More than 80 wrong side error (WSE) incidents were reported across 100 hospitals in Spain over the past decade, revealed new research.
TOP INSIGHT
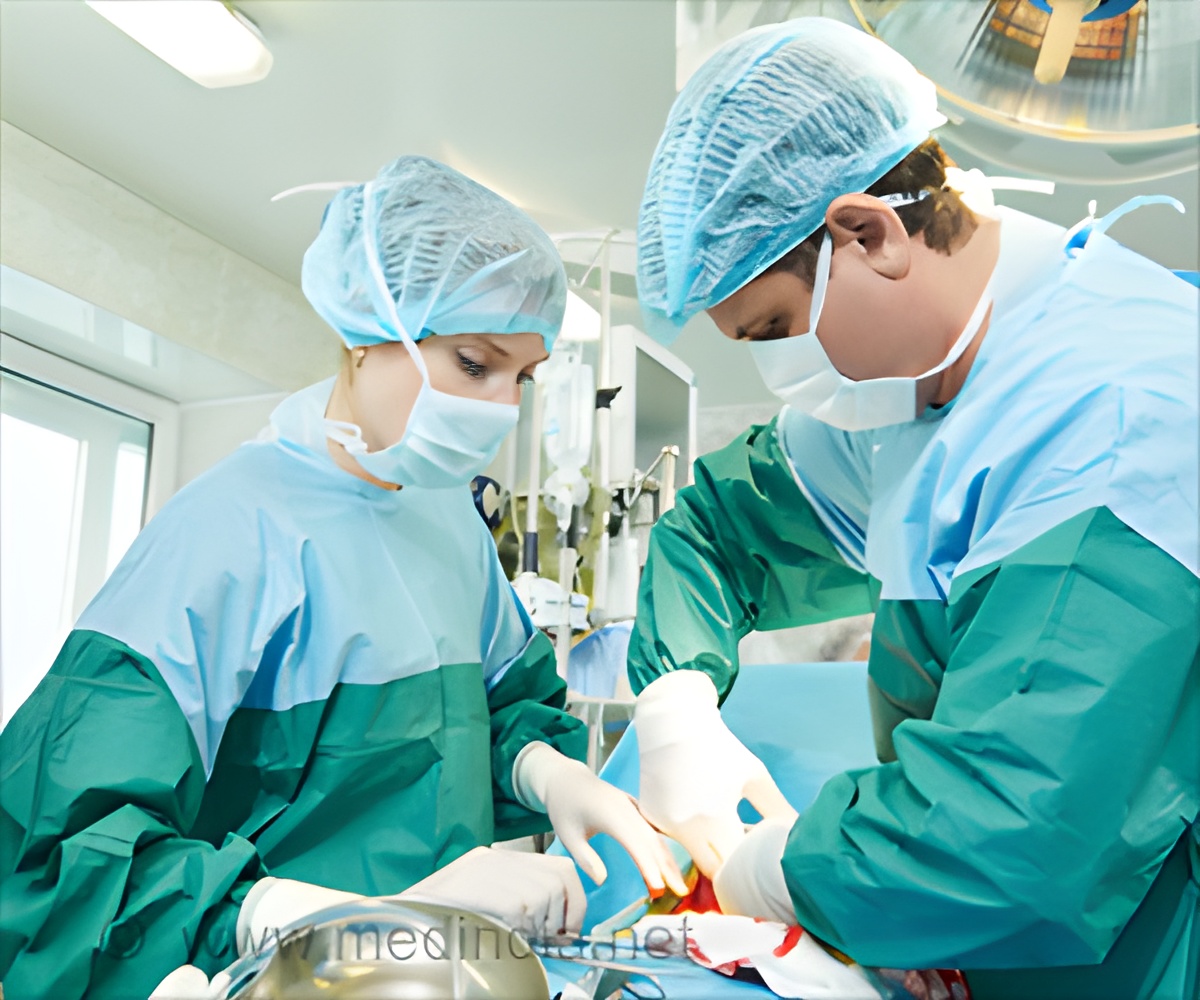
Performing a procedure on the wrong side of a patient's body, although rare, may be more common than generally thought.
Although wrong side errors seem preventable, they continue to occur. Previous studies have estimated 1 wrong side surgery per 100,000 procedures and 1.3 wrong-side nerve blocks per 10,000 procedures [1].
To provide more information on how often and why they occur, and on the safety mechanisms needed to prevent them, Arnal and colleagues analysed WSE incidents reported to SENSAR (Spanish Safety Reporting System in Anaesthesia and Resuscitation), which covers 100 predominantly large hospitals across Spain between 2007 and 2018.
Overall, 81 incidents were reported in 11 years, with high numbers of WSEs noted in orthopaedic (48%) and ophthalmology (28%) surgery.
36 (44%) of these WSEs were related to the surgical procedure, and the surgery was actually performed in half of these cases. The remaining 45 (56%) WSEs involved the anaesthetic technique (the wrong side of the the body given anaesthesia), with an incorrect nerve block performed in 91% of cases. Severe harm was caused on three occasions.
"Our findings highlight the need for adequate training and appropriate use of surgical check-lists, as well the creation of a standardised surgical site marking protocol, the correct revision of clinical history and imaging tests, and involving patients in their own safety", says Dr Arnal. "While these serious wrong side events are extremely rare, our mission should be to drive them down to zero."
 MEDINDIA
MEDINDIA



 Email
Email




