- Stoke - (https://www.ahajournals.org/doi/10.1161/strokeaha.107.183689)
- Intracranial and extracranial hemorrhages in newborns with hemophilia: a review of the literature - (https://pubmed.ncbi.nlm.nih.gov/10445891/)
- Intracerebral Hemorrhage - (https://pubmed.ncbi.nlm.nih.gov/31971743/)
- Hemorrhage on MRI - (https://radiopaedia.org/articles/haemorrhage-on-mri)
- Stroke Facts - (https://www.cdc.gov/stroke/facts.htm)
- Recombinant Activated Factor VII in the Management of Massive Bleeding in Hospital Universiti Sains Malaysia - (https://clinicaltrials.gov/study/NCT03251547)
- New Treatments for Brain Hemorrhage - (https://journals.lww.com/em-news/fulltext/2007/07000/new_treatments_for_brain_hemorrhage.25.aspx)
What is Brain Hemorrhage?
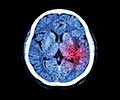
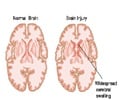
Brain hemorrhage otherwise called intracranial hemorrhage (ICH) is a type of hemorrhagic stroke that is specified by bleeding inside the skull and/or brain. It is a life-threatening emergency where the bursting of arteries causes brain damage that may even extend into the surrounding brain structures like meninges (protective brain layers) and ventricles (brain cavities)(1✔ ✔Trusted Source
Stoke
Go to source).
Intracranial hematoma, a condition where blood collects within the brain's parenchyma, exacerbates the situation, leading to cerebral ischemia and excruciating pain. This hemorrhagic stroke often occurs in individuals who are on blood thinners, increasing the risk of cerebral hemorrhage and eventual death.
Historical Evidence
Historically at the time of Hippocrates, the old word for stroke – “apoplexy” was used to denote all types of stroke – due to infarction as well as hemorrhage. Later in 1658, Wepfer devised the concept of hemorrhage as the cause of apoplexy.
The brain hemorrhage was first differentiated from other strokes in 1823 (two centuries later) by Rostan due to the appearance of ‘softening of the brain’ mediated via "leaks and plugs". When the leaked blood inside the brain starts clotting, it is called a hematoma.
Types of Brain Hemorrhage
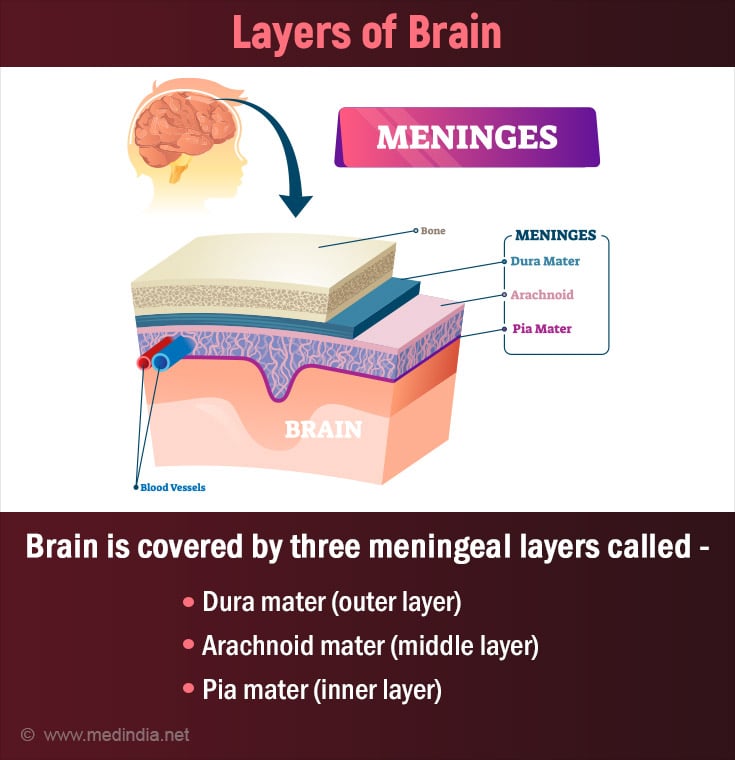
The brain is encased inside a tough bony skull followed by a protective three membranous layer (covering) called meninges. They are:
- Dura mater (outer tough layer)
- Arachnoid mater (middle layer with subarachnoid space for CSF flow)
- Pia mater (innermost layer attached to brain tissue)
Brain hemorrhage may occur fundamentally in two regions:
- Bleeding outside the brain but within the skull (extra cerebral hemorrhage). This incorporates bleeding in the meningeal layers:
- Epidural/ Extra dural hemorrhage (EDH): Bleeding between the skull and the dura mater. Differentiating feature – the presence of lucid interval where the patient is initially conscious followed by unconscious subsequently (incidence of 20−28%).
