Antibiotics used early in elderly patients with urinary tract infection (UTI) reduce the risk of sepsis and death. Therefore, antibiotics should be prescribed immediately in elderly UTI patients.
- Antibiotics should be prescribed immediately in elderly patients with urinary tract infection (UTI)
- If the prescription of antibiotics is delayed, it can result in sepsis and even death
- Antibiotics used early can save the lives of many elderly patients with UTI
The study, published in the British Medical Journal (BMJ), was led by Professor Paul Aylin, MBChB, FFPH, FRCPE, who is a Professor of Epidemiology and Public Health in the Faculty of Medicine, School of Public Health at Imperial College London, UK
Professor Alan Johnson, PhD, who is the Head of the Department of Healthcare-Associated Infection and Antimicrobial Resistance at Public Health England, London, UK was Professor Aylin’s collaborator.
The lead author of the study was Dr. Myriam Gharbi, MPH, PhD who is an Honorary Research Associate at the Department of Medicine, Imperial College London, UK.
Read More..
Prescribing Antibiotics for UTIs in the Elderly: A Major Dilemma
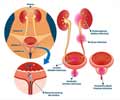
Urinary tract infection (UTI) is an infection in any part of the urinary system, including the kidneys, urinary bladder or urethra. Bladder and urethral infections cause pelvic pain, increased urge to urinate, painful urination and blood in the urine (hematuria).UTIs are caused by bacteria such as Escherichia coli (E. coli), which particularly attack the elderly, and if untreated, may cause blood poisoning or sepsis. UTIs are the second most common infections that require antibiotic therapy in the UK. However, due to the dramatic rise in antibiotic resistance worldwide, there is a dilemma about whether to prescribe antibiotics or delay prescribing or not prescribe at all.
In this regard, Gharbi says: “Current national guidelines for GPs recommend they should ask patients about the severity of their symptoms, discuss possible self-care, such as drinking plenty of water to avoid dehydration and taking paracetamol or ibuprofen for pain relief, and consider a back-up antibiotic prescription to be used if symptoms worsen or have not improved after 48 hours. This is to avoid antibiotic overuse, as sometimes UTIs can get better without medication. However, our research suggests antibiotics should not be delayed in elderly patients.”
Study Procedure
- The study was conducted between 2007 and 2015
- Patient data were accessed from the Clinical Practice Research Datalink (CPRD), which is a repository of de-identified patient data from GPs, linked to hospital records throughout the UK, which enables efficient tracking of patients across the health system
- Medical records of 157,264 patients aged above 65 years (average age: 77 years) across England were analyzed
- The analysis took into account all available information about age, gender, pre-existing illnesses and other personal characteristics
- The patients had been diagnosed with suspected or confirmed UTI by their GP
- With reference to antibiotic prescriptions, the patients were stratified into the following three categories:
- Antibiotics Prescribed Immediately – 87 percent of cases
- Antibiotics Delayed up to 7 Days – 6 percent of cases
- No Antibiotics Prescribed – 7 percent of cases
Study Findings
- About 0.2 percent of patients who received antibiotics immediately, developed sepsis within 60 days
- Patients in whom antibiotics were delayed or didn’t receive antibiotics, were 8-times more likely to develop sepsis within 60 days
- 1.6 percent of patients who received antibiotics immediately, died within 60 days
- Patients in whom antibiotics were delayed, had a 16 percent risk of death within 60 days
- Patients who didn’t receive antibiotics had over double (> 32%) the risk of death compared to those in whom antibiotics were delayed
- For every 37 cases who didn’t receive antibiotics or for every 51 cases where antibiotics were delayed, one case of sepsis occurred, which was absent in the group that received antibiotics immediately
- Hospital admission rates were roughly half (15%) in the group that received antibiotics immediately than the groups that either didn’t receive antibiotics or antibiotics were delayed (27%)
- Older men (> 85 years) and those who were underprivileged had the highest risk
Concluding Remarks
It may be concluded that a delay in antibiotic therapy is associated with sepsis and death in elderly patients with UTI. However, it is speculated that there may have been additional health conditions, which couldn’t be accounted for due to unavailable data, but which, nevertheless, might have increased the risk of sepsis and death.With reference to antibiotic use in the study population, Aylin says: “Although antibiotic prescribing must be controlled to help combat the increasing problem of antibiotic resistance, our study suggests early use of antibiotics in elderly patients with UTIs is the safest approach.”
Johnson sums-up: “Antibiotic resistance is a major threat to public health that is being driven by the overuse of antibiotics. Current recommendations suggest healthcare professionals take a number of different factors into account when deciding whether to prescribe antibiotics immediately or consider deferring antibiotics for patients with a suspected UTI. This study highlights the importance of taking age into account when making clinical decisions about antibiotic prescribing in order to reduce the risk of complications. This work will help doctors target antibiotic use more effectively and improve patient wellbeing.”
Funding Source
The study was funded by the National Institute for Health Research Health Protection Research Unit (NIHR HPRU) in Healthcare Associated Infections and Antimicrobial Resistance at Imperial College London in partnership with Public Health England (PHE), UK.Reference:
- Delaying Antibiotics in Over 65s with UTI May Increase Risk of Sepsis - (https://doi.org/10.1136/bmj.l922)
Source-Medindia