- What is delirium? - (http://www.icudelirium.org/patients.html)
- Delirium - Overview - (http://icusteps.org/assets/files/booklet/delirium.pdf)
- Brummel NE, Girard TD. Preventing delirium in the intensive care unit. Crit Care Clin. 2013 Jan; 29(1): 51–65. doi: 10.1016/j.ccc.2012.10.007
- Girard TD, Pandharipande PP, and Ely EW. Delirium in the intensive care unit. Crit Care. 2008; 12(Suppl 3): S3. doi: 10.1186/cc6149
- Cavallazi R, Saad M, Marik PE. Delirium in the ICU: an overview. Annals of Intensive Care2012; 2:49 doi: 10.1186/2110-5820-2-49
What is ICU Delirium?
Delirium in general means decreased awareness of one’s own surroundings. If such a condition occurs in the ICU it is termed as ICU delirium.
ICU delirium or psychosis is a condition, or rather, a complication of hospitalization in the intensive care unit. It is characterized by a set of symptoms ranging from mere confusion to agitation. It can also be called as acute brain dysfunction of critically ill patients.
ICU Delirium is classified as hypoactive, hyperactive and mixed types.
- Hypoactive Delirium – The symptoms are of milder variety characterized by confusion, withdrawal, decreased responsiveness and lethargy. This type of delirium is rarely recognized but is much more common than hyperactive delirium. Pure hypoactive type of delirium contributes to about 43.5% of the ICU cases.
- Hyperactive Delirium - As the name suggests, hyperactive delirium is characterized by symptoms like agitation, restlessness and emotional lability. Though this type of delirium can be diagnosed at an early stage, purely hyperactive type of delirium is a rare entity and is seen in about 1.6% of the total cases.
- Mixed Types – Mixed type of delirium has features of both hypoactive and hyperactive delirium and contributes to about 54.1% of cases.
Delirium depends on various factors like age, length of stay in the ICU, if patients is being ventilated or not, severity of disease, having pneumonia, cognitive impairment, depression, or history of previous stroke. It can affect almost one out of four patients admitted to the ICU, but the incidence can be higher depending on the type of patients being admitted.
ICU Delirium has significant impact on the clinical outcome and recovery of the patient. Delirious patients may have three times more risk of mortality than their non-delirious counterparts, and are six times more likely to have complications.
Even after discharge, the amount of time the patient was delirious in the ICU predicts long-term cognitive impairment, physical disability and death even up to a year after discharge from ICU.
What are the Causes / Risk factors of ICU Delirium?
- There are several conditions that increase the risk of developing ICU delirium. These include: Sepsis – Sepsis is an infection of the bloodstream which causes disturbance in the microcirculation, which may precipitate delirium.
- Hypoglycemia or low blood glucose levels - Patients on insulin are more likely to develop low blood sugar. Hence, blood glucose levels should be closely monitored in these patients.
- Hyperglycemia or high blood glucose levels – High blood sugar can also precipitate delirium.
- Sleep deprivation – Sleep deprivation is an important cause of ICU delirium. Most ICU patients are deprived of sleep due to the constant buzzing sounds of the monitors and frequent investigations.
- Sedatives and muscle relaxants – Frequent use of sedatives and muscle relaxants also precipitate delirium. Benzodiazepines, (Midazolam) commonly used for ICU sedation are a common culprit when it comes to precipitating Delirium, and should be avoided for long term infusions hence, sedation vacations are very important to prevent ICU delirium.
- Hypertension – Uncontrolled blood pressure that can happen due to many reasons can precipitate delirium.
- Hypotension or low blood pressure - Several patients in ICU suffer from shock requiring medications to stabilize the blood pressure.
- Fever- Fever due to any reason can cause delirium, especially if the temperature is high and the episodes are frequent.
- Electrolyte imbalance – Electrolyte imbalances like decreased sodium or potassium levels in the blood can cause delirium.
- Unfamiliar surroundings
- Dehydration
- Anemia – Anemia leads to decreased blood and oxygen supply to tissues.
- Respiratory failure – 80% of the delirious patients are those on mechanical ventilation due to respiratory failure.
- Heart failure
Some patients who are more likely to develop delirium than their counterparts in the ICU are-
- Patients with advanced age
- Patients with pre – existing dementia
- Patients who have had a major surgery (surgery of hip or heart) recently
- Patients with depression
- Patients who have poor eye sight or hearing
What are the Signs and Symptoms of ICU Delirium?
ICU delirium manifests with a wide range of symptoms depending on whether the patient presents with hypoactive, hyperactive or mixed delirium:
- Confusion
- Fluctuation in the level of consciousness which maybe highest in the morning and least in the evening
- Disorientation to time, place and person.
- Withdrawal
- Decreased responsiveness
- Emotional lability i.e. changes in feeling or perception
- Inability to sustain attention
- Short-term memory impairment
- Agitation
- Irritability
- Hallucinations
- Illusions
Signs of ICU delirium include:
One of the first signs of ICU delirium is alteration in sleep pattern - inability to sleep at night, and drowsy during the day, and persistent reporting of lack of sleep and the patient asking for sedation. Other signs may include -
- Tachycardia or increase in heart rate
- Hypertension
- Incoherent or irrelevant speech
- Muscle tremors
- Cloth-picking behavior
How do you Diagnose ICU Delirium?
