The serum-based test would be the first of its kind to be used to detect acute intracranial bleeding hemorrhage in infants.
Highlights
- Approximately 30 percent of acute intracranial hemorrhage (AHT) diagnoses are missed when caretakers provide inaccurate histories or when infants have nonspecific symptoms such asvomiting or fussiness.
- Biomarkers for Infant Brain Injury Score (BIBIS) is a formula to discriminate between infants with and without intracranial hemorrhage.
- The test takes into account multiple biomarkers simultaneously using an extremely small amount of blood and detects AHT 90 percent of the time.
TOP INSIGHT
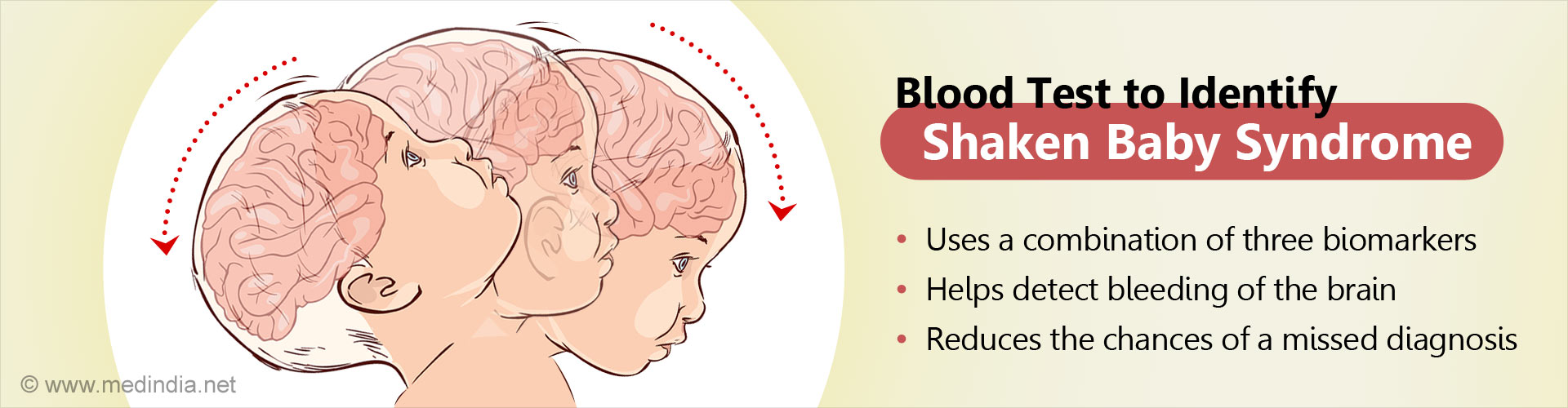
The Biomarkers for Infant Brain Injury Score (BIBIS) helps identify shaken baby syndrome when the symptoms may be unclear and help physicians make a decision about whether an infant needs brain imaging.
However, approximately 30 percent of AHT diagnoses are missed when caretakers provide inaccurate histories or when infants have nonspecific symptoms such as vomiting or fussiness. Missed diagnoses can be catastrophic as AHT can lead to permanent brain damage and even death.
Berger and colleagues at Children's Hospital and the Safar Center for Resuscitation Research at Pitt's School of Medicine have long been researching approaches to detect acute intracranial hemorrhage in infants at risk.
Biomarkers for Infant Brain Injury Score
In the current study, the researchers collaborated with Axela, a Canadian molecular diagnostics company, to develop a sensitive test that could reduce the chances of a missed diagnosis by using a combination of three biomarkers along with a measure of the patient's level of hemoglobin, the protein that carries oxygen in blood.
To arrive at the formula, called the Biomarkers for Infant Brain Injury Score (BIBIS), for discriminating between infants with and without intracranial hemorrhage, the team used previously stored serum samples from a databank established at the Safar Center.
"The test is not intended to replace clinical judgement, which is crucial," said Dr. Berger. "Rather, we believe that it can supplement clinical evaluation and in cases where symptoms may be unclear, help physicians make a decision about whether an infant needs brain imaging."
The specificity of the test--or the ability to correctly identify an infant without bleeding of the brain who would not require further evaluation--was 48 percent. The researchers aimed for the test to be highly sensitive rather than maximizing accuracy, since missing a diagnosis has more serious consequences than performing brain imaging in babies without the condition.
Reference
- Rachel Berger et al., Blood test shows promise in detecting abusive head trauma in infants , JAMA Pediatrics (2017).
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email