- Water Resource, Hygienic Practice, and Soil Transmitted Helminthiasis in Some Rural Communities of Osun State, Nigeria - (https://www.scirp.org/(S(351jmbntvnsjt1aadkposzje))/reference/ReferencesPapers.aspx?ReferenceID=1968288)
- Hookworm - The Great Infection of Mankind - (https://journals.plos.org/plosmedicine/article?id=10.1371/journal.pmed.0020067)
- Brooker S, Bethony J, Hotez PJ. Human hookworm infection in the 21st century. Adv Parasitol. 2004;58:197–288.
- Pullan RL, Smith JL, Jasrasaria R, Brooker SJ. Global numbers of infection and disease burden of soil transmitted helminth infections in 2010. Parasit Vectors. 2014;7:37.
- Jourdan PM, Lamberton PH, Fenwick A, Addiss DG. Soil-transmitted helminth infections. Lancet. 2018;391:252–65.
- Hookworm infection - (https://en.wikipedia.org/wiki/Hookworm_infection)
- Soil-transmitted helminth infections - (https://pubmed.ncbi.nlm.nih.gov/28882382/)
- Ancylostoma ceylanicum, a re-emerging but neglected parasitic zoonosis - (https://pubmed.ncbi.nlm.nih.gov/23968813/)
- Traub RJ. Ancylostoma ceylanicum, a re-emerging but neglected parasitic zoonosis. Int J Parasitol. 2013;43:1009–15.
- Hookworm FAQs - (https://www.cdc.gov/parasites/hookworm/gen_info/faqs.html)
- Hookworm Intestinal - (https://www.cdc.gov/dpdx/hookworm/index.html)
- Hookworm Treatment - (https://www.cdc.gov/parasites/hookworm/treatment.html)
- Hookworm (Intestinal) - (https://www.cdc.gov/dpdx/hookworm/index.html)
- About Hookworm infection - (https://medlineplus.gov/ency/article/000629.htm)
What is Hookworm Infection?
Hookworm infection is the result of a parasitic roundworm that lives in the small intestine of birds or mammals. These are blood-feeding worms cause one of the most neglected tropical disease called hookworm disease.
Hookworm infestation is common in tropical and subtropical climates. It affects nearly 500 million people in tropical regions of South America, Africa and Asia.(1✔ ✔Trusted Source
Water Resource, Hygienic Practice, and Soil Transmitted Helminthiasis in Some Rural Communities of Osun State, Nigeria
Go to source). Children are especially at risk as they often play barefoot. Hookworm infection during pregnancy can retard the growth of the fetus, and result in premature birth or low birth weight. Hookworms may also cause intellectual, cognitive and physical growth problems in small children.(2✔ ✔Trusted Source
Hookworm - The Great Infection of Mankind
Go to source)
It is estimated that ‘Hookworm disease’ results in four million disability-adjusted life years (DALYs) and up to USD139 billion annual economic productivity losses.(3✔ ✔Trusted Source
Soil-transmitted helminth infections
Go to source)
What are the Symptoms of Hookworm Infection?
Symptoms of hookworm infection are usually general and most patients remain asymptomatic or manifesting with symptoms of intestinal inflammation, protein deficiency and iron-deficiency anemia.(4✔ ✔Trusted Source
Ancylostoma ceylanicum, a re-emerging but neglected parasitic zoonosis
Go to source) Chronic iron-deficiency anemia can affect all age groups but it is particularly makes children and pregnant women who have low iron stores more prone to severe disease.
Presentation of the hookworm infection depends upon the stage of the disease i.e., early or late. They include:
Symptoms of the lungs: Usually occur after 1 week of exposure
- Wheezing
- Pneumonitis
- In rare cases, severe infections may give rise to Löffler syndrome, characterized by paroxysmal attacks of a cough, dyspnea, pleurisy, little or no fever and eosinophilic pulmonary infiltrates that last several weeks after the initial infection
- Cough

