- Skin Cancer Foundation - ( http://www.skincancer.org/)
- Skin Cancer - (http://www.nlm.nih.gov/medlineplus/skincancer.html)
What is Skin Cancer?
Skin cancer is a disease where malignant cells are found in the epidermis (outer layer of the skin). One reason why skin cancers can develop is due to exposure to the sun over the years. Ultra Violet radiation from the sun’s rays can cause damage to the DNA and result in gene mutations causing skin cancer. As ozone levels are getting depleted there is less protection from the radiation and this will result in increasing incidence of skin cancers in the world. It is estimated that a 10 per cent decrease in ozone levels will result in an additional 300,000 non-melanoma and 4,500 melanoma skin cancer cases. Hence protective strategies are important against skin cancers and require education of the community.
Skin is the largest organ of the body and protects the body from injury and infection. It also regulates the body temperature and gets rid of waste substances through the sweat glands. Outer layer of the skin is called the epidermis and the layer underneath is known as the dermis. The epidermis contains the squamous cells, which are flat in shape. Below this layer are the basal cells, which appear round. In between these layers are the melanocytes, which produce the pigment, melanin that gives color to the skin.
The body is made up of different types of cells that normally divide and multiply in an orderly manner. These new cells replace the older cells. In case of cancer, certain cells in the body have changed in appearance and function. They divide and grow in an uncontrolled manner to cause an abnormal growth called cancer.
What are the Types of Skin Cancer?
There are three main categories of skin cancer. Each of these three cancers begins in a different type of cell within the skin, and each cancer is named after the cell type in which it begins.
- Actinic/Solar Keratosis
- Basal and Squamous Cell
- Carcinomas/Nonmelanoma skin cancer
- Malignant Melanoma
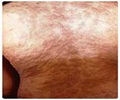
Actinic Keratosis:
Actinic keratosis is otherwise known as a solar keratosis. It is a scaly or crusty bump, which is reddish or pink in color usually seen on the skin surface. It is recognized by touch rather than sight because the crust is horny, dry or rough.
It is the first step in the development of skin cancer and is therefore considered a precancerous skin condition. A keratosis is most likely to appear on the face, ears, bald scalp, neck, backs of hands and forearms, and lips.
The lesions if detected early should be treated or else the lesion grows and invades the surrounding tissues. On rare occasions the lesions metastasize or spread to the internal organs.
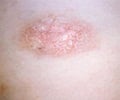
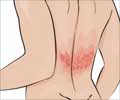
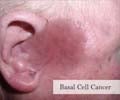
Basal cell carcinoma (BCC) or Rodent Ulcer:
Basal cell carcinoma accounts for about 90% of all skin cancers. If it is detected in the early stage it can be completely cured. If they are left untreated they can erode the skin and cause an ulcer, known as a rodent ulcer. It starts in the basal cell layer of the epidermis and grows very slowly. It is the most common skin cancer found in Caucasians.
A basal cell carcinoma can take several forms. It can appear as a shiny translucent or pearly nodule or a sore that continuously heals and then re-opens, a pink slightly elevated growth or a reddish irritated patch of skin, or a waxy scar. It is mainly seen in the areas exposed to the sun, such as the head, neck, arms, hands, and face. They do not spread to other parts of the body but on rare occasions can spread to the underlying bone.
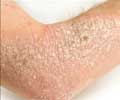
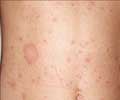
Squamous Cell Carcinoma (SCC):
Squamous cell carcinoma is the second most common skin cancer found in Caucasians, and is more commonly found among the fair-skinned population. It is a cancer of the outermost cells of the skin. The cure rate for squamous cell carcinoma can be 95%, if it is diagnosed early.
It is typically found on the rim of the ear, face, lips and mouth, but it can spread to other parts of the body. Though it is commonly found on sun-exposed areas of the body, it can also be seen inside the mouth and the genitalia.
It is more aggressive than BCC. It usually develops from actinic/solar Keratosis. It is seen as a crusted or scaly area of skin with a red inflamed base that resembles a growing tumor, non-healing ulcer, or crusted patch of skin. Scales can be peeled off, but will eventually reform. SCC requires early treatment to prevent metastasis.