- Subdural hemorrhage (SDH): Bleeding between the dura mater and the arachnoid mater. The patient’s condition worsens within 24−72 hours of injury.
- Subarachnoid hemorrhage (SAH): Bleeding between the arachnoid mater and the pia mater (into the subarachnoid space)(2✔ ✔Trusted Source
Intracranial and extracranial hemorrhages in newborns with hemophilia: a review of the literature
Go to source). - Bleeding inside the brain (intra cerebral hemorrhage). It can be primary (spontaneous rupture of blood vessels) or secondary (underlying cause). This includes:
- Intra parenchymal hemorrhage: Bleeding inside the brain tissue/parenchyma. It may occur at different sites of the brain like lobes (lobar hemorrhage), thalamus (thalamic hemorrhage), pons (pontine hemorrhage), cerebellum (cerebellar hemorrhage), or anywhere within the brain tissue.
- Intra ventricular hemorrhage: Bleeding inside the brain cavities called ventricles – responsible for CSF (cerebrospinal fluid) production(3✔ ✔Trusted Source
Intracerebral Hemorrhage
Go to source).
To Read in Detail about types of Brain Hemorrhage, Click Here.
Stages of Brain Hemorrhage
Depending upon the time of onset of the hemorrhage it can be of the following types:
- Hyper acute stage: Lasts from minutes to a few hours (less than 24 hours)
- Acute stage: Lasts for the next 1 to 12 or 48 hours after onset
- Sub-acute stage: Lasts from 3 days to a week; Divided into the early (3 to 7 days) and late stages (7 to 14-28 days)
- Chronic stage: Lasts from 21−30 days(4✔ ✔Trusted Source
Hemorrhage on MRI
Go to source)
Statistics on Brain Hemorrhage
- Brain hemorrhage is the 2nd leading cause of stroke.
- It constitutes 13% of all strokes and 20% of all cerebrovascular diseases in the United States.
- Almost 2.5 per 10,000 people get affected annually, especially males and older population.
- Deaths occur in 44% of people within one month of diagnosis.
- Arteriovenous malformations (AVM) contribute to 2% of all hemorrhagic strokes every year(5✔ ✔Trusted Source
Stroke Facts
Go to source).
To Read more about Brain Hemorrhage Vs. Stroke, Click Here.
Causes and Risk Factors of Brain Hemorrhage
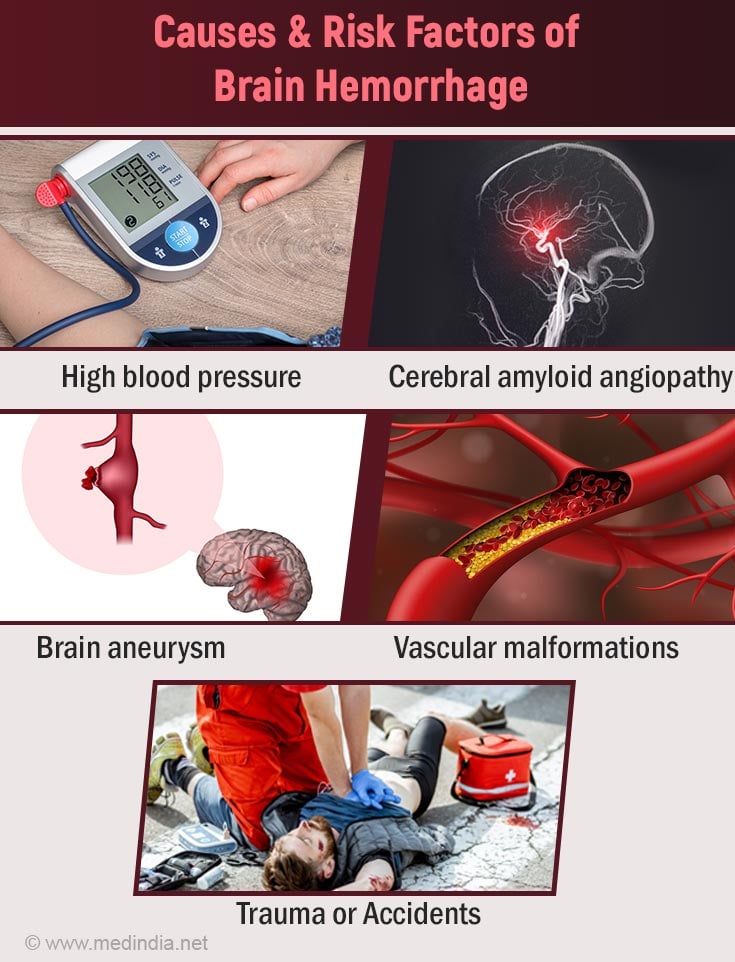