Diagnosis of ICU delirium is purely clinical depending on the signs and symptoms. A few tools are highly helpful in diagnosing ICU delirium and initiating early treatment.
Tools which help in diagnosing ICU delirium include the following:
1. Abbreviated cognitive test for delirium – The total score is obtained by summing up two content scores
- For memory – the score ranges from 0-10
- For attention- the score ranges from 0-14
A total score less than 11 is considered positive for delirium
2. The Intensive Care Delirium Screening Checklist (ICDSC).
Here, the patient is assessed based on the following 8 points:
- Altered level of consciousness
- Inattentiveness
- Disorientation to time, place or person
- Hallucinations- Delusions-Psychosis
- Psychomotor agitation or retardation
- Inappropriate speech or mood
- Sleep disturbances
- Fluctuation in the above symptoms
A score of 4 or above indicates delirium.
3. The Richmond Agitation Assessment Score (RAAS Score). The score ranges from +4 to -5 with 0 being the neutral score where the patient is alert and calm. The +4 score is allotted to the combative patient and a patient who is not arousable is given a -5 score.
4. The Confusion Assessment Method for the ICU (CAM-ICU). This scale is a very important tool to diagnose delirium in ICU patients especially in ventilated patients
Here the patient is assessed for 4 features
- Fluctuation in mental status
- Inattention
- Altered level of consciousness
- Disorganized thinking
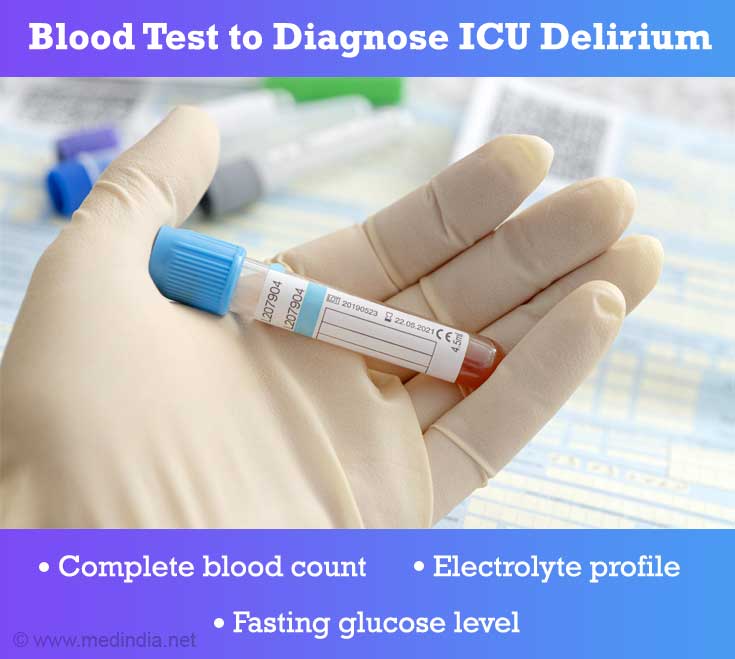
Blood tests-
The following blood tests are done to check for underlying causes of ICU delirium:
- Complete blood count – done to rule out anemia
- Electrolyte profile– done to rule out electrolyte imbalances
- Fasting glucose level – to detect hypoglycemia or hyperglycemia
How Do You Treat ICU Delirium?
ICU delirium is an acute brain failure rather than a mental illness and is reversible in most cases.
Treatment involves supportive treatment and medications.
Supportive treatment – Supportive treatment involves:
Orienting the patient to their surroundings by the following measures:
- Provide visual and hearing aids
- Encourage communication and orient patient repetitively
- Have familiar objects from patient’s home in the room
- Attempt consistency in nursing staff
- Allow television during daytime specially daily news
- Allow light music
Altering the environment
- Maintain sleep hygiene – Keep lights off at night and on at day
- Control excess noise at night
- Ambulate or mobilize patients early
Maintaining certain clinical parameters
- Maintain the systolic blood pressure to more than 90 mmHg of mercury
- Maintain oxygen saturation more than 90%
- Treat underlying metabolic derangements and infections
Medications - Medications usually has a limited role in managing ICU delirium but are definitely helpful in acute psychotic episodes.
Drugs used in ICU delirium are:
- Haloperidol – An antipsychotic
- Risperidone - Newer anti-psychotics like haloperidol and have lesser extrapyramidal effects
- Dexmedetomidine – Dexmedetomidine may be useful to provide sedation without causing delirium
- Melatonin – Melatonin is a naturally-occurring hormone secreted by the pineal gland which regulates the sleep –wake cycle may be useful in the treatment of ICU delirium

How Do You Prevent ICU Delirium?
ICU delirium can be prevented by minimizing or preventing the trigger factors.
- Minimize unnecessary noise or stimuli by keeping a relatively quiet environment
- Cognitively stimulate the patient multiple times a day – The patient has to be spoken to multiple times a day by the health care workers
- The patient should be repeatedly re- oriented to his /her surroundings and the current day and time
- A non-pharmacological sleep protocol should be encouraged- the use of sedatives should be minimized and the need should be re-assessed daily.
- Pain should be assessed on a day-to-day basis and a scheduled pain management protocol should be followed.
- The need of catheters and central lines should be assessed daily and should be removed as early as possible.
- Early mobilization and transfer of the patient to the ward must be considered.