- Stevens-Johnson Syndrome - (http://sjsupport.org/)
- Stevens–Johnson syndrome / toxic epidermal necrolysis - (http://www.dermnetnz.org/topics/stevens-johnson-syndrome-toxic-epidermal-necrolysis/)
- What is Stevens Johnson Syndrome? - (http://www.skinassn.org/what-is-stevens-johnson-syndrome.html)
- National Drug Code Directory mobile app launches - (https://www.fda.gov/drugs/default.htm)
What is Stevens-Johnson Syndrome?
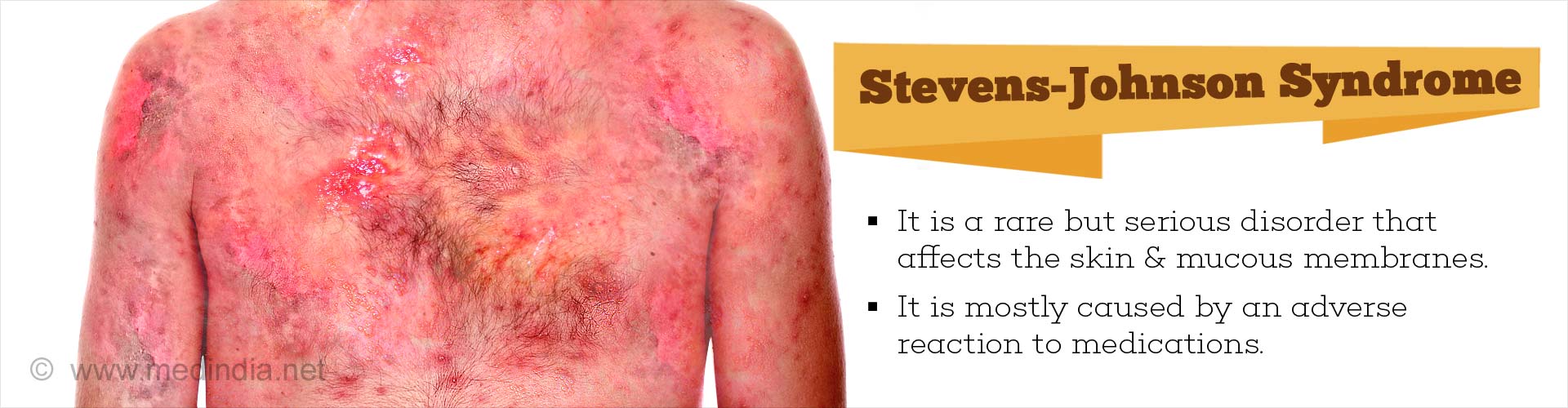
Stevens-Johnson syndrome (SJS) is a rare but serious disorder that affects the skin and mucous membranes. It is an overreaction of the body’s immune system to a trigger like a medication or sometimes a mild infection. It was named after the pediatricians A.M. Stevens and S.C. Johnson who diagnosed a child with a severe eye and mouth reaction to a drug in 1922.
SJS causes blistering and peeling of the skin and surfaces of the eyes, mouth, throat and genital tract. Swelling of the face, diffuse reddish or purplish rash that blisters and swollen lips covered in crusty sores are common features of Stevens-Johnson syndrome. If the eyes are affected, it may result in corneal ulcers and vision problems.
SJS is one of the most debilitating adverse drug reaction (ADR) recognized. Adverse drug reactions (ADR s) account for approximately 150,000 deaths per year in the U.S. alone, making drug reactions the fourth leading cause of death in the United States. Stevens-Johnson syndrome is rare with the overall risk of getting the syndrome being 2–6/million each year.
SJS is a medical emergency with a most severe form referred to as toxic epidermal necrolysis. The two conditions can be differentiated based on the total body surface area (TBSA) affected. SJS is comparatively less severe and encompasses 10% of TBSA. Toxic epidermal necrolysis (TEN) is the most serious form of disease and covers 30% or more of TBSA. An involvement of 10 to 30% of TBSA is referred to as overlapping Stevens-Johnson syndrome/toxic epidermal necrolysis. SJS is most common in children and the elderly. SCORTEN is an illness severity score that has been developed to predict mortality in SJS and TEN cases.
What are the Causes of Stevens-Johnson Syndrome?