Skin disease: Usually occurs after 1 -2 week of cutaneous infection
- Itching
- Pale skin, rashes
- Creeping eruption or cutaneous larvae migrans
Intestinal symptoms due to eosinophilic enteritis: These are common with initial exposures and peak between 30 – 45 days after exposure to the infection.
- Indigestion
- Abdominal pains
- Constipation that changes into diarrhea
- Nausea and vomiting
- Emaciation – Extreme weight loss and loss of adipose tissue or fat under the skin
- Abdominal distension with ascites
Symptoms of the eye:
- The worms migrate to the eye and cause Diffuse Unilateral Subacute Neuroretinitis (parasitic disease affecting the retina).
- Vitritis (inflammation of the vitreous body).
- Consecutive crops of multiple, evanescent retinal lesions.
- Visual loss.
- The condition may progress to retinal arterial narrowing, optic atrophy and electroretinographic changes.
Other symptoms:
- Cardiac failure in severe cases.
- Slow physical and cognitive growth.
- Hypoproteinemia (low level of protein in the blood) leading to peripheral edema.
- Symptoms of infections such as fever, wheezing, chest pain.
- When the infection is long term, it can cause iron deficiency and anemia presenting with pallor, chlorosis (greenish-yellow skin discoloration), hypothermia, spooning nails and tachycardia.
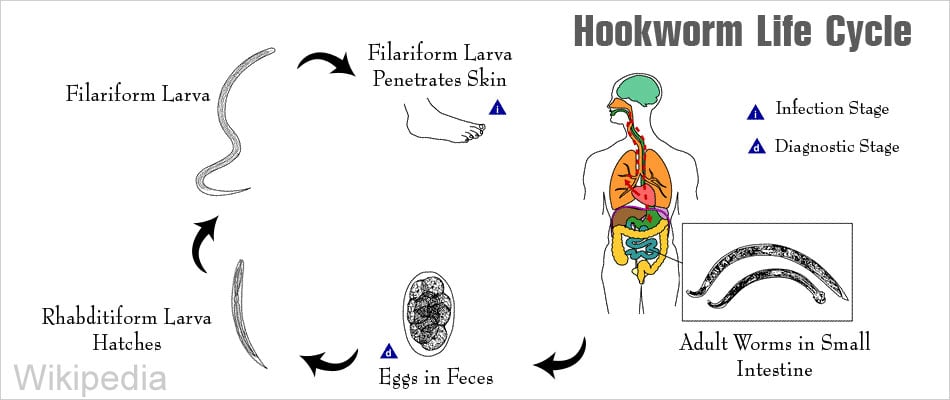
Hookworm Life Cycle
Hookworm spreads from an infected person to others when the eggs of the hookworms are passed along with feces of the person. When the weather is moist, warm and shady, the larvae hatch out of the eggs and grow in the soil. By about 5 to 10 days, they become ready to infect another animal, though these immature worms can survive 3 to 4 weeks in the soil.(5✔ ✔Trusted Source
Hookworm (Intestinal)
Go to source)
These immature worms are transmitted to humans from the soil to the skin, when the children touch the soil or a person walks on the soil barefoot. Sometimes, the soil may be ingested accidentally when the vegetables grown out of it are not washed properly. The larvae reach the bloodstream via the skin to be carried to the lungs and through the mouth to the intestine. The blood carries the larvae to the lungs, where they enter into the air sacs. The hookworms then crawl up the breathing tubes to the throat, where they are swallowed. The larvae pass through the stomach and mature into adult worms in the bowel.
The skin invasive larvae of Ancylostoma duodenale spread around the body via the blood stream and settle down inside muscle fibers in dormant condition. They then re-enter the blood circulation under favorable conditions.
On reaching the small intestine, the larvae mature into half-inch long worms. The adult hookworm attaches to the intestinal wall with its sharp buccal teeth. It tears open the blood vessels of the intestinal walls to feed on the blood. They secrete anticoagulant substances that prevent clotting of the blood so that they can continue to feed on them.
They mate and produce about 5000 to 10000 eggs at a time, which are passed outside via feces of the human host.
During pregnancy, they enter the umbilical cord and reach the fetus. After the childbirth, the larvae pass to the mammary glands to contaminate the mother’s milk, passing on the infection to the newborn baby.
What are the Causes of Hookworm Infection?
Hookworm is generally caused by unhygienic environmental conditions and habits. Hookworm eggs are passed on to the soil by the feces of the infected person or animals like dogs and cats. The eggs in the feces contaminate the soil from where they can be ingested or get into the host via their skin. The eggs or larvae can spread by –
Skin:
- Walking barefoot in contaminated soil
- Touching the contaminated soil in the fields, for example while weeding or cleaning up
- Bathing in the water body into which sewage is disposed
- Contact with sewage water by workers or during rains
- Lying on beach sand that is contaminated by infected feces