Almost 80% of brain hemorrhages are caused due to hypertension (high blood pressure). The increased blood pressure weakens the walls of the blood vessels. This results in the bursting of the blood vessels followed by blood leakage. Other etiological factors include:
- Cerebrovascular disorders (e.g., cerebral amyloid angiopathy - an abnormal build-up of amyloid proteins on the arterial wall of the brain).
- Brain trauma or accidents
- Enlargement of an artery due to a weak spot (Aneurysm)
- Vascular malformation (malformations of blood vessels e.g., arteriovenous malformation)
- Deposits of fatty plaques in the arteries (Atherosclerosis) and obesity
- Blood clots or occlusion in cerebral veins (Cerebral venous sinus thrombosis- CVST)
- Inflammation of blood vessels (Vasculitis)
- Brain tumors
- Blood thinners (Anticoagulants)
- Drug abuse (cocaine), smoking, and
alcoholism - Abnormal clotting disorders (e.g. hemophilia)
- Liver disease
- Idiopathic (unknown cause)
Symptoms of Brain Hemorrhage
The larger the bleed, the more severe the symptoms. Generally, a brain hemorrhage must be treated as an emergency unless the life-threatening cause is ruled out. Certain symptoms of brain hemorrhage may resemble that of stroke:
Small Bleed on the Brain Symptoms
Headache: A sudden, severe headache is a common symptom of a small brain bleed. The headache may feel different from regular headaches and may worsen over time.
- Nausea and Vomiting: Feeling nauseous or vomiting without any apparent cause can be a sign of a small brain bleed.
- Changes in Mental Status: Confusion, disorientation, difficulty concentrating, and memory problems may occur due to a small bleed on the brain.
- Weakness or Numbness: Weakness, numbness, or tingling sensations in the arms, legs, or face may be indicative of a small intracranial hemorrhage.
- Vision Changes: Blurred vision, double vision, or other visual disturbances can occur as a result of pressure on the optic nerve or other parts of the visual pathway.
- Speech Difficulties: Slurred speech or difficulty speaking clearly may be observed in individuals with a small bleed on the brain.
- Seizures: Seizures can occur if the bleeding irritates brain tissue or affects normal electrical activity in the brain.
- Loss of Consciousness: In more severe cases, loss of consciousness or coma may occur, especially if the bleeding is significant or if there are other complicating factors.
