About
PSA blood test is specific to prostate gland; it is not necessarily a cancer - specific test but is commonly used to diagnose prostate cancer.
Most of this protein is eliminated from the body through the semen; however, small measures of this antigen enters the bloodstream and can be found in the blood serum.
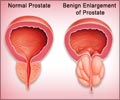
PSA is an established biological marker or a cancer tumor marker because it enables disease–detection, ranging from benign conditions such as prostatitis and prostate gland hypertrophy to cancer of the prostate.
Research is being carried out to improvise the PSA test and make it more reliable and sensitive.
Prostate cancer is the commonest cancer that affects older men. It causes a rise in the level of PSA in the blood. This change in the PSA levels can be detected by a simple blood test, known as the PSA test.
Although PSA is not specific enough to be the final determinant of prostate cancer, elevated levels of PSA are considered serious enough to warrant further investigations.
PSA can either be attached to another compound or may exist by itself:
- Attached PSA: This is a type of PSA which is complexed or attached to the protease inhibitor, alpha –1 antichymotrypsin
- Free PSA: This PSA is free and is not complexed to any molecule
- Total PSA: This is the sum of both the attached and the free form of the PSA
In a standard PSA test, total PSA is usually measured. This is done by taking a blood sample and analyzing the amount of PSA. The amount of PSA in the blood is very low, therefore specific tests, such as the monoclonal antibodies, are employed to carry out the test.
Individuals with prostate cancer tend to have low percent of free PSA compared to those with the benign disease.
Normal concentration of PSA is 0-4 nanogram/ml. This concentration can vary with age. Normally, the prostate gland enlarges in older men and this leads to the increased production of PSA.
Age-specific PSA levels are given below:
- 40 – 49 yrs - 2.5ngms/ml
- 50 – 59 yrs - 3.5 ngms /ml
- 60 – 69 yrs - 4.5ngms /ml
- 70 – 79 yrs - 6.5 ngms /ml
The use of this age-specific PSA range to diagnose cancer remains controversial.
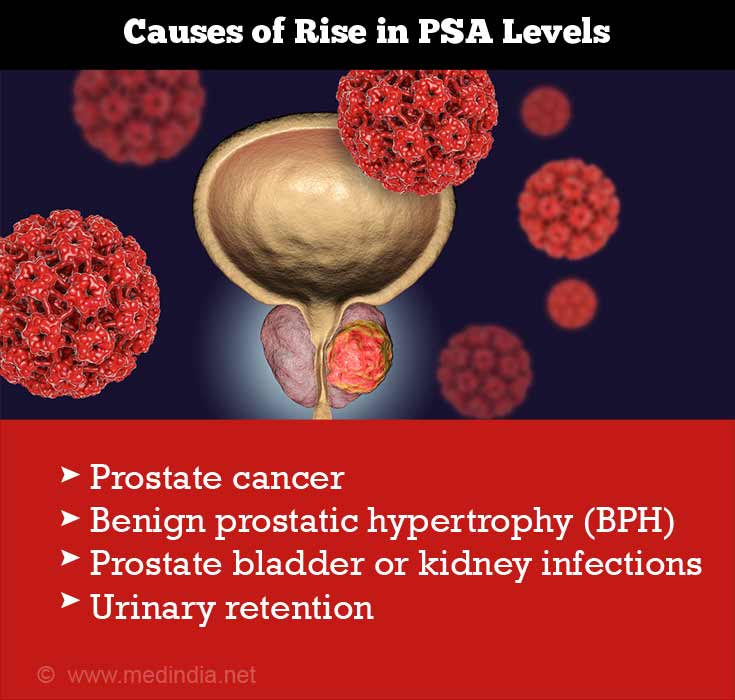
PSA levels not only rise in the case of prostate cancers but also in the case of many conditions of the prostate such as:
- Benign prostatic hypertrophy (BPH)
Prostate bladder or kidney infections- Poor blood supply to the prostate
- Urinary retention
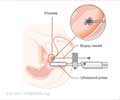
PSA also increases after prostate surgery or after exams or procedures such as biopsies, catheterization or digital rectal exam.
In many cases, PSA is also carried out to check recurrence in a person with prostate cancer. Increased levels of PSA are definitely indicative of recurrence although a single PSA test may not be sufficient to confirm it. Once the levels rise the doctors will ask for further tests to be carried out to confirm the cancer!
It may be interesting to note that the PSA levels increase much before the clinical symptoms of prostate cancer manifest themselves and hence they provide a window of opportunity to cure the cancer before it spreads to other parts of the body. They are also useful in the follow up of the patients who had been treated. Any persistent elevation is considered as recurrence of the cancer.
Sometimes PSA tests reveal small tumors that are not life-threatening. However this will prompt unnecessary treatment initiation. There are also several cases of false positives reported.

![Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis](https://images.medindia.net/patientinfo/1920_500/prostate-specific-antigen.jpg)