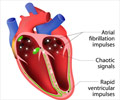
Guidelines presented in The Journal of Thoracic and Cardiovascular Surgery offer evidence-based clinical recommendations, including hybrid procedures.
TOP INSIGHT
Clinical practice regarding surgical ablation of atrial fibrillation varies widely. This consensus statement should guide surgeons to provide the best therapy for their patients who have atrial fibrillation.
"These guidelines are extremely important for a few reasons," stated lead author Niv Ad, MD, Professor of Surgery, Division of Cardiothoracic Surgery, West Virginia University School of Medicine, Morgantown, WV. "This consensus statement demonstrates the safety of the procedure and the clear association with reduced early death compared to patients who were left with atrial fibrillation. It also clearly states that there is a reduction in late stroke and better long term survival with improved quality of life."
"Clinical practice regarding surgical ablation of atrial fibrillation varies widely. This consensus statement should guide surgeons to provide the best therapy for their patients who have atrial fibrillation," added co-author Marc Gillinov, MD, Department of Thoracic and Cardiovascular Surgery, The Cleveland Clinic, Cleveland, OH.
The guidelines offer a robust look at many facets surrounding surgical ablation and begin with morbidity, stroke risk, and quality of life outcomes for atrial fibrillation patients. For example, investigators found that concomitant surgical ablation for atrial fibrillation improves 30-day operative mortality, so it is recommended to be performed when indicated.
The recommendations also note that ablation does not increase the risk of periprocedural morbidity or early stroke/transient ischemic attack (TIA) and that late stroke/TIA is decreased by surgical ablation in a follow up longer than one year. Other topics covered include indications for off pump hybrid procedures, the recommended surgical ablation devices that are associated with reliable transmural lesions, and the importance of standardized surgeon training and education.
"It was a pleasure to participate in putting together this important document, which represents a significant contribution to the field of surgical atrial fibrillation ablation," remarked co-author Hugh Calkins, MD, Director of the Cardiac Arrhythmia Service, and Professor, Division of Cardiology, Department of Medicine, Johns Hopkins University School of Medicine, Baltimore, MD.
 MEDINDIA
MEDINDIA


 Email
Email