Symptoms of Large Bleed in the Brain
- Sudden onset of severe headache(typical ‘thunderclap headache’ in subarachnoid hemorrhage)
- Loss of consciousness over 24 to 48 hours of onset or stupor or lethargy
- Hemiparesis (one-sided weakness) hemiplegia (one-sided paralysis) or quadriplegia (paralysis of all 4 limbs)
- Visual and speech disturbances
- Vomiting and dizziness
- Seizures
- Neck stiffness or signs of meningism (SAH)
- Fever (damage to the hypothalamus – brain structure vital for hormonal regulation)
Unsteadiness in walking (Ataxia) - Coma
- Death

Signs of Brain Hemorrhage
- Brain edema/swelling
- Midline shift of the brain (space-occupying effect in the brain)
- Raised intracranial pressure (ICP - Raised pressure inside the brain)
- Hydrocephalus (accumulation of cerebral fluid inside the brain)
- Kernig’s sign positive in subarachnoid hemorrhage (stretching of the nerve roots by extending the knee causes pain)
- Papilloedema (swelling of the optic nerve - responsible for vision)
- Pupillary asymmetry
Diagnosis of Brain Hemorrhage
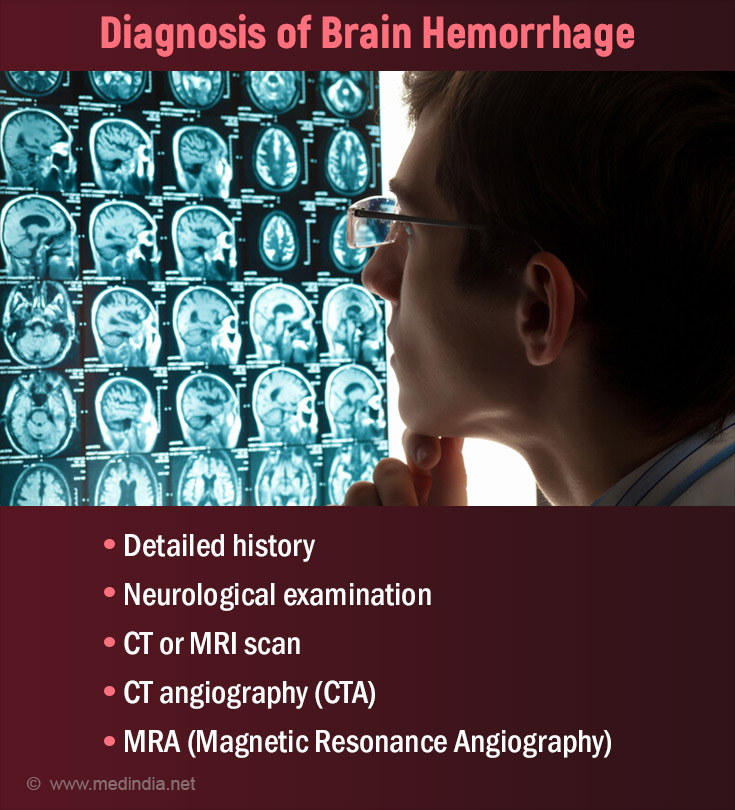
- Detailed history and neurological examination are the keys to an apt diagnosis.
- CT scan: The gold standard tool of investigation for a brain hemorrhage is a CT scan. It helps in determining the site of the bleed along with its extent.
- Epidural/ Extradural hemorrhage (EDH) appears as a hyperdense (bright white), biconvex (lenticular) mass adjacent to the skull.
- Subdural hemorrhage (SDH) appears as hyperdense, crescentic collections between the dura and the arachnoid mater.
- Subarachnoid hemorrhage (SAH) appears as a hyperdensity in the subarachnoid space
- Cerebral Angiography:
- It employs the visualization of brain arteries through X-rays and injecting iodine-containing contrast material into the blood vessels. The contrast reaches the target structure by insertion of a catheter (thin tube) in the arteries of the hands or legs and guiding the tube to the brain.
- If the images of the blood vessels are electronically manipulated rather than x-ray film, then the technique is referred to as intra-arterial digital subtraction angiography (IADSA).
- CT angiography (CTA): CT scan of the blood vessels by injecting the contrast material into the blood. This helps in ruling out causal factors like vascular malformations, aneurysms, or vasculitis.
- Magnetic Resonance Imaging (MRI) with MRA (Magnetic Resonance Angiography): Due to better resolution and multiplanar capabilities, MRI of the brain may help demonstrate even smaller hematomas. It also helps in differentiating chronic brain hemorrhages. MRA helps in the visualization of blood vessels simultaneously. However, MRIs can be time-consuming in an emergency setting.
- Digital angiography: In cases where CTA or MRA fails to exhibit a positive finding, the four-vessel angiography is performed. Along with 3-D rotational techniques, multiple views of the vessels or the aneurysm can be made to aid the precise diagnosis.
- Spinal tap or lumbar puncture: Enables examination of the cerebrospinal fluid that surrounds the brain. Useful to diagnose subarachnoid hemorrhage. However, it is contraindicated in severe cases due to the risk of herniation (lethal displacement of the brain from its original position due to high pressure).
- Infrared spectroscopy: Furnishes reasonable sensitivity and specificity for the detection of intracranial lesions in a short time when the patient is critically ill and requires urgent surgical intervention.
