Interleukin-6 levels which cause immune response and thrombosis was reduced when two molecules- IL-23 and IL-27 were blocked.
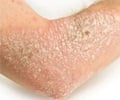
- Psoriasis is well-known for causing too many skin cells on elbows, knees, and across the body.
- Overactive immune cells in the skin can spread and inflame arteries, causing heart attacks and stroke.
- Interleukin-6 triggers immune response in the skin and also is found in patients with congestive heart failure.
"We wanted to pursue the mechanisms by which skin inflammation contributes to cardiovascular disease," said Nicole Ward, PhD, associate professor of dermatology at Case Western Reserve University School of Medicine. "In multiple mouse models, we showed removing IL-6 reduced cardiovascular risk, but did not get rid of psoriasis unless combined with other interventions."
In psoriasis clinical trials, blocking IL-6 hasn't been successful. Trial results show IL-6 inhibitors don't reliably improve skin, and can even cause spontaneous psoriasis in people who didn't have it before. A protein called MRP14, which has been used to predict heart attack risk in certain populations was tested. People with autoimmune diseases like psoriasis have high levels of MRP14 in their blood, and the gene encoding MRP14 is located near psoriasis genes. The researchers deleted the gene encoding MRP14 in mice with psoriasis, hoping it would reduce thrombosis.
"The disappointing result was that after two years of work, it had no effect on skin inflammation or cardiovascular comorbidities," said Ward. "The MRP14-deficient psoriasis mice were completely the same as the regular psoriasis mice - they all had similar levels of skin inflammation and thrombosis."
The MRP14-deficient psoriasis mice still had lots of IL-6 in their skin, plus two other pro-inflammatory molecules, called IL-23 and IL-17. Ward hypothesized that IL-23 and IL-17 could be part of a "workaround" mechanism in the mice that compensated for a lack of MRP14 and sustained skin inflammation.
Ward said, "We discovered that blocking IL-23/IL-17 decreased skin-derived IL-6 in MRP14-deficient psoriasis mice and reversed the thrombosis." In another study Ward identified several immune system molecules impacted by the genetic deletion of IL-6 in her psoriasis mice. Said Ward, "We were surprised to see compensatory increases in other pro-inflammatory molecules that we know are critically involved in sustaining skin inflammation. It is possible that these factors also increase in psoriasis patient skin and explain why they do not respond clinically to IL-6 blockade."
Reference
- Jonathan Karn et al., Immune System’s “Workaround” May Explain Heart Disease in Psoriasis Patients, JCI Insight (2016), http://casemed.case.edu/newscenter/news-release/newsrelease.cfm?news_id=459.
Source-Medindia