- Overview - Intracranial Hypertension - (http://www.mayoclinic.org/home/ovc-20249919)
- Google Books: Cerebral Herniation Syndromes and Intracranial Hypertension - Page 66.
What is Intracranial Hypertension?
Intracranial hypertension is a medical condition resulting from increased pressure around the brain.
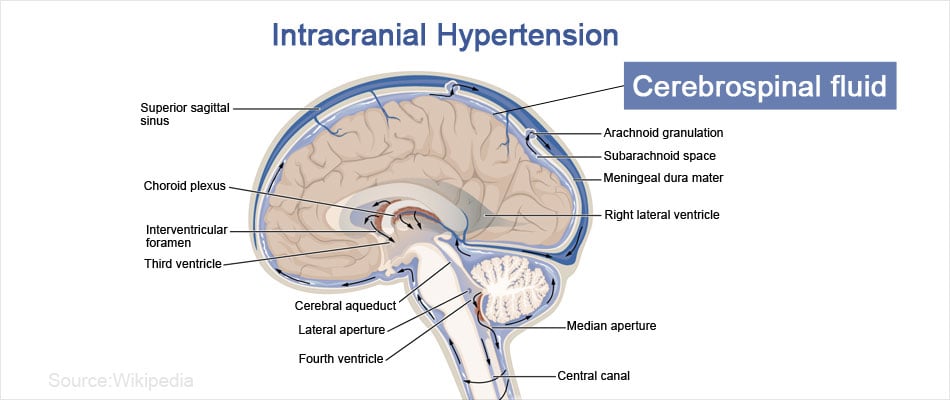
The brain is surrounded by fluid filled spaces or ventricles, which act as a cushion and prevent the brain from injury. Fluid in these spaces is called cerebrospinal fluid (CSF). When the fluid pressure inside these spaces increases, it leads to increased compression of nearby structures, mainly the optic nerve. As a result, intracranial hypertension often impacts the eyes. The spaces inside the skull cannot expand and can therefore accommodate only a fixed volume of cerebrospinal fluid.
What are the Causes of Intracranial Hypertension?
Intracranial hypertension may occur with or without any underlying cause. If it happens without any underlying cause, it is called idiopathic intracranial hypertension. Earlier, intracranial hypertension was referred to as benign, but since it can result in permanent loss of vision, it is no longer referred to as benign. It is also called pseudotumor cerebri because its signs and symptoms mimic that of a brain tumor.
Increased intracranial pressure can be due to a tumor, internal bleeding owing to hemorrhage, or swelling within the brain.
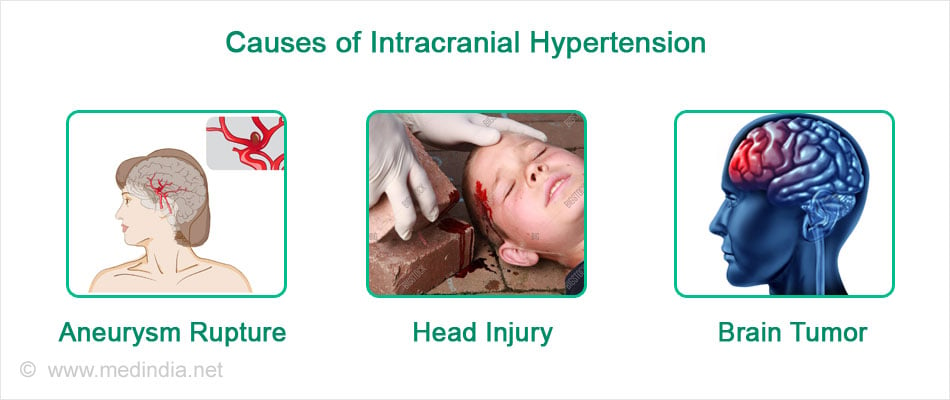
Common causes of intracranial hypertension include:
- Aneurysm rupture
- Subarachnoid hemorrhage
- Brain tumor
- Encephalitis
- Head injury
- Hydrocephalus
- Hypertensive brain hemorrhage
- Intraventricular hemorrhage
- Meningitis
- Subdural hematoma
- Status epilepticus
- Stroke
What are the Risk Factors for Idiopathic Intracranial Hypertension?
There are certain conditions that predispose to the development of intracranial hypertension. These include
- Obesity
- Intake of certain medication namely, growth hormone, tetracycline, excess vitamin A, oral contraceptives, steroids, isotretinoin, lithium, nitrofurantoin, phenytoin sulfa drugs, minocycline, Tamoxifen, nalidixic acid, thyroid replacement, and some chemotherapeutic drugs
Intracranial hypertension can be a secondary complication in certain medical conditions like:
- Addison's disease
- Anemia
- Behcet's syndrome
- Blood-clotting disorders
- Lupus
- Kidney disease
- Polycystic ovary syndrome
- Sleep apnea
- Underactive parathyroid glands
- Uremia
- Blockage of the brain’s venous drainage (dural sinus thrombosis)
- Renal disease
- Head injury
- Lyme disease
- Lupus
- Acute sinusitis
- Measles
- Blood clotting disorders
- Anemia
- Malnutrition
What are the Symptoms of Intracranial Hypertension?