- Blood tests to evaluate the coagulation profile (blood clotting ability) of the patient
- Radionuclide tracers, such as 99mTc hexamethyl propylene amine oxime (99mTc-HMPAO) and xenon-enhanced CT cerebral blood flow studies are performed in cases where regional cerebral blood flow is to be measured.
- Glasgow coma scale (GCS) or National Institutes of Health Stroke Scale (NIHSS) helps assess the level of consciousness or neurological status.
Treatment of Brain Hemorrhage
Smaller hemorrhages can be managed with conservative treatment in fully conscious patients. Other strategies for larger hemorrhages include:
- Initial Assessment :
- Immediate transfer of the patient to the intensive care unit or stroke unit.
- Assessment of airway, breathing, and circulation to aid patients’ stabilization.
- A patient with a GCS score of less than 9 should be kept under strict intracranial pressure monitoring.
- Hypotension (low blood pressure) and hypoxemia (low oxygen level in the blood) should be avoided.
- Surgery:
- Hematoma evacuation through surgery within 4 hours of onset (Burr-hole, craniectomy, stereotactic evacuation, or endoscopic evacuation depending upon the location).
- Ventricular drainage of blood.
Brain Hemorrhage Surgery
Purpose: Brain hemorrhage surgery, also known as neurosurgery for intracranial hemorrhage, aims to address bleeding inside the brain to relieve pressure and prevent further damage.
Indications for Surgery: The decision to perform brain hemorrhage surgery depends on factors such as the size, location, and severity of the hemorrhage, as well as the patient's overall health condition and neurological status.
- Medications:
- The strict control of blood pressure through antihypertensive therapy. It aims to achieve a systolic pressure of 140 mmHg as per The American Heart Association and American Stroke Association guidelines.
- The head of the patient is elevated to 30 degrees along with an infusion of 20% mannitol (1.0-1.5 g/kg) to reduce fluid and pressure load in the brain.
- The patient may be connected to ventilation (respiratory support) to maintain the pCO2 (carbon dioxide level) at 30−35 mmHg.
- Intravenous administration of prothrombin concentrate, frozen plasma, protamine, platelet transfusions, or vitamin K for patients on blood thinners.
- Control of blood glucose levels through anti-diabetic drugs.
- Anti-seizure medications to control seizures.
- Sedatives (sleep-inducing medications) to reduce agitation in patients.
- Corticosteroids may increase mortality rates. Hence they must be strictly avoided if a patient suffers from a brain hemorrhage.
Treatment
Surgical Techniques: Neurosurgeons may use different techniques during the surgery, including:
- Craniotomy: Involves temporarily removing a portion of the skull to access the brain and remove the clot causing the hemorrhage.
- Minimally Invasive Approaches: Such as making a small hole in the skull to drain excess blood or fluid from the brain(6✔ ✔Trusted Source
Recombinant Activated Factor VII in the Management of Massive Bleeding in Hospital Universiti Sains Malaysia
Go to source).
Anesthesia and Monitoring: The surgery is typically performed under general anesthesia to keep the patient unconscious and pain-free. Patients are closely monitored in the intensive care unit post-surgery to assess neurological status and prevent complications.
Risks and Considerations: While brain hemorrhage surgery can be life-saving, it carries risks like any surgical procedure, including infection, swelling, and potential neurological deficits.
Multidisciplinary Approach: Close collaboration between neurosurgeons, neurologists, and other healthcare professionals is essential to ensure optimal outcomes for patients undergoing brain hemorrhage surgery.
