- Sasse KC, Warner DL, Ackerman E, Brandt J. Hiatal Hernia Repair with Novel Biological Graft Reinforcement. JSLS. 2016 Apr-Jun;20(2).
- Anti-reflux surgery - (https://medlineplus.gov/hiatalhernia.html)
- Imperatore K, Olivieri B, Vincentelli C. Acute gastric volvulus: a deadly but commonly forgotten complication of hiatal hernia. Autops Case Rep. 2016 Mar 30;6(1):21-6.
- Nissen fundoplication - (https://en.wikipedia.org/wiki/Nissen_fundoplication)
- Bilgin YM, van der Wiel HE. An unusual presentation of a patient with intrathoracic stomach: a case report. Cases Journal. 2009;2:7514.
- Kahrilas PJ, Kim HC, Pandolfino JE. Approaches to the Diagnosis and Grading of Hiatal Hernia. Best practice & research Clinical gastroenterology. 2008;22(4):601-616. doi:10.1016/j.bpg.2007.12.007.
- Hiatal Hernia - (https://medlineplus.gov/ency/article/002925.htm)
- Hiatal hernia - Definition - (http://www.mayoclinic.org/diseases-conditions/hiatal-hernia/basics/definition/con-20030640)
- Digestive Health - Hiatal Hernia - (http://www.memorialhermann.org/digestive/hiatal-hernia/)
- Hiatus hernia - (https://en.wikipedia.org/wiki/Hiatus_hernia)
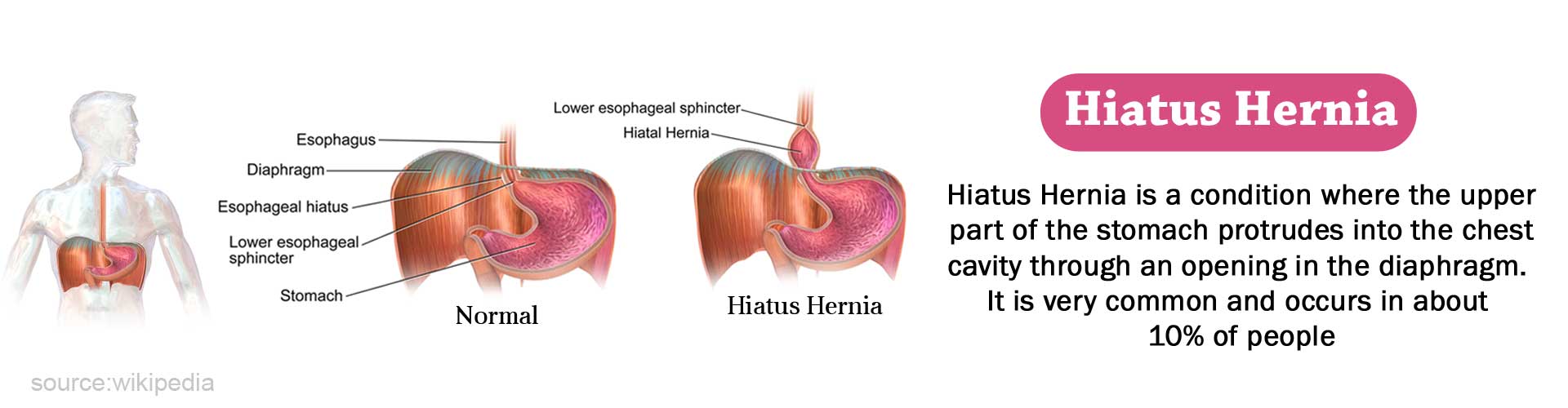
What is Hiatus Hernia?
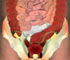
Hiatus hernia or hiatal hernia is a condition where the upper part of the stomach protrudes into the chest cavity through an opening (hiatus) in the diaphragm.
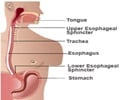
The diaphragm is a sheet of muscle that separates the lungs or the chest cavity from the abdomen. The left diaphragm contains the hiatus in concern here (esophageal hiatus) through which passes the tube-shaped esophagus that carries food and liquid to the stomach. Normally this hiatus is small and fits snugly around the esophagus. The J-shaped stomach sits below the diaphragm.
The diaphragm also prevents the acid from the stomach from getting into the esophagus. When hiatus hernia occurs, and the stomach protrudes upwards, the acid is reflexed up into the esophagus. This can result in a painful burning sensation unlike the other hernias which often appear without symptoms. Hiatus hernia is fairly common and occurs in about 10 per cent of people.
What are the Types of Hiatus Hernias?
Type 1: Also known as sliding hiatal hernia it accounts for 95% of all hiatal hernias. A part of the gastroesophageal junction (the junction containing the part of the esophagus that connects to the upper part of the stomach) herniates into the chest cavity in this type. It is a risk factor for gastroesophageal reflux disease (GERD), a digestive disorder.
