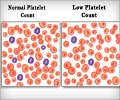
Research has revealed that blood transfusion received while treating a heart attack is capable of causing more harm than good.
Saurav Chatterjee, MD, of Brown University and Providence Veterans Affairs Medical Center, Rhode Island, and his colleagues, carried out a review of studies published during the period between January 1966 and March 2012.
Ten studies, comprising 203,665 subjects, were included for analysis. All studies were observational, while just a single study was a randomized trial. The analysis was carried out to assess the effect of blood transfusion in myocardial infarction (heart attack) patients as against no blood transfusion during myocardial infarction. It was found that there was a death risk increase by 12 percent in the former.
Other statistical studies revealed that blood transfusion was linked to a higher risk for death and this was independent of baseline or nadir hemoglobin level or any other change in hemoglobin level during the patient’s stay in the hospital. Blood transfusion is also a risk factor for subsequent heart attack, the study showed.
The study published online by the Archives of Internal Medicine, a publication of the JAMA Network, concluded that the risks for all-cause mortality and subsequent myocardial infarction are notably greater in acute myocardial infarction patients getting a blood transfusion.
Jeffrey L. Carson at the University of Medicine and Dentistry of New Jersey, and Paul C. Hébert at the Ottawa Hospital Research Institute, Canada, however, are not very convinced. According to them, ‘The authors remind us that patients with an acute myocardial infarction are often anemic and receive red blood cell transfusion. However, because of its many limitations, as physicians, we should not use the results of this review to justify or limit the use of red blood cells’.