Direct ingestion:
- When animals such as pet dogs eat the weeds or leftovers from the contaminated soil.
- Eating raw food such as fruits and vegetables without washing properly.
- Ingestion of food with contaminated hand, after playing in the contaminated soil.
Hookworms grow well in warm, tropical or sub-tropical environments. Pregnant women, pre-school and school-age children, farmers and sanitation workers are at high risk for getting hookworm infection.
How Do You Diagnose Hookworm Infection?
- Hookworm infection is confirmed with a microscopic examination of the stool to look for ova and parasites in the person who is seen to manifest symptoms of hookworm infection.
- Complete blood count to check for anemia and differential count to look for eosinophilia will be done to evaluate the level of infection. High white blood cell count indicates the presence of infection.
- Specific diagnosis with PCR (polymerase chain reaction) can be employed to confirm hook worm infection.
- Rarely, endoscopy is done that would reveal the presence of adult worms in the intestine. This is done for the purpose of identification of the species that has infected the person.
- Chest X- ray is done to check lung involvement in hookworm infection.
How Do You Treat Hookworm Infection?
Treatment of hookworm infection involves the following:
Cure the infection
Drugs like mebendazole are currently used to destroy the adult hookworms in the intestine and albendazole is effective in treating the disease while the worm is in the intestine or in the skin. Other antihelminthic drugs include levamisole and pyrantel pamoate.

Medicines prescribed for pregnant and lactating women would differ according to the sensitivity of the drug and severity of the infection.
Thiabendazole is applied topically to destroy the larvae in the skin. Local cryotherapy is used to destroy the hookworms while the parasite is still in the skin, causing itching and rashes.
Two weeks after completion of the treatment, stool examination should be repeated.
Treatment of anemia and its complications
Anemia must be treated immediately with iron supplements, accompanied by vitamin C. Folic acid and vitamin B12 supplements are also recommended.
Improve nutrition for the patient
Hookworm grows in the intestine and absorbs nutrients for its growth. This in turn affects the human host harboring the worm and develops deficiency of nutrients. There may be a rapid weight loss and deterioration in the health.
Diet for a patient with hookworm infection must include the following components.
- Iron
- Protein
- Fiber
- Vitamin C
- Folic acid
- Vitamin B12
Hookworm Infection Prevention
Prevention of hookworm infection can be done in the following ways:
Improving hygiene in the society:
- Improving the sanitation of the area where the hookworm infection is prevalent.
- Improving socioeconomic conditions and educating people about the disease.
- Conducting school-based or community-based deworming programmes.
- Pets like cats and dogs must be dewormed periodically.
- Providing adequate clean drinking water and tap water for other uses.
- Not using human excreta or raw sewage as fertilizer in agriculture.
- Employing effective sewage disposal systems prevent transmission of the infection.
- Making footwear available and accessible for the people of the area.

Improving personal hygiene:
- Do not defecate in the open, use toilets.
- Wash hands before eating.
- Stay away from water bodies contaminated by human feces.
- Improve your health through nutrition.
Screening programmes for High-Risk groups:
Screening programmes can be held to identify hookworm infection in a particular community or locality. The World Health Organization identifies the following high-risk categories:
- Pre-school and school-aged children
- Women of the childbearing age
- Pregnant women, especially those in the 2nd and 3rd trimesters
- Lactating women
- Farmers and their family
- Sanitation workers
Mass-Drug administration:
Periodical mass drug administration can be conducted in high-risk communities. The drugs are distributed door-to-door as they are safe to be used. Most often, these drugs are inexpensive or may be sponsored by a company or social groups.
Health Tips
- Wear proper footwear while going out.
- Wash your hands with soap and clean water before eating any kind of food.
- Avoid having raw salads while eating out or at a gathering.
- Deworm pet dogs and cats periodically.
- Discourage the habit of defecating in the open.
- Maintain hygienic conditions in and around the house.
- Wash all raw foods properly before eating.

 MEDINDIA
MEDINDIA
 Email
Email