Causes of Stevens Johnson Syndrome include the following:
Medications. This is the most common cause of SJS. Thereaction in drug-induced SJS occurs within a week of starting the medication, though it may occur even a month or two later with medications like anticonvulsants. The following medications have been particularly implicated in SJS:
- Antibiotics that include:
- Sulfonamides or sulfa drugs like cotrimoxazole
- Penicillins like amoxicillin and bacampicillin
- Cephalosporins like cefaclor and cephalexin
- Macrolides, which are broad-spectrum antibiotics and include azithromycin, clarithromycin, erythromycin
- Quinolones like ciprofloxacin, norfloxacin and ofloxacin
- Tetracyclines like doxycycline and minocycline
- Anticonvulsantsare used in the treatment of epilepsy to prevent seizures. Drugs like lamotrigine, carbamazepine, phenytoin, phenobarbitone, and particularly, the combination of lamotrigine with sodium valproate increases the risk of SJS
- Allopurinol, which is used for treating gout
- Acetaminophen, which is often considered as a safe drug for all age groups
- Nevirapine which is a non-nucleoside reverse-transcriptase inhibitor used to treat HIV infection
- Non-steroidal anti-inflammatory drugs (NSAIDs) – These are painkillers like diclofenac, naproxen, indomethacin and ketorolac

Infections:
Infections that can predispose to SJS include the following:
- Viral infections - Infections with viruses such as mumps, influenza, herpes simplex, Epstein-Barr virus, hepatitis A, and HIV have been associated with SJS. In pediatric cases, the Epstein-Barr virus and enteroviruses have been particularly associated with SJS.
- Bacterial infections - Infections such as mycoplasma pneumonia, typhoid, brucellosis and lymphogranuloma venereum may precede SJS
- Protozoal infections such as malaria and trichomoniasis may presdispose to SJS
Factors that increase the risk of SJS are:
- Genetic factors - Genetic variations most bly associated with Stevens-Johnson syndrome occurs in the HLA-B gene. Studies indicate a b association between HLA-A*33:03 and HLA-C*03:02 alleles and allopurinol-induced SJS or TEN, especially in an Asian population. The risk of suffering from SJS is higher if a close family member has suffered from an episode, which also indicates a possible underlying genetic risk factor.
- Weakened immune system - A weakened immune system as a result of HIV infection, autoimmune conditions, chemotherapy or organ transplants can predispose individuals to SJS.
- Previous history of Stevens-Johnson syndrome - There is a risk of SJS recurring if the same medication or medications from the same group that had previously caused the reaction are taken.
What are the Symptoms and Signs of Stevens-Johnson Syndrome?
Symptoms and signs of SJS include the following:
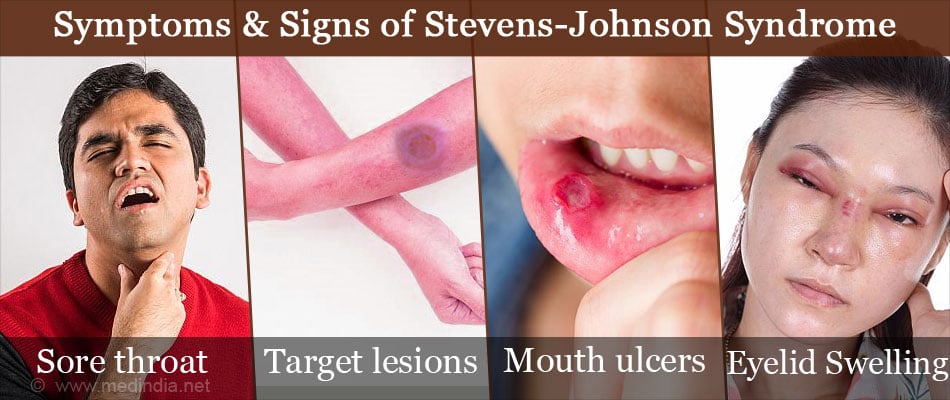
- Symptoms resembling an upper respiratory tract infection such as fever > 39° C, sore throat, cold and cough, headache and body pain
- Target lesions – These lesions that are darker in the middle surrounded by lighter areas are considered diagnostic of SJS
- Painful red or purplish rash, blisters on the skin, mouth, eyes, ears, nose and genital area. As the disease progresses, the flaccid blisters may merge and rupture thereby exposing painful sores. Eventually the top layer of the skin forms a crust and is shed.
