Radiotherapy is the standard treatment regimen for locally advanced non-small cell lung cancer (NSCLC), but can lead to esophagitis and radiation pneumonitis.
TOP INSIGHT
Elderly non-small cell lung cancer (NSCLC) patients undergoing definitive radiation have a lower incidence of esophagitis compared to younger patients and tolerate aggressive standard treatment regimens.
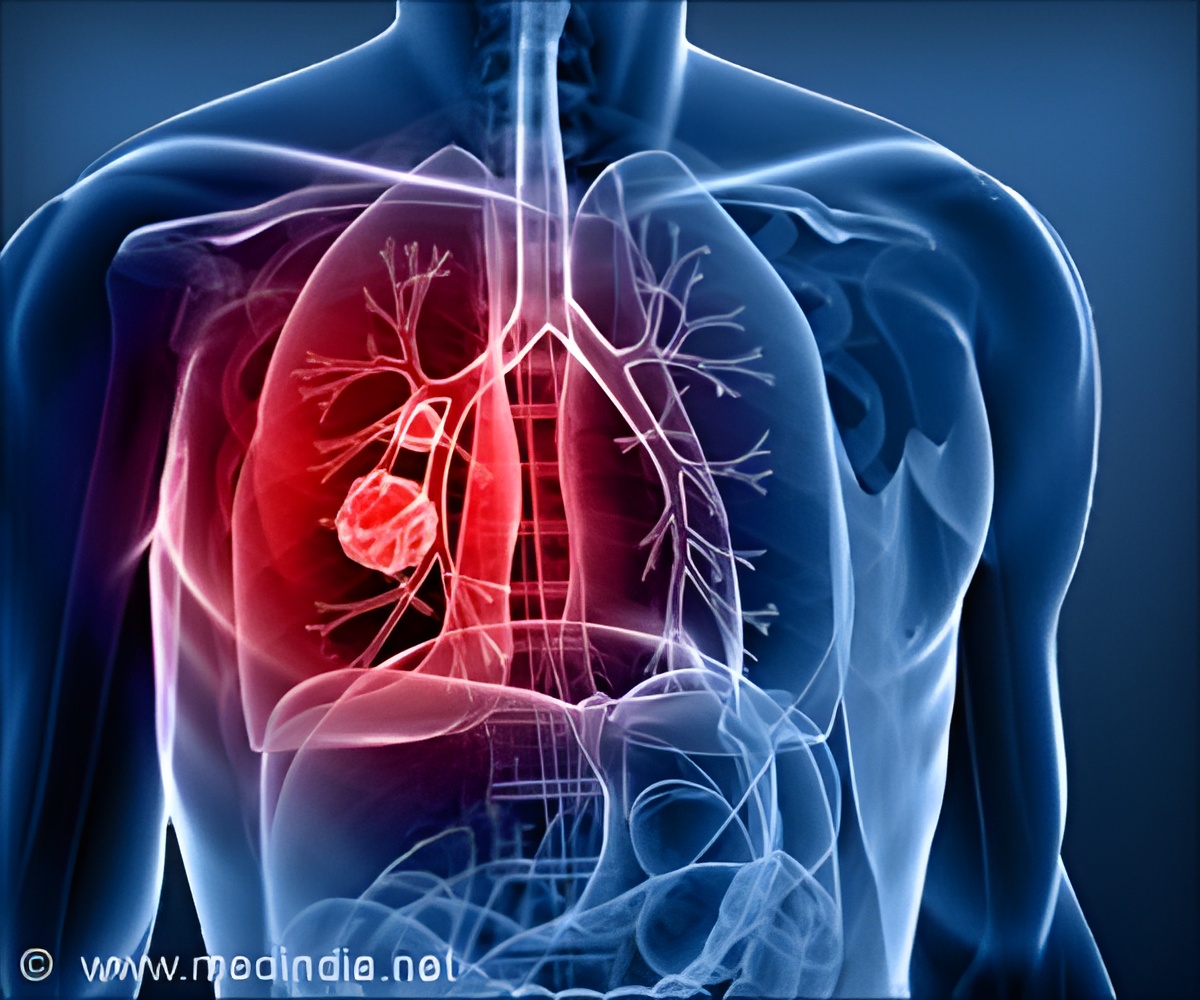
Radiotherapy is the standard treatment regimen for locally advanced NSCLC, but can lead to esophagitis and radiation pneumonitis, which are potentially life-altering toxicities of thoracic radiation.
Elderly non-small cell lung cancer (NSCLC) patients undergoing definitive radiation have a lower incidence of esophagitis compared to younger patients and tolerate aggressive standard treatment regimens.
A group of researchers in the United States conducted a study to evaluate elderly patients undergoing definitive lung radiation to assess how the elderly tolerate treatment compared to younger patients. Patients undergoing definitive radiation for lung cancer with or without chemotherapy from 2004-2013 were identified from a prospective institutional database in which patients of all ages were eligible for inclusion (UM cohort).
Patients were excluded if they were treated with stereotactic body radiation therapy (SBRT) or if complete dosimetric information was not available for review. Logistic regression modeling was performed to assess the impact of age on esophagitis grade ?3 or ?2 and pneumonitis grade ?3 or ?2, adjusting for esophageal and lung dose, chemotherapy utilization, smoking status, and performance status. The analysis was validated in a large cohort of 691 patients from the Michigan Radiation Oncology Quality Consortium (MROQC) registry, an independent state-wide prospective database.
Of the 125 patients, 82 patients were <70 years old and 48% experienced grade ?2 and 16% experienced grade ?3 esophagitis. Conversely, among the 43 patients age ?70, these rates were 23% (grade ?2) and 2% (grade ?3). Multivariate regression modelling of the UM cohort revealed a significant inverse correlation between age and rate of esophagitis for both grade levels. The same association was noted in the MROQC cohort, which validated these results. There was no significant association between age and pneumonitis.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email