- What is Buruli ulcer? - (http://www.dermnetnz.org/bacterial/buruli.html)
- Buruli ulcer endemic countries - (https://www.who.int/buruli/country/en/)
- Buruli ulcer - Wikipedia - (https://en.wikipedia.org/wiki/Buruli_ulcer)
- Buruli ulcer (Mycobacterium ulcerans infection) - (https://www.who.int/en/news-room/fact-sheets/detail/buruli-ulcer-mycobacterium-ulcerans-infection)
- Buruli Ulcer: A Systemic Disease - (https://academic.oup.com/cid/article/37/6/e78/300951)
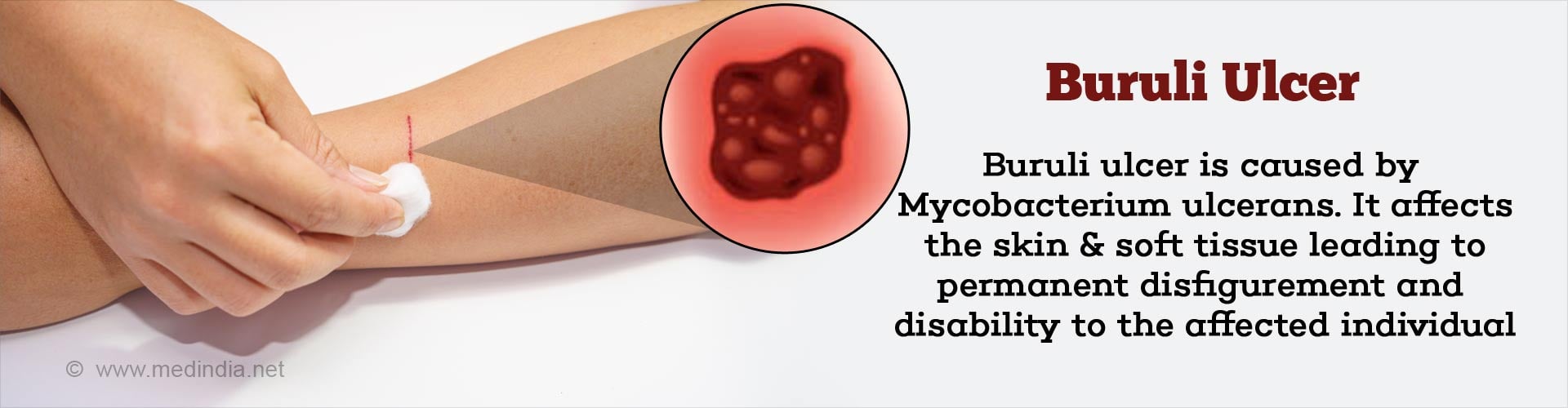
What is Buruli Ulcer?
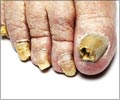
Buruli Ulcer, caused by Mycobacterium ulcerans, affects the skin and soft tissue leading to permanent disfigurement and disability to the affected individual. This necrotizing disease of the skin begins with a painless nodule on the skin or under the skin. Over a period of two weeks, it breaks down to form a necrotic ulcer with undermined edges. The ulcer may be larger under the surface of the skin and is surrounded by swelling.
As the disease progresses, bones are also infected, resulting in the necrosis (death of tissue) of bones.
The other names of Buruli ulcer are:
- Bairnsdale ulcer
- Daintree ulcer
- Mossman ulcer
- Searl ulcer
What are the Causes of Buruli Ulcer?
Burili ulcer is caused by Mycobacterium ulcerans, a member from a family of bacteria that causes tuberculosis and leprosy.
Transmission of M. ulcerans is not fully understood, though it is found to occur in those who are in close proximity to water. The infective agent may enter the body through a traumatic wound.
The organism produces a toxin called mycolactone that suppresses immune system and causes tissue death. The necrosis occurs without any initial inflammation or systemic symptoms like fever or pain.
The primary site of infection is the fat under the skin. The bacteria attack the fat and accumulate into groups of spherules within the dead cells. Skin ulceration takes place only after dramatic tissue death under the skin. These may further progress to granulation, scarring and contractures. The infection may also spread into the bone tissues.
What are the Symptoms and Signs of Buruli Ulcer?
- Buruli ulcer initially presents as a painless nodule under the skin, around 1 to 2 cm in diameter.
- Tissue destruction takes place around the nodule, without any systemic symptoms such as fever or lymph node enlargement.
- This nodule then breaks down to form a painless ulcer. The destruction of tissues (necrosis) extends several centimeters beyond the edges of the ulcer.
- The ulcer extends down into deeper tissues and destroys muscles, blood vessels, nerves and bone.

The extent of destruction caused by Buruli ulcer does not surface up until the tissues are really damaged. It is important that the ulcer is examined on time to help in proper diagnosis.
How to Diagnose Buruli Ulcer?
- Based on clinical findings in endemic areas
- Microscopic examination of smear taken from the necrotic base reveals the Mycobacterium
- Polymerase chain reaction (PCR) testing on swabs of ulcers or tissue biopsies
- Biopsy of the lesion
What are the Treatments for Buruli Ulcer?
Treatment of Buruli ulcer is done with various antibiotics including:
- Rifampicin
- Streptomycin
- Amikacin
- Clarithromycin
- Moxifloxacin

Rifampicin is either combined with streptomycin, clarithromycin or sometimes moxifloxacin and is prescribed for 8 weeks. Use of antibiotics for Buruli ulcer helps heal smaller lesions and also prevents relapse of the disease. Lesions less than 5 cm are seen to respond well to antibiotics given for eight weeks as a first-line treatment.
Surgery is done to remove the necrotic tissue. Debridement of necrotic tissue improves the rate of wound healing and prevents further deformity. Surgery must be aimed at conserving the existing healthy tissues around the scar. Skin grafting is done after debridement.
Heat therapy can be used in combination with medicines or when antibiotics are contraindicated. Heat delivered using servo-controlled heating coils or hot-air delivery systems have been used in the past.
Suitable rehabilitation is provided for the individual who has suffered extensive disabilities due to Buruli ulcer.
Bacillus Calmette-Guerin (BCG) vaccine has shown to provide temporary protection against Mycobacterium ulcerans.
Prognosis of Buruli Ulcer
Buruli ulcer can be completely healed in most patients. The extent of damage done to the tissues however, cannot be reversed. WHO reports that nearly 80% of cases that are detected early can be cured with a combination of antibiotics.
Medical and surgical interventions take a long time, sometimes as much as 3 months of hospitalization. Further, rehabilitation in the form of using the limbs and counseling requires further time.
Health Tips
- People living in endemic areas must wear protecting clothing and boots to reduce the risk of contamination.
- Frequent cleaning and washing of areas of skin or wounds exposed to soil is recommended.
- During outbreaks, BCG vaccine is given as it seems to offer temporary protection.
- Never ignore a long-standing painless ulcer. It has to be checked and treated immediately.
 MEDINDIA
MEDINDIA
 Email
Email