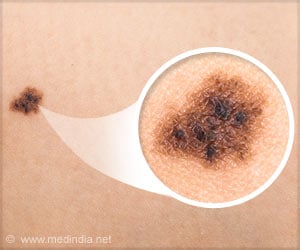
Melanoma:
Melanoma arises from the melanocytes. It is one of the most lethal forms of skin cancer. It accounts for about 4% of all the skin cancers. It has the ability to rapidly spread to the lymphatic system and internal organs especially to the liver, lungs, bones and brain.
Early detection and proper treatment, the cure rate for melanoma is about 95%. Once its spreads, the prognosis is poor. It is the main cause for the majority of skin cancer deaths.
In women, melanomas commonly occur on the arms and legs, while in men they may develop on the back. The malignant melanoma cells still produce melanin and hence the tumors are often shaded brown or black.
Melanoma most often develops in a pre-existing mole or looks like a new mole, which is why it is important for people to know what their moles look like and be able to detect changes in existing moles and spot new moles.
According to recent research, certain moles are at a higher risk for changing into malignant melanoma. Moles that are present at birth, and atypical moles, have a greater chance of becoming malignant. The following ABCDE criteria are crucial in detecting malignant melanoma at its earliest stage.
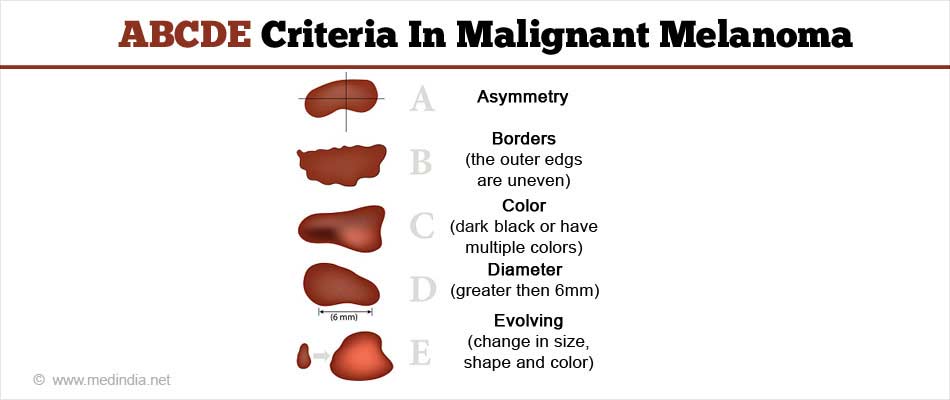
What are ABCDE Criteria in Malignant Melanoma?
Asymmetry: Half of the mole does not match the other half
Border: The border (edges) of the mole are ragged or irregular
Color: The color of the mole varies throughout the mole and maybe unevenly distributed ( can be blue, black, brown or tan )
Diameter: Mole's diameter is larger than a 6 mm.(The size of the pencil eraser)
Evolving: A mole that suddenly changes in it look and the change maybe in its size size, shape or color.
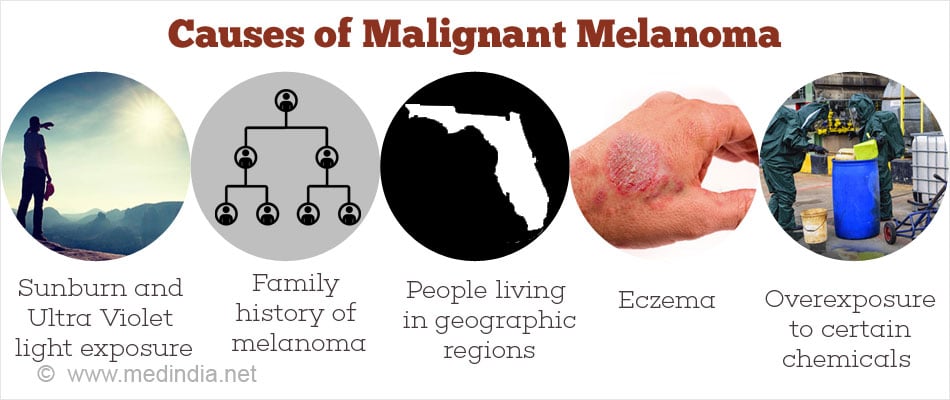
What are the Causes and Risk Factors of Skin Cancer?
- Sunburn and Ultra Violet light exposure cause maximum damage resulting in DNA damage to the skin. The body can usually repair this damage before gene mutations occur. But when a person’s body cannot repair the damaged DNA, then it results in skin cancer. It is likely that most skin damage from ultraviolet radiation occurs before the age of 20.
