus keeping the baby healthy as well. Some vaccines like the flu vaccine and the T dap vaccine (adult tetanus, diphtheria and acellular pertussis vaccine) are specifically recommended during pregnancy.
How are Birth Defects Treated?
Some birth defects can be treated on the birth of the baby or even prior to birth, while others may need lifelong treatment and rehabilitation. An examination of the baby at birth and certain tests give an understanding of any genetic, hematological, metabolic and hormonal disorders present.
- A congenital hearing impairment results in a hearing loss that might not surface until the child is two years old. Early diagnosis that leads to early intervention can help with the delayed speech and language development that usually occurs with the loss.
- If early diagnosis detects the presence of phenylketonuria (an inherited disorder resulting in high levels of phenylalanine in the blood), treatment in the form of a diet low in phenylalanine and high in tyrosine (precursor of phenylalanine) can be started at birth.
- Surgery is possible prenatally for some conditions like cleft lip and palate, spina bifida, heart and renal-tract defects. This limits long-term damage and allows early correction for a better developmental prognosis.
 MEDINDIA
MEDINDIA
 Email
Email