A wide variation has been found in the use of minimally invasive surgery at hospitals across hospitals in the United States, found in a study published on the bmj.com on Tuesday.
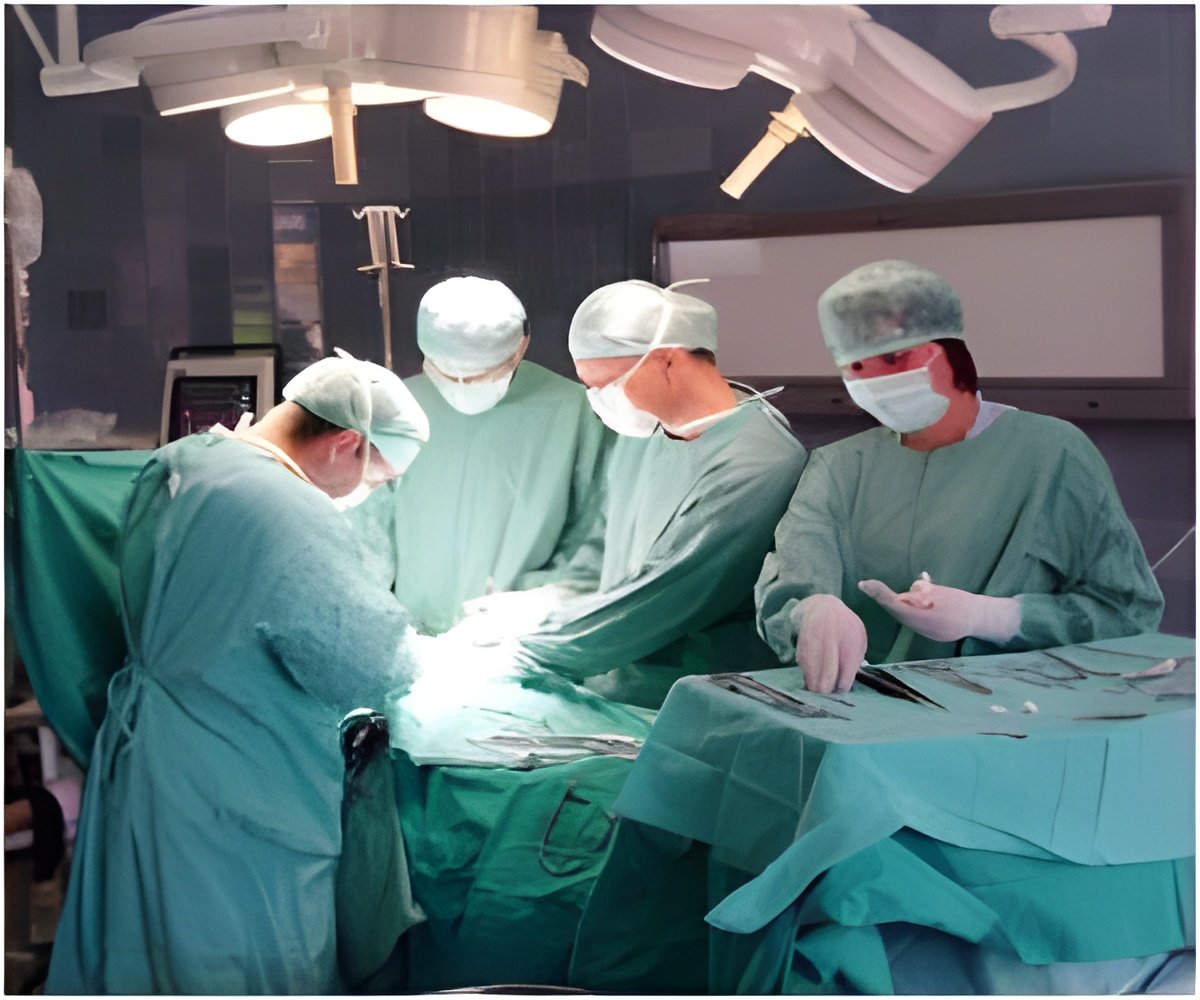
Surgical complications represent a substantial burden of harm to patients and in the United States alone are estimated to cost $25b annually. For some procedures, however, complications can be reduced by using minimally invasive surgery rather than traditional open surgery.
Despite this, hospitals may only offer and surgeons may only perform open surgery, so many patients who are candidates for minimally invasive surgery will undergo open surgery instead.
So a team of researchers based at Johns Hopkins University in the United States set out to investigate levels of variation in the use of minimally invasive surgery across the US and to measure this potential disparity in surgical care.
They calculated use of minimally invasive surgery for four common surgical procedures (appendectomy, colectomy, hysterectomy, and lung lobectomy) at over 1000 hospitals across the United States in 2010.
Levels were adjusted for case-mix (differences in a hospital's unique patient population), and for each procedure a model was used to calculate the predicted proportion of minimally invasive operations for each hospital based on patient characteristics.
Average hospital use of minimally invasive surgery was 71% for appendectomy 28% for colectomy, 13% for hysterectomy and 32% for lung lobectomy. Surgical complications were less common with minimally invasive surgery compared with open surgery for each procedure.
Some hospitals never used minimally invasive surgery for some of the four procedures, while others used minimally invasive surgery for more than 75% of these procedures.
Urban hospitals were more likely to perform minimally invasive surgery for three of the four procedures, but other hospital characteristics, such as size and geographic region, showed no association or an irregular pattern of association with use of minimally invasive surgery.
"Hospital use of minimally invasive surgery for these four common procedures varies widely in the United States, representing a disparity in the surgical care delivered nationwide," says Dr Martin Makary, a Johns Hopkins Professor of surgery and senior author of the study.
"This disparity in appropriateness of operations offered between hospitals has important implications for training, informed consent, and patient empowerment through data transparency," he and his team conclude.
Source-Eurekalert
 MEDINDIA
MEDINDIA
 Email
Email