- In some cases about 5-10% of melanomas develop in people with a family history of melanoma. But inherited faulty genes do not cause non-melanoma skin cancers.
- The regular use of sunlamps and sunbeds increases the risk of developing skin cancer.
- Individuals on long term immunosuppression (to prevent organ rejection) or for treatment of severe arthritis face an increased skin cancer risk.
- People living in geographic regions receiving high-intensity sunlight, such as Florida, Caribbean, or northern Australia are at a greater risk.
- Some of the areas of skin that have been badly burned, or have had long-term inflammation have an increased risk of squamous cell carcinoma.
- Certain skin conditions like eczema, psoriasis, xeroderma pigmentation can also cause skin cancer.
- Radiotherapy given to treat other conditions can sometimes cause skin cancers in the treatment area later in life.
- Other possible but rare predisposing factors are overexposure to certain chemicals at work, including coal tar, soot, pitch, asphalt, creosotes, paraffin waxes, petroleum derivatives, hair dyes, cutting oils and arsenic. Protective clothing should be worn during handling these substances.
- Older people are at higher risk of getting non melanoma skin cancer. But it can develop in younger people too.
- Individuals with light skin that freckles easily and who tend to burn rather than tan.
What are the Symptoms of Skin Cancer?
- A new growth or abnormal accumulation of cells in the skin.
- A change in an existing skin growth.
- A sore that does not heal.
Basal cell carcinoma:
- They are painless smooth pearly or waxy lumps on the sun-exposed surface of the skin.
- The lesions bleed and develop a crust.
- The lesion may become itchy.
Squamous cell carcinoma:
- The lesions are hard with a horny cap but are tender to touch.
- They have a scaly appearance.
Melanoma:
- A change in the size, shape, or color of a mole.
- When there is oozing or bleeding from a mole.
- The lesions are shaded brown or black due to melanin pigment.
How do you Diagnose Skin Cancer?
Skin cancer has to be detected early in life because it is 100% curable if found and treated early.
Self-examination: It is easy to detect skin cancer by skin self-examination. A person has to look for the various symptoms and recognize skin cancer. But in case of doubt the individual has to consult a dermatologist.
Consulting a dermatologist: A specialist in skin diseases is called a dermatologist. When a person has the above-mentioned symptoms, a dermatologist has to be consulted. Based on clinical examination and the history elicited from the patient, the dermatologist comes to the surmise of skin cancer.
Biopsy:
A biopsy is the only certain way of identifying skin cancer, and determining the specific type of cancer. This involves anesthetizing the area of the skin and removing the lesion, or part of it, for microscopic examination.
Skin biopsy is generally a quick and simple procedure; it is usually performed in the office of the dermatologist's in an outpatient setting using a local anesthetic agent.
The type of biopsy performed depends on the type of skin cancer suspected, the position of the tumor, and the tumor's size. Two types of biopsy are done for most skin cancers:
- An excisional biopsy: in case of non melanoma cancer, the entire visible tumor is removed. In the case of malignant melanoma additional removal of a wider margin of normal tissue around the site is also essential
- An incisional biopsy: it is otherwise called as core biopsy. A portion of the lesion is removed and is usually performed on a large lesion. It is the most common type of biopsy
After the sample is removed it is subjected to microscopic examination. With the help of these results the dermatologist divides the skin cancer into two stages:
How do you Treat Skin Cancer?
Up to 90% of all the skin cancers can be treated if they are detected at an early stage. The dermatologist determines the specific treatment for skin cancer based on:
- Age, overall health, and previous medical history
- Stage of the disease
- The immunity status and the tolerance for specific medications, procedures, or therapies
The treatment is tailored to the individual requirement. Treatment can cure most people with basal cell or squamous cell skin cancer. Although the treatment can cause side effects such as scarring in the affected area, this is often minimal or easy to disguise.
If no treatment is offered, the cancer will continue to grow and may spread into deeper tissues of the skin and may need more extensive surgery.
There are several different kinds of treatment available for skin cancer. They are:
1. Surgery:
Surgery is a common treatment for skin cancer.
Excision: Small cancers can be removed by excising them out. It will be done using local anaesthetic agent.
Skin grafts: If the tumor is large or spreading, a larger area of skin may have to be removed and the skin replaced with a skin graft. Skin grafts are layers of skin taken from another part of the body and placed over the area from which the skin cancer has been removed.
Lymphadenectomy: If the squamous cell carcinoma has spread, then some lymph glands have to be removed from the area around the cancer. This is quite a large operation and is done under general anesthesia.
