Critical access hospitals (CAHs) recorded higher rates of hospital transfers after surgery though the percentage of patients who used post acute care was similar.
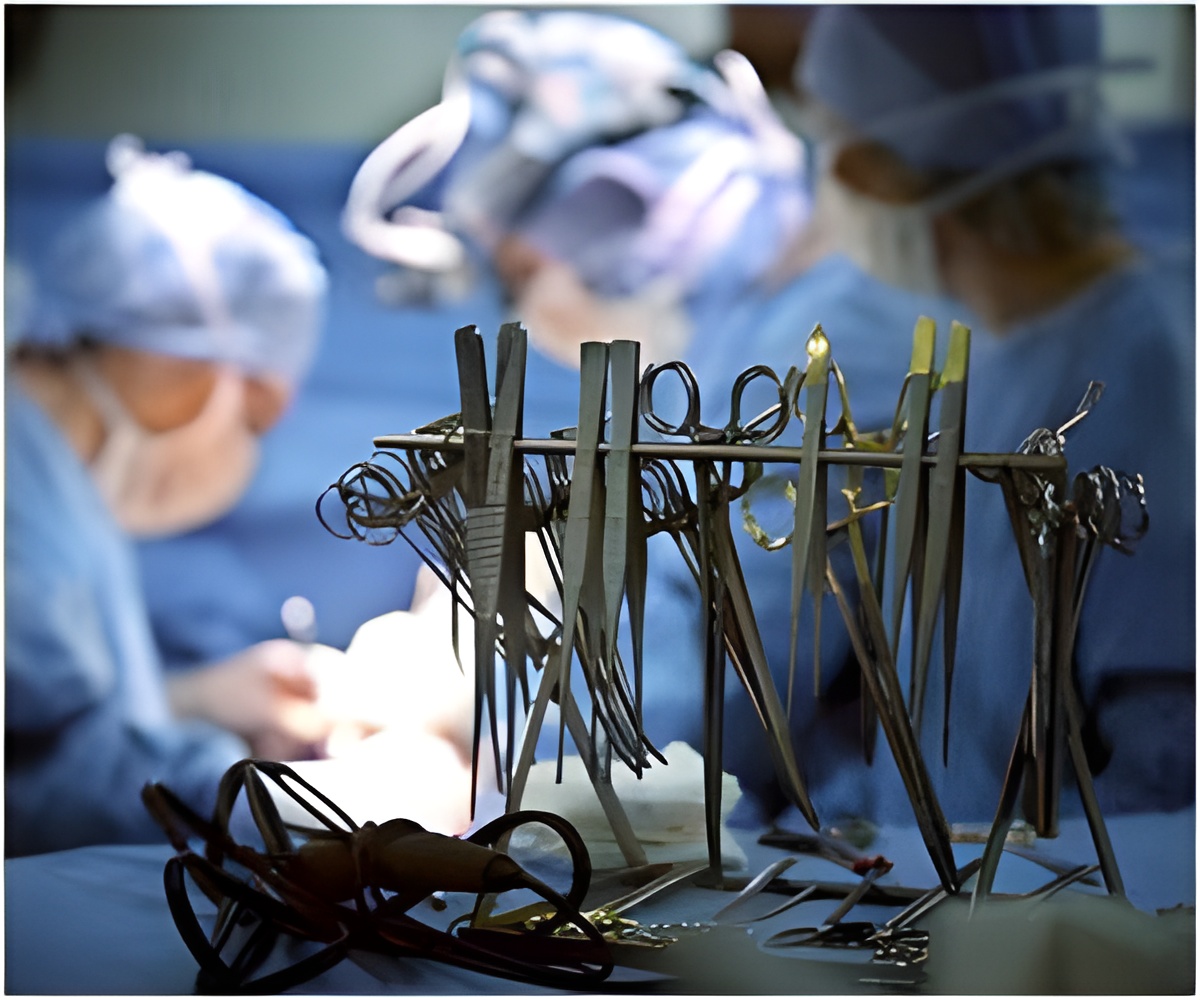
The authors used data from the Nationwide Inpatient Sample and the American Hospital Association to examine patients undergoing six common surgical procedures (hip and knee replacement, hip fracture repair, colorectal cancer resection, gall bladder removal and transurethral resection of the prostate [TURP]) at CAHs or non-CAHs. The authors measured hospital transfer, discharge with post-acute care or routine discharge. The authors identified 4,895 acute-care hospitals reporting from 2005 through 2009: 1,283 (26.2 percent) of which had a CAH designation.
For each of the six inpatient surgical procedures, a greater proportion of patients from CAHs were transferred to another hospital (after adjustment for patient and hospital factors), ranging from 0.8 percent for TURP to 4.1 percent for hip fracture repair for CAH patients and from with 0.2 percent and 1.2 percent for the same procedures, respectively, for non-CAH patients. However, patients discharged from CAHs were less likely to receive post-acute care for all but one of the procedures (TURP) examined. The likelihood of receiving post-acute care ranged from 7.9 percent for gall bladder removal to 81.2 percent for hip fracture repair for CAH patients and from 10.4 percent to 84.9 percent, respectively, for non-CAH patients. The authors note there must be future work to define the causes for the disparity in transfer rates.
"These results will affect the ongoing deliberations concerning CAH payment policy and its implications for health care delivery in rural communities."
Author: Adam J. Gadzinski, M.D., M.S., of the University of Michigan Health System, Ann Arbor, Mich., and colleagues.
(JAMA Surgery. Published online May 14, 2014. doi:10.1001/jamasurg.2013.5694)
Commentary: The Right Triangle
"There remains no obvious mechanism to ensure the financial viability of individual CAHs, particularly in the era of the integrated health care delivery system. Medicare will probably have to continue subsidizing these hospitals to maintain broad access to financially unsuccessful service lines; the challenge will be to keep the quality and cost corners of the triangle from growing too obtuse or acute."
(JAMA Surgery. Published online May 14, 2014. doi:10.1001/jamasurg.2013.5707.)
Editor's Note: Please see the article for additional information, including other authors, author contributions and affiliations, financial disclosures, funding and support, etc.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email