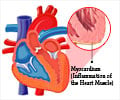
Polypills or combination pills help lower both blood pressure and cholesterol. A new study reveals that taking one polypill daily can also lower the risk of heart attack and stroke in patients living in areas with limited access to healthcare.
Highlights:
- Combination pills or polypills contain agents that lower both blood pressure and cholesterol and need to be taken only once daily
- Polypills are also effective in reducing heart disease risk in patients living in areas with limited access to healthcare
- Persons given polypills had a 25% lesser risk of heart attack and were also more compliant with the one daily dosing compared to those on regular medications
The study was undertaken at the Vanderbilt University Medical Center, Nashville, Tennessee and funded by the American Heart Association.
The findings of the study appear in the prestigious journal New England Journal of Medicine.
TOP INSIGHT
Persons given polypills are 25% lesser risk of developing a heart attack compared to persons given normal medications. Such novel measures can help reduce the risk of serious heart disease in persons with limited access to health care.
Read More..
Improving Healthcare of Populations With Limited Access to Healthcare
The aim of the study was to find ways and means of improving heart health and reducing risk of serious events such as heart attack and stroke of populations living in rural communities and remote locations with limited access to healthcare."Patients face a variety of barriers to getting the care they need," says study author Daniel Muñoz, M.D, M.P.A., assistant professor of cardiology at Vanderbilt University Medical Center, Nashville, Tennessee. "Those barriers can include cost and complexity of medication regimens, so innovative strategies are needed to improve the delivery of preventive care, especially when it comes to socio-economically vulnerable individuals."
Testing the Efficacy of Polypills in Improving Heart Health
- The study team looked at polypills containing a combination of four medicines that decrease blood pressure as well as low-density lipoprotein (LDL) cholesterol in patients with hypertension and dyslipidemia in a rural health center in Mobile, Alabama
- Of the 303 patients studied, nearly 75% reported earning less than $15,000 a year; 96% of the participants were black; the average age of the participants was 56 and 60% were women
- One group of patients (50%) were given the polypill that contained a combination of four medicines in low dose to lower blood pressure and/or LDL cholesterol: amlodipine (2.5 mg), atorvastatin (10mg), losartan (25 mg) and hydrochlorothiazide (12.5 mg)
- The second half of patients were given standard care and regular medications
- Doctors measured patients' blood pressure and serum cholesterol at the start of the study, at two months and finally after one year
- Patients taking the polypills had larger reductions in systolic blood pressure and levels of LDL cholesterol compared to those in the standard care group
- In the polypill group, the average reduction of systolic blood pressure was 9 mm Hg compared 2 mm Hg in the usual care group at the end of one year
- LDL cholesterol reduction in the polypill on an average was 15 mg per deciliter versus 4 mg per deciliter in the standard care group
- These readings translate to a 25% lower risk of suffering a heart attack or stroke
- Compliance to medication over the 12-month study period was significantly higher (86%) in the polypill group, compared to less than 50% of patients on standard blood pressure medicines at one year
Scope of Study
Study offers simple and easy to implement measures to reduce heart attack or stroke poor and vulnerable populations. The efficacy of the polypill can also be studied in the general population.Strategically Focused Research Network for Prevention
The current study was part of $15 million initiative by the American Heart Association in four study teams --Vanderbilt University Medical Center, University of Texas Southwestern Medical Center, Icahn School of Medicine at Mount Sinai, and Northwestern Medical Center. It started in July 2014 with the aim of finding novel ways to prevent or reduce heart attack and stroke in the population.In summary, combination pills or polypills containing four drugs in low doses is effective in lowering blood pressure and cholesterol and also patients are more adherent to their medications. Such simple measures will ensure optimal health of rural and other populations with poor healthcare access.
Reference:
- Polypill for Cardiovascular Disease Prevention in an Underserved Population - (https://www.nejm.org/doi/10.1056/NEJMoa1815359)
Source-Medindia
 MEDINDIA
MEDINDIA

 Email
Email