Patients at Michigan hospitals are less likely to experience a urinary tract infection caused by a catheter than at other hospitals in the United States, a new study reveals.
"Michigan hospitals, which have taken the lead in applying low-tech practices aimed at timely removal of urinary catheters, are also proving to be leaders in reducing the risk of patient harm from UTIs."
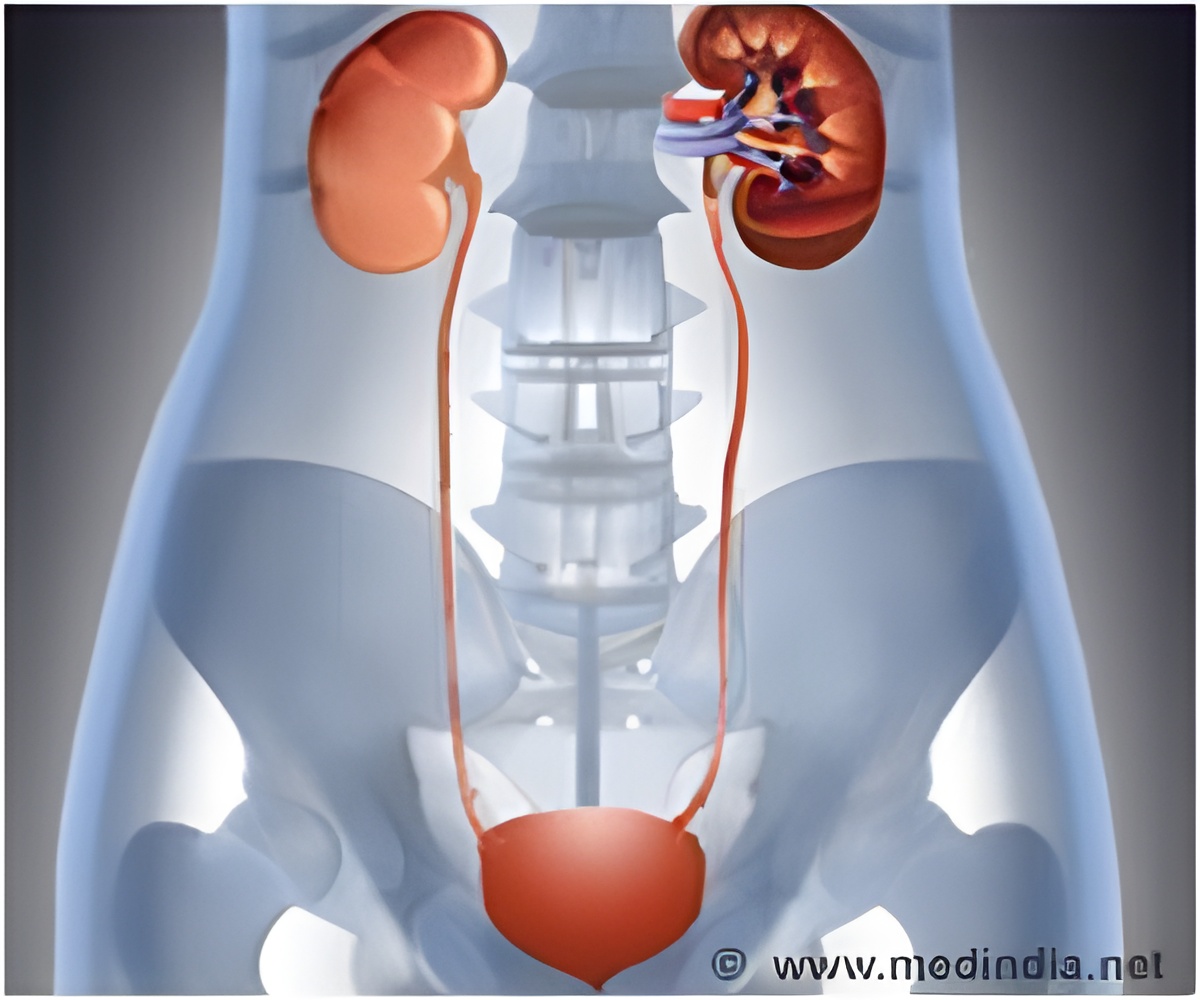
UTIs, which often arise from catheters used to empty bladders for hospitalized patients, are responsible for 35 percent of infections related to hospitalization and can, lead to serious complications. Aiming to cut expenses and improve care, a 2008 Medicare policy stopped paying hospitals for the cost of treating preventable urinary tract infections that develop in hospitalized Medicare patients.
Michigan's Keystone "Bladder Bundle" Initiative has focused on a significantly higher use of practices aimed at timely removal of urinary catheters in Michigan hospitals. The study published in JAMA Internal Medicine, funded by a $1.7 million grant from the National Institutes of Health four years ago, supports efforts by UMHS and the VA Ann Arbor Healthcare System to help hospitals find the best ways to prevent UTIs.
Saint and his colleagues found that Michigan hospitals were more likely to participate in efforts to reduce catheter-associated infections by using bladder-scanners as well as reminders or stop-orders to ensure catheter use was discontinued at an appropriate time. More frequent use of preventive practices coincided with a 25 percent reduction in UTI rates at Michigan hospitals compared to a 6 percent overall decrease experienced by other U.S. hospitals."These data reinforce the significance of appropriately maintaining and removing catheters in the effort to prevent catheter-associated UTIs," says Saint, who is also the director of the U-M/VA Patient Safety Enhancement Program, and leader of several other studies on infection prevention including some taking place in Italy and Japan.
"The Keystone Bladder Bundle project in Michigan provides an effective model for implementing strategies to lower patients risk of developing a UTI in the hospital. There is clearly a need to identify strategies to help hospitals in other states - and even other countries - enact similar practices to improve care and reduce healthcare costs."
"Every hospital has its own approach to catheter use that's become ingrained into that specific institution's culture of care," says lead author of the second study Sarah Krein, Ph.D., R.N. research associate professor, U-M Department of Internal Medicine, research scientist, VA Ann Arbor Healthcare System; and of the U-M School of Nursing.
Krein and Saint are on the national leadership team of a nationwide project funded by the Agency for Healthcare Research and Quality (AHRQ) that aims to reduce catheter-associated UTIs by 25 percent in all 50 states and Puerto Rico. So far, approximately 800 hospitals are participating.
Source-Newswise
 MEDINDIA
MEDINDIA
 Email
Email