Type 2: Also known as para-esophageal or rolling hiatal hernia, it accounts only for 5% of all hiatal hernias but causes the most complications. The gastroesophageal junction remains in its place below the diaphragm while the stomach rotates itself and herniates into the chest cavity next to the esophagus.
If more than 30% of the stomach goes into the chest cavity, it is called a giant para-esophageal hernia.
Type 3: Majority of the para-esophageal hernias belong to this type where the gastroesophageal junction is herniated above the diaphragm and the stomach herniates next the esophagus. Hence, it is a combination of type 1 and type 2.
Type 4: Other organs like the colon, small intestine, pancreas and spleen also herniate into the chest cavity along with the stomach.
The end stage of hiatal herniation involves total herniation of the stomach into the chest by rotating 1800. This is referred to as intrathoracic stomach.
What are the Causes and Risk Factors of Hiatus Hernia?
The cause of hiatus hernia is not known. The result of a weakening of the supporting tissue around the opening can lead to this condition.
Hiatus hernias are very common, especially in people over 50 years old. This can lead to the reflux of gastric acid from the stomach into the esophagus. Children can have this condition from birth.
Obesity and smoking may be the risk factors in adults.

Possible causes for hiatus hernia could be:
- Intense pressure on the abdomen caused by persistent or severe coughing or vomiting, straining while going to the bathroom, pregnancy or by lifting heavy objects.
- Injury to the area.
- Being born with an unusually large opening.
What are the Symptoms of Hiatus Hernia?
Usually, most people are not troubled by their hiatus hernia. But if reflux of the acid contents of the stomach occurs (called gastro-esophageal reflux), heartburn is experienced and it is a painful burning sensation in the chest, which can sometimes be felt in the throat. This can bring the acid fluid into the mouth, especially, when you lie down or bend forward. These symptoms are a problem when you go to bed and can wake you up.
Other symptoms are:
- Belching
- Dull chest pain
- Pain on swallowing hot fluids
- Feeling full after meals due to the “balling up” of food in the lower esophagus before moving on to the stomach
- Shortness of breath
- Heart palpitations
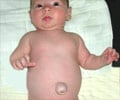
Newborns can have a congenital opening in the diaphragm with symptoms of fast or difficult breathing and increased heart rate.
What are the Complications of Hiatus Hernia?
It is important to distinguish between the symptomatic and complicated hiatal hernia. This is essential because surgery is very often indicated in the latter group.
- Slow bleeding and iron deficiency anemia occur in large hernia.
- Aspiration of hernial fluid can lead to some chest complication.
- Ulceration and stricture of esophagus leading to obstruction
- Rotation of the stomach beyond 1800 causes a rare condition called gastric volvulus.
- Massive hemorrhage
What is the Diagnosis for Hiatus Hernia?
Hiatus hernia is discovered when the patient complains of acid reflux or upper abdominal pain. The diagnosis is confirmed by -
- Radiography - In barium meal X-rays, a chalky liquid is consumed. This coats the upper digestive tract and the esophagus, stomach and the upper part of the small intestine are seen on an X-ray.
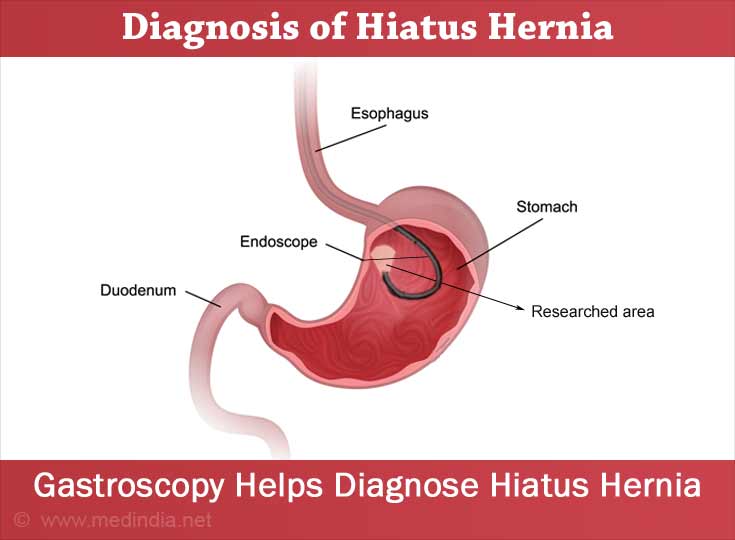
- An endoscopic procedure called gastroscopy - A thin flexible tube is passed down the throat into the esophagus and stomach to check for inflammation.
- High resolution manometry - A catheter sent through the nose down to the gastrointestinal tract measures pressure and movement using sensors. It can detect the exact location and quantify the different elements of the gastroesophageal junction.
- Complete blood tests to check for anemias.
