Lung cancer due to commonly-targeted mutations are revealed during progression. Radiation treatment can prevent the tumor spread to the brain.
TOP INSIGHT
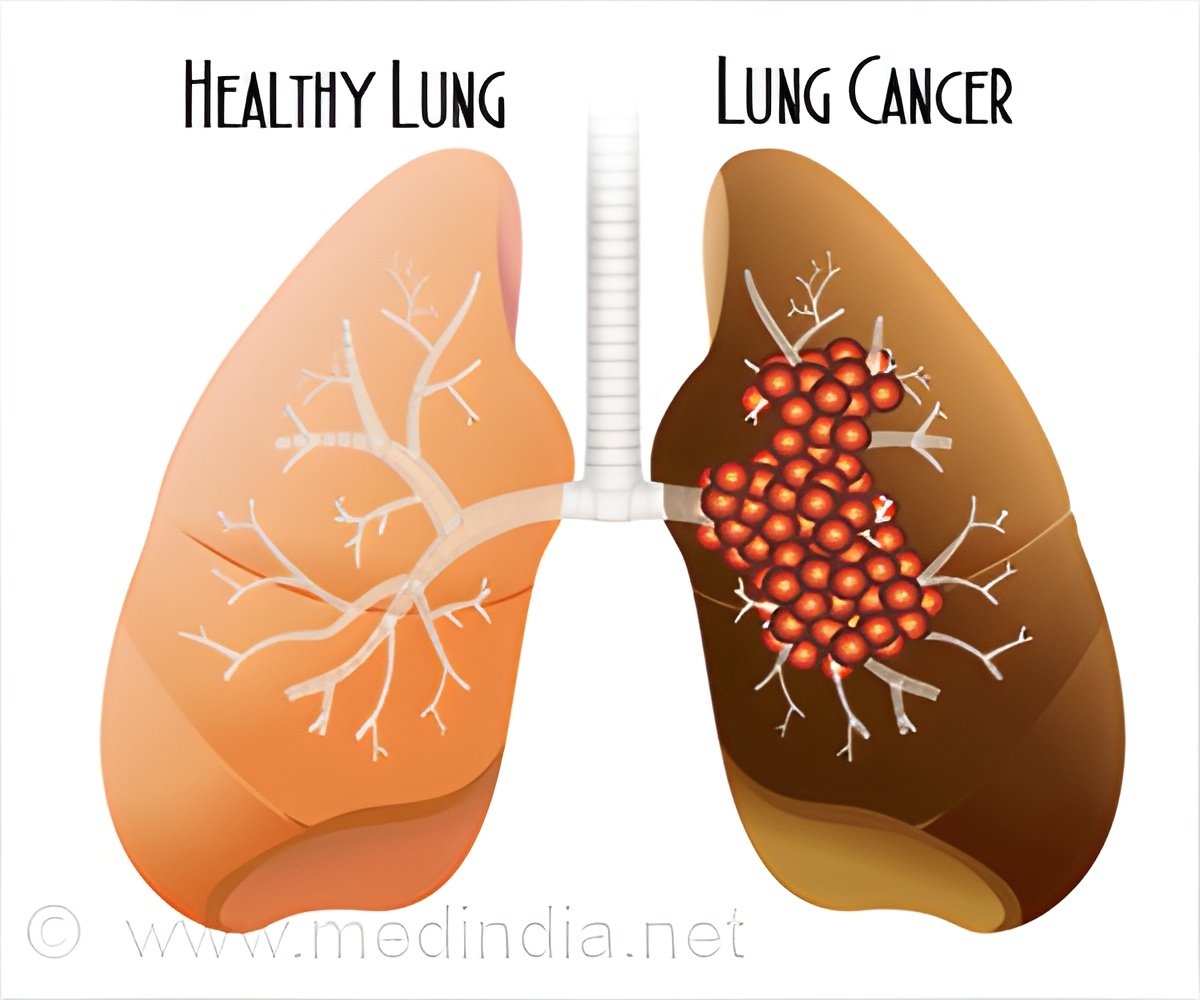
Mutations of non-small cell lung cancer (NSCLC) can reveal the progression at the primary site. Treating the tumor with a preventative course of radiation can often help patients whose tumor spreads to the brain.
The first study (Oral Abstract Session, Presentation #11) deals with SCLC, which is a type of lung cancer with the strongest ties to smoking. It's particularly aggressive, with between 60 and 70 percent of patients diagnosed at advanced stages of the disease. The disease will spread to the brain in more than half of the patients.
Penn researchers looked into a treatment called Prophylactic Cranial Irradiation (PCI), which involves treating the brain with radiation before the cancer has spread there in hopes of preventing the disease's spread and prolonging survival.
"PCI is controversial for patients with extensive stage disease because two past randomized control trials have looked at this question but came to conflicting results," said the study's lead author Sonam Sharma, MD, chief resident of Radiation Oncology.
The group studied 944 propensity score matched patients in the National Cancer Database who had metastatic SCLC but whose disease had not spread to the brain, making this the largest study to ever examine the question of PCI.
The data also shows certain patients were more likely to receive PCI than others. African Americans, patients 75 or older, and those with additional diseases were less likely to receive the treatment.
The second study (Presentation #162) focuses on NSCLC, the most prevalent form of lung cancer. There are multiple known genetic mutations within NSCLC tumors, each of which affects treatment in different ways. The idea is to identify the specific genetic change that has occurred - called drivers - then use an inhibitor drug to precisely target the mutation instead of using general chemotherapy. The most common driver mutation physicians are currently able to target is known as EGFR.
Researchers from Penn focused their study on NSCLC patients with EGFR mutations who had been treated with inhibitors - specifically a tyrosine kinase inhibitor (TKI) like afatinib, gefitinib, or erlotinib-- which target the specific enzyme that is mutated in this subtype of lung cancer. They hoped to learn how the disease in these cases is likely to progress even in the face of drug treatment.
"It's sometimes hard to identify patients when you're being this specific," said David Guttmann, MD, MS, assistant chief resident of Radiation Oncology and one of the study's authors. "Fortunately, using the database available through Penn's Center for Personalized Diagnostics, we were able to identify 74 patients who fit our criteria."
Abigail Berman, MD, MSCE, an assistant professor of Radiation Oncology and the associate director of the Penn Center for Precision Medicine, was the study's lead author.
Of the patients treated with a TKI whose cancers did progress, almost half (46 percent) experienced that progression at the primary tumor site within the lung. Guttmann noted patients who also have metastatic liver disease seemed to have a particularly high rate of progression at their primary site, something he says warrants further investigation. The team's analysis also showed that upfront treatment to their primary tumor was associated with improved progression-free survival. Patients who had received prior treatment to the primary tumor prior to initiating TKI therapy survived an average of 20 and a half months without progression, while patients who had no upfront therapy average 11 months.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email