- Rehabilitation: Regular rehabilitation, depending upon the symptoms helps in improving the outcomes. These include:
- Physical therapy
- Speech therapy
- Occupational therapy(7✔ ✔Trusted Source
New Treatments for Brain Hemorrhage
Go to source)
Differential Diagnosis of Brain Hemorrhage
Conditions that may mimic brain hemorrhage include:
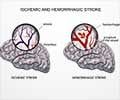
- Ischemic stroke (due to a blood clot or narrowing of an artery)
- Transient ischemic attack (TIA - minor stroke)
- Acute hypertensive crisis (extremely increased level of blood pressure beyond 180 mm Hg of systolic pressure and 120 mm Hg diastolic pressure)
- Sentinel headache (pre-stroke headache especially in subarachnoid hemorrhage)
- Sinusitis (may result in headache due to inflammation or swelling of the sinuses)
- Hypoglycemia (low levels of blood sugar may cause loss of consciousness)
- Cerebral venous thrombosis (blood clots or occlusion in cerebral veins)
- Spontaneous intracranial hypotension (due to loss of cerebrospinal fluid volume through damage in the dura mater of the spinal cord)
- Reversible cerebral vasoconstriction syndrome(results in severe headaches that occur as a result of blood vessels narrowing in the brain)
Prognosis of Brain Hemorrhage
The overall prognosis or mortality from brain hemorrhage ranges between 25–60%. If the patient is in a coma, the mortality rate increases up to 90%. Other prognostic factors include:
Poor Prognostic Factors
- Poor neurological status like loss of consciousness and coma (no response to even deep pain).
- Older age group as they tend to have more comorbid conditions.
- Delayed surgery, beyond 4 hours of onset.
- CT parameters like increased clot thickness, hematoma volume, and midline shift.
- Persistent elevation of intracranial pressure (> 20 mm Hg), especially post-operative.
- Pontine and brain stem hemorrhage have a high mortality rate as it may end in the compression of vital respiratory and circulatory centers in the brain.
- Presence of intracerebral/ intraventricular haematoma or contusion (brain damage).
- Comorbidities like lung infections, sepsis, meningitis (inflammation of the meninges), cardiac arrhythmias (irregular heart rhythms), or gastrointestinal hemorrhages.
Good prognostic factors
- Small and superficial hematomas or lesions.
- No loss of consciousness or patient localizes to painful stimuli.
- Intraventricular hemorrhage may show complete recovery (however larger bleed may worsen the condition).
Brain Hemorrhage Self-Care
Follow Medical Advice: Adhere strictly to the treatment plan outlined by your healthcare provider, including medication schedules, follow-up appointments, and any lifestyle recommendations.
Rest and Recovery: Allow yourself plenty of rest and avoid strenuous activities that could increase your blood pressure or strain your brain. Listen to your body and take breaks when needed.
Medication Management: Take prescribed medications as directed by your healthcare provider. These may include blood thinners, anticonvulsants, pain relievers, or other medications to manage symptoms and prevent complications.
Monitor Symptoms: Stay vigilant for any new or worsening symptoms such as severe headaches, vision changes, weakness, numbness, difficulty speaking, or seizures. Contact your healthcare provider immediately if you experience any concerning symptoms.
Healthy Lifestyle Choices: Focus on maintaining a healthy lifestyle by eating a balanced diet rich in fruits, vegetables, lean proteins, and whole grains. Stay hydrated, limit alcohol consumption, and avoid smoking or using recreational drugs.
Manage Stress: Practice stress-reduction techniques such as deep breathing, meditation, yoga, or mindfulness to promote relaxation and reduce anxiety.
Physical Activity: Engage in light to moderate physical activity as recommended by your healthcare provider. Walking, gentle stretching, and low-impact exercises can help improve circulation, mood, and overall well-being.
Safety Precautions: Take necessary precautions to prevent falls and injuries, especially if you experience balance or coordination problems. Install handrails, remove tripping hazards, and use assistive devices if needed.
Stay Connected: Seek emotional support from family, friends, support groups, or mental health professionals if you're feeling overwhelmed or anxious about your recovery process.
Regular Follow-up Care: Attend scheduled follow-up appointments with your healthcare provider to monitor your progress, adjust treatment plans as needed, and address any concerns or questions you may have.
Prevention of Brain Hemorrhage
Certain measures that may help reduce the risk of brain hemorrhage include:
- Monitor your blood pressure and cholesterol levels
- Stop smoking and alcohol consumption
- Avoid using drugs like cocaine as it increases the risk of brain bleed
- Consult your specialist if you are on blood-thinning drugs (warfarin)
- Follow a daily exercise regimen that includes at least 150 minutes of moderate to intense exercise every week as per AHA (American Heart Association)
- Follow a healthy balanced diet. DASH diets are reported to be good for brain health
- Lifestyle modifications like avoiding a sedentary lifestyle and reducing weight (if you are obese)
- Most importantly, wear your helmet and seat belt while riding to avoid brain hemorrhages due to accidents
 MEDINDIA
MEDINDIA

 Email
Email