Most prescribed blood pressure drugs such as ACE inhibitors could be less effective than others. Patients administered thiazides as first-line therapy experience 15 percent fewer cardiovascular events.
- Most frequently prescribed blood pressure drugs could be less effective than others
- Popular antihypertensive medications like ACE inhibitors are not as effective as thiazides that are prescribed less frequently
- This revelation could bring about a change in doctor’s prescribing habits for treating high blood pressure (hypertension)
The research team calculated that approximately 3,100 major cardiovascular events could have been averted if the patients who received ACE inhibitors as the first-line therapy were prescribed thiazide diuretics instead. The study has been published in the prestigious medical journal The Lancet.
Mechanism of Blood Pressure Control by ACE Inhibitors and Thiazide Diuretics
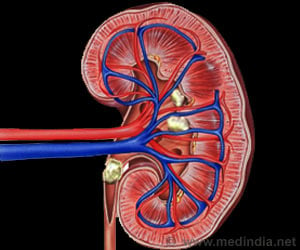
Angiotensin-converting enzyme (ACE) is a molecule responsible for the conversion of Angiotensin I to Angiotensin II, which causes constriction of the blood vessels. ACE inhibitors are drugs that block this conversion so that Angiotensin II is not produced, which results in relaxation of the blood vessel walls, thereby decreasing BP.Thiazide diuretics are drugs that promote diuresis (increased urine flow) by blocking the reabsorption of sodium (Na+) and chloride (Cl-) ions from the distal convoluted tubules of the nephrons in the kidneys. This increases urine flow, resulting in the lowering of BP.
Study Team
The study was jointly led by Dr. George Hripcsak, MD, MS, and Dr. Patrick Ryan, PhD. Dr. Hripcsak is the Vivian Beaumont Allen Professor of Biomedical Informatics and Chair of the Department of Biomedical Informatics at Columbia University, New York. He is also the Director of Medical Informatics Services at New York-Presbyterian Hospital, New York, USA.Dr. Ryan is an Adjunct Assistant Professor of Biomedical Informatics at Columbia University Vagelos College of Physicians and Surgeons, New York. He is also Vice President, Observational Health Data Analytics at Janssen Research & Development, LLC, a subsidiary of Johnson & Johnson, based in Raritan, New Jersey, USA.
What are the Drawbacks of Current Guidelines on Antihypertensive Drugs?
Current guidelines for the use of antihypertensive drugs are available from the American College of Cardiology and the American Heart Association. These guidelines recommend that treatment of hypertension could be started with any of the following 5 classes of antihypertensive drugs:- Thiazide diuretics
- ACE inhibitors
- Angiotensin II receptor blockers (ARBs)
- Dihydropyridine calcium channel blockers
- Non-dihydropyridine calcium channel blockers
“Randomized clinical trials demonstrate a drug’s effectiveness and safety in a highly defined patient population,” says Hripcsak. “But they’re not good at making comparisons among multiple drug classes in a diverse group of patients that you would encounter in the real world.”
Observational studies are sometimes useful for detecting effects that may be missed in randomized clinical trials. However, these are usually small-scale studies, which make it difficult to draw meaningful conclusions due to the scanty data generated.
“Unintentionally or not, journals and authors tend to publish studies that have exciting results, and researchers may even select analytical methods that are best suited to getting the results that fit their hypotheses,” says Hripcsak. “It comes down to a cherry-picking exercise, which makes the results less reliable.”
How Did the New Study Overcome the Drawbacks?
In order to overcome the drawbacks, a team of researchers analyzed electronic health records of millions of patients, which took into account tens of thousands of variables that are crucial for the exclusion of any confounding factors. The analytical technique used is termed Large-Scale Evidence Generation and Evaluation across a Network of Databases (LEGEND). This technique was developed by a consortium of scientists who were part of the Observational Health Data Science Initiative (OHDSI). The LEGEND technique enabled the scientists to share their methodology and refine the data, thereby significantly reducing bias.“LEGEND provides a systematic framework that can reproducibly generate evidence by applying advanced analytics across a network of disparate databases for a wide array of exposures and outcomes,” says Ryan. “Not only does LEGEND offer a path to scale to the real needs of the healthcare community, it also provides the complementary diagnostics to help us understand how much we can trust the evidence we’ve produced.”
Study Procedure
- 4.9 million electronic health records and insurance claims of patients from 4 countries were analyzed
- The analyzed data accounted for 10 percent of patients worldwide
- The patients were starting antihypertensive therapy with a single drug
- The algorithm used identified the following parameters:
- Heart attacks
- Strokes
- Hospitalizations due to heart failure
- 50 side effects of any of the first-line antihypertensive drugs
- Several techniques were used to minimize bias for approximately 60,000 variables
Study Findings
- ACE inhibitors were the most popular first-line antihypertensive drugs, prescribed to 48 percent of patients
- Thiazides were prescribed as first-line antihypertensive therapy to only 17 percent of patients
- Patients who received thiazides had 15 percent fewer cardiovascular events than those who received other first-line therapies
- Patients who first received ACE inhibitors had higher rates of 19 side effects compared to those who received thiazides first
- Non-dihydropyridine calcium channel blockers were the least effective among all first-line antihypertensive drugs
- 3,100 major cardiovascular events could have been averted if thiazides were prescribed as a first-line drug instead of ACE inhibitors
Concluding Remarks
“With LEGEND, we have found a way to fill in the gaps left by randomized, controlled trials and help guide physicians in their clinical decision making,” says Hripcsak.Funding Source
The study was funded by the US National Science Foundation, the National Institutes of Health, the Australian National Health and Medical Research Council, Janssen Research & Development, and IQVIA, a Consultancy Company headquartered in Durham, North Carolina, USA.Reference:
- Comprehensive Comparative Effectiveness and Safety of First-line Antihypertensive Drug Classes: A Systematic, Multinational, Large-scale Analysis - (https://doi.org/10.1016/S0140-6736(19)32317-7)
Source-Medindia