- Facial swelling, swollen lips covered in crusty sores, and mouth ulcers. Ulcers in the throat can cause difficulty in swallowing, while those in the digestive tract can cause diarrhea, ultimately causing dehydration
- Swelling of eyelids, inflammation of the conjunctiva and /or photosensitivity, where eyes are sensitive to light
How do you Diagnose Stevens-Johnson Syndrome?
Diagnosis of Stevens-Johnson syndrome is based on the following:
- Clinical examination- A thorough clinical history which reveals the predisposing factor and presence of the characteristic target rash play a key role in the diagnosis of SJS
- Skin biopsy- A skin biopsy can help to confirm the diagnosis
How is Stevens-Johnson syndrome Treated?
Stevens-Johnson syndrome is a medical emergency and requires immediate hospitalization.
Firstly, the medicines suspected of causing SJS are stopped
Treatment of skin and mucous membrane lesions:
- The dead skin is gently removed and the sore areas of the skin are covered with a non-stick dressing to protect them against infection while they heal. Dressings with biosynthetic skin substitutes, or non-adherent nanocrystalline containing silver gauze may be used
- Antibiotics and local antiseptics are used to treat infection. Tetanus immunization may be given to prevent tetanus infection
- Intravenous immunoglobulins (IVIG) is given to stop the disease process. It is not clear whether corticosteroids, drugs used to control inflammation reduce mortality or hospital stay in toxic epidermal necrolysis and Stevens-Johnson syndrome since they could increase the chances of infection.
- Mouthwash and topical oral anesthetics are prescribed to alleviate pain in the mouth and throat and enable oral nutritional intake
- The eyes are treated with lubricant or artificial tears to stop the surface drying out. Topical steroids, antiseptics and antibiotics may be used to prevent inflammation and infection. Surgical treatment e.g. PROSE treatment (prosthetic replacement of ocular surface ecosystem) may be needed for chronic ocular surface disease
- Intravaginal steroid ointments are used in women to prevent scar tissue formation in the vagina
Other treatments used for SJS patients include:
- Nutritional and fluid replacement through a nasogastric tube or intravenously to prevent and treat dehydration and support nutrition
- Temperature maintenance of 30–32°C as body temperature regulation is impaired
- Analgesics/ painkillers for pain relief
- Intubation and mechanical ventilation, which may be required if the trachea (windpipe) and bronchi are affected, and the patient has respiratory problems
- Psychiatric support for extreme anxiety and emotional lability, if present
How do you Prevent Stevens-Johnson Syndrome?
It is very difficult to predict which patients will develop SJS. However,
- If a close family member may have developed SJS to a particular drug, it is best to avoid usage of that medicine or other medications belonging to the same chemical group. Always inform your doctor of the reaction in your family so that the doctor does not prescribe a possible allergen.
- If Stevens-Johnson syndrome has been caused by an adverse reaction to a medication, avoid taking the medication and other chemically similar medications in the future. Also, it is helpful to wear a Medicalert or equivalent bracelet so as to inform the treating health professional in case you are involved in an emergency situation and are not conscious or capable enough to inform them.

- Rarely, genetic testing may be recommended. For example, if you are of Chinese, southeast Asian or Indian descent, you can undergo genetic testing to determine whether the genes (HLA B1502 and HLA B1508) that have been associated with SJS caused by the medications carbamazepine or allopurinol are present or not.
What is the Prognosis of Stevens-Johnson Syndrome?
Patients with SJS or TEN caused by a drug have a better prognosis if the alleged drug is withdrawn early.
About one-third of all patients diagnosed with Stevens-Johnson syndrome have recurrence of the disease.
The death rate is 5% in SJS and about 30-35% in toxic epidermal necrolysis (TEN).
SCORTEN is an illness severity score that has been developed to predict the chances of people dying in SJS and TEN cases. One point is awarded for each of seven criteria present when the patient is admitted to the hospital. The SCORTEN criteria are:
- Age >40 years
- Presence of a malignancy
- Heart rate >120
- Initial percentage of epidermal detachment >10%
- Serum urea level >10 mmol/L
- Serum glucose level >14 mmol/L
- Serum bicarbonate level <20 mmol/L.
SCORETEN predicted mortality rates:
- SCORETEN 0-1 >3.2%
- SCORETEN 2 >12.1%
- SCORETEN 3 >35.3%
- SCORETEN 4 >58.3%
- SCORETEN 5 >90%
It can thus be noted that the higher the score, the greater is the risk of dying and therefore, worse is the prognosis.
 MEDINDIA
MEDINDIA
 Email
Email