Endoscopy and radiography are relatively insensitive in detecting sliding hiatus hernia.
What is the Treatment for Hiatus Hernia?
If no symptoms like pain or discomfort are present, no treatment is required. When there is pain or discomfort at night due to acid reflux, patients should keep their head raised in bed and avoid lying down immediately after eating. If the cause is being overweight, weight loss is indicated.
Medications that strengthen the lower esophageal sphincter should be avoided. Medicines help to reduce the entry of stomach contents into the esophagus (gastro esophageal reflux). Examples are:
- Proton pump inhibitors that block acid production and heal the esophagus are lansoprazole and omeprazole.
- H2 receptor blockers reduce acid production are cimetidine, famotidine, nizatidine and ranitidine.
- Over-the-counter antacids that neutralize stomach acid.
Surgery:
When the hiatal hernia is huge or when it is of the para-esophageal type, the esophagus gets narrowed or tightened and swallowing becomes difficult. This might cause chronic acid reflux and the cells in the walls of the esophagus could get damaged. Surgery is then advised. In para-esophageal hernia it is the first-line procedure. Any hernia with unrelenting symptoms or complications is an indication for surgical repair. The types of surgery include
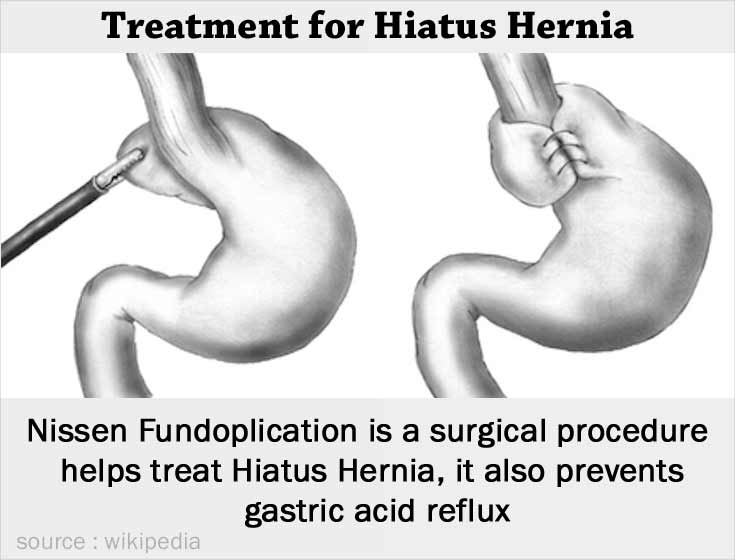
Nissen Fundoplication
The most common surgical procedure is Nissen fundoplication. In this procedure, the upper part of the stomach is wrapped around the lower part of the esophagus and secured with a mesh so the stomach does not herniate upwards. This also reinforces the closing of the lower esophageal sphincter so that gastric acid reflux is prevented.

It can be performed laparoscopically in which case there are lower complication rates, quicker recoveries, and relatively good long term results.
In the open repair surgery, a single large surgical cut is done on the belly and a tube is inserted into the stomach. The tube is removed a week after the surgery.
In the laparoscopic repair surgery, 3 to 5 small cuts are made on the belly through which a tiny tube with a camera at the end and other surgical tubes are inserted. The surgeon does the procedure while looking at the inside of the belly with a video monitor that is connected o the laparoscope.
Endoluminal Fundoplication
In endoluminal fundoplication, no incisions are made. An endoscope with a camera is sent down though the mouth into the esophagus. Small clips are put in place at the gastroesophageal junction to prevent food and stomach acid from refluxing.
Surgery could sometimes be dangerous, so watchful waiting may be advised.
Post-operative complications in surgery could include -
- Recurrence especially high in the case of hiatal hernias
- Difficulty eating within the first month
- Gas bloat syndrome when the stomach fills up with air or food and you are unable to relieve the pressure
- Trouble swallowing
- Ingested foods passing through the stomach very rapidly and entering the small intestine largely undigested (dumping syndrome)
- Excessive scarring
- Smooth muscle fibers failing to relax, which can cause a sphincter to remain closed and fail to open when needed.
- A second surgery might be needed to be done to correct repairs
Using synthetic meshes in this procedure causes infections and erosions. According to a new study, surgeons can perform laparoscopic fundoplication using a new biologically derived material instead of the synthetic mesh reinforcements. They are durable for 3 years post operation.
How do you Prevent Hiatus Hernia?
- Control weight.

- Avoid smoking and drinking alcohol.
- Avoid spicy food and gas producing drinks.
- Have light meals instead of one single heavy meal.
- Don’t bend or lie down immediately after a meal.
- Take an antacid when there is a need.
- Elevate the head of the bed 8 to 10 inches by putting pillows or a wedge under the upper part of the mattress. Gravity then helps keep stomach acid out of the esophagus while sleeping.