Less Common Surgical Methods include:
Curettage and electrocautery:
The cancer cells are scrapped using a curette (spoon shaped instrument) and an electrically heated loop is applied to cauterise the wound (stop bleeding) and destroy any remaining cancer cells.
Mohs micrographic surgery:
In
2. Cryotherapy:
When the size of the tumor is very small then it can be treated by cryotherapy or cryosurgery. Liquid nitrogen is sprayed on to the cancer to freeze it. After the treatment, blisters may appear which should be covered with a dressing until a scab forms. Then the scab clears off leaving a white scar on the area.
3. Radiotherapy:
High-energy rays are used to treat skin cancer. Radiotherapy affects only a small area of skin causing edema (fluid collection) and erythema (reddening of the skin). After a few weeks the area will dry up and form a crust or scab, which will eventually peel away.
4. Chemotherapy:
It is the use of cytotoxic (anticancer) drugs to destroy cancer cells.
- Topical chemotherapy: It is used to treat early-stage basal or squamous cell cancers. The chemotherapeutic agent is directly applied to the skin cancer as a cream or lotion.
- Systemic chemotherapy: It is used to treat squamous cell carcinoma, which has spread to other parts of the body, chemotherapy is given by injection (intravenously) so that the drugs are carried in the blood and reach the cancer cells.
5. Electro-chemotherapy:
Electro-chemotherapy uses a combination of chemotherapy and electrical pulses to treat cancer.
6. Biological therapy or Biological response modifier (BRM) therapy or Immunotherapy:
Biological therapy helps the body to fight against cancer by using materials like vaccines to bacteria that boost or restore the body's immune system against diseases. In case of treating melanoma it involves injecting Interferons, which boots the immune system and slows down the growth of cancer.
7. Photodynamic therapy (PDT):
It is the new age treatment of skin cancer. It combines the use of laser, or other light sources, with a light-sensitive drug (photosensitizing agent) to destroy cancer cells. A photosensitizing cream will be applied to the skin.
The patient will then need to wait for approximately four to six hours before being treated. Treatment would last for 20-45 minutes. Following treatment, a dressing will be applied to cover the area and protect it from light.
After the treatment the skin heals quickly without scarring. Mild side effects such as pain and sensitivity of the skin can be experienced.
Follow-up:
After the treatment it is always better to go in for regular check-ups to make sure that remission of cancer does not occur. If it does come back additional treatment will be required. Care should be taken because individuals who have developed skin cancer once have a higher risk of developing skin cancer at other skin sites.
What are the Survival Rates for Skin Cancers?
The five-year survival rates for different types of skin cancer are:
- Basal cell carcinoma is more than 99%.
- Squamous cell carcinoma is more than 95%.
- Malignant melanoma is about 88% if it is localized. The survival rates drop to 58% percent when melanoma has spread to nearby lymph nodes, and 13% when it has spread to distant parts of the body.
How do you Prevent Skin Cancer?
Avoid sun overexposure – this is one of the most important preventive measures.
Sun protection creams reduce one's risk of developing skin cancer and also decreases the likelihood of recurrence.
- Use a high-factor sunscreen (SPF 30 or above) whenever exposed to the sun. It should have a broad spectrum offering protection against ultraviolet A (UVA) and ultraviolet B (UVB) rays. Follow the instructions on the bottle and re-apply as recommended, particularly after profuse sweating and swimming
- Wear clothing made of cotton or natural fibers, which are closely woven and offer good protection against the sun
- Stay out of the sun during the hottest part of the day - usually between 10 am and 4 pm
- Avoid tanning beds and sunlamps because they too emit harmful UV rays, which increases the risk for skin cancer
- Vitamin D dietary supplements prescribed by a physican
- Use sunglasses with 99% to 100% UV absorption to provide optimal protection for the eyes. Wear a wide-brimmed hat to protect the face and neck
- Use extra caution near water, snow, and sand as they reflect the damaging rays of the sun

Note: Follow these practices to protect your skin even on cloudy or overcast days. UV rays travel through clouds. Do not use sunscreen on children under 6 months of age.
 MEDINDIA
MEDINDIA
 Email
Email


















I have a scar on my right cheek from a large mole removed when I was three years old. It was itchy and the bumpy red part bled when scratched. Turns out it was Basal Cell Carcinoma.