The most often reported symptom of intracranial hypertension is headache of fluctuating intensity, which occurs daily and may or may not be associated with nausea and vomiting. The headache might worsen with coughing or straining.
Most important neurological manifestation in chronic intracranial hypertension is bilateral papilledema. Increased pressure on the optic nerve leads to papilledema. It is the swelling of the optic disc, the spot where the optic nerve enters the eyeball. This result in symptoms’ related to disrupted vision or temporary visual loss. If not treated timely, might result in permanent visual loss which is irreversible even though the intracranial pressure gets reduced.
- Pulsatile tinnitus (a ringing sound heard in one or both ears)
- Horizontal double vision (results owing to increased compression on the 6th cranial nerve)
- Radiating pain in the arms or legs
- Blurred vision owing to blind spots in the eyes
- Temporary visual loss
- Loss of color vision
- Difficulty seeing to the side
- Light flashes (photopsia)
- Problems with balance and spatial awareness
How is Idiopathic Intracranial Hypertension (IIH) Diagnosed?
History and Physical Examination
It is essential to take a complete medical history of the patient and perform a thorough physical examination to understand the onset of symptoms and their association with any existing or past medical problem and identify the presence of any underlying risk factor.
Opthalmoscopic Examination
Then as a next step, the doctor will examine the eyes of the patient with an ophthalmoscope to check for any swelling in the optic disc or presence of any additional blind spots.
Diagnostic Imaging
This is further followed by detailed neurological examination through various diagnostic imaging scans namely, magnetic resonance imaging (MRI) and computerised tomography (CT) scan to identify the cause and extent of the problem such as occurrence of a brain tumor or presence of blood vessel clots.
Lumbar Puncture
A lumbar puncture may be necessary to check the CSF pressure and to estimate the glucose and protein levels of the CSF.
What is the Treatment for Intracranial Hypertension?
The most important aim of treatment is to save the vision of the patient. Therefore, the vision of the patient is very closely monitored by regular eye examinations and to arrest the vision loss by immediate steps.
Medical Treatment
Initially, if there is no vision loss, medications are prescribed to reduce the cerebrospinal fluid pressure within the skull.
- This is done by either by draining out excess fluid through diuretics or by reducing the production of CSF by carbonic anhydrase inhibitors.
- Symptomatic treatment like pain killers for headache and medicines to control nausea are prescribed.
- The doctor might suggest repeated lumbar punctures to drain out fluid from spine so as to reduce pressure on brain. Despite the ongoing medical treatment, if any vision loss is diagnosed or the symptoms are progressive, surgery is considered.

Surgical Treatment
Surgical treatment aims at relieving the intracranial pressure thereby reducing the compression on nearby anatomical structures of the brain. Two major types of surgeries are done:
- Shunting - The surgical procedure called shunting drains out the extra CSF. This is done by inserting a tube in the fluid filled space of the skull. Either the fluid is drained out or diverted to other parts of the body, which enables its excretion. But shunting can be associated with complications like infection, CSF blockage, and too much CSF drainage.
- Optic Nerve Sheath fenestration - The protective layer (sheath) surrounding the nerve connecting eye and brain, called optic nerve, is opened by making small cuts to relieve the pressure on optic nerve, thereby reducing the impact on eye. But this procedure has little impact on overall pressure of the skull.
Other Treatments
- Losing weight, especially in case of obesity helps in reducing the symptomatic impact of intracranial hypertension.
What is the Prognosis of Intracranial Hypertension?
Treatment is mainly to relieve symptoms but relapse can occur. If started early, treatment helps in preventing loss of vision.
What are the Lifestyle Changes to Manage Intracranial Hypertension?
- Avoid heavy sports activities like twisting, jumping, running, swimming
- Avoid excessive sun exposure
- Limit fats and salt intake; high salt intake causes water retention in the body which combined with high-calorie diet leads to weight gain

- Reduce the intake foods rich in vitamin A, such as beef liver and certain vegetables, namely carrots, tomatoes, sweet potatoes and leafy greens rich in vitamin A
- Reduce the intake of foods rich in tyramine, which include preserved, dried or smoked foods such as pepperoni, liverwurst, pickle, salami, cheese, beer, wine, nuts, fermented soy products, olives and broad beans. Tyramine results in dilatation of blood vessels which is harmful in cases of high intracranial pressure
- Avoid intensive activities like bungee jumping, negative G-force rides at amusement parks, judo and rugby
- Limit alcohol consumption
- Avoid caffeine intake as it can cause dilation of blood vessels and dehydration