Patients must be routinely checked for prostate cancer recurrence after prostate cancer surgery. Statistically, prostate cancer has a higher chance of recurrence.
TOP INSIGHT
Usually, the location of recurring prostate cancer after surgery is often in the prostate fossa, the region where the tumor was before it was removed, but sometimes cancer progresses into the lymph nodes and bones.
Read More..
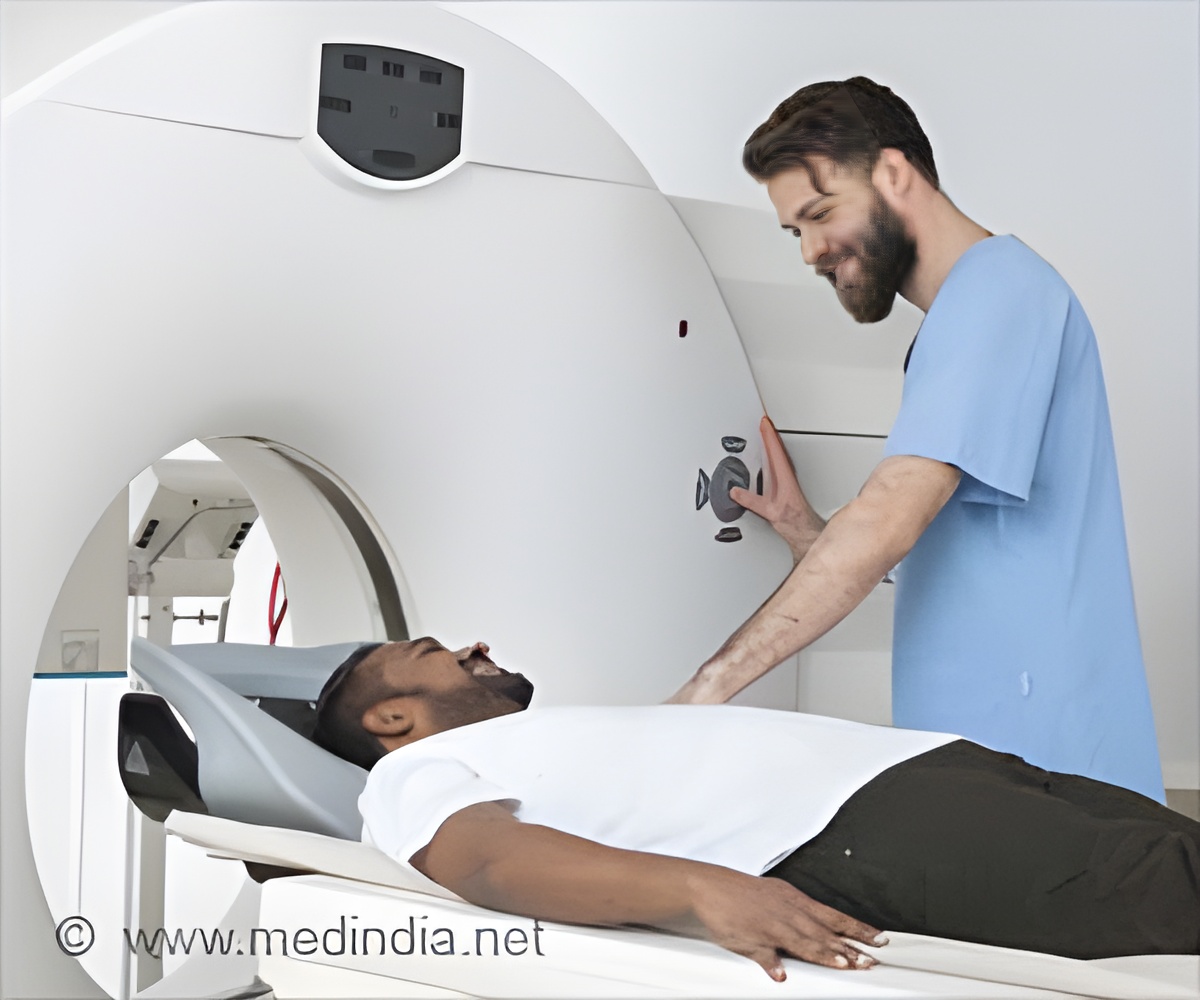
An imaging technique called fluciclovine positron emission tomography, or Axumin PET/CT, is currently the standard of care in the United States for finding the location of the prostate cancer recurrence. However, another new imaging method exists that is called prostate-specific membrane antigen imaging, or PSMA PET/CT, that can also be used for the same purposes. This scan is currently investigational and has not yet been approved by the FDA.
Researchers from the UCLA Jonsson Comprehensive Cancer Center undertook a head-to-head comparison of these two imaging techniques and have concluded that prostate-specific membrane antigen imaging is more effective in detecting the location of the prostate cancer recurrence.
BACKGROUND
As men age, their prostate glands produce increasing levels of prostate-specific antigens. Levels above a certain threshold can be a sign of cancer. For men who have been treated for prostate cancer, a high level of prostate-specific antigens can signal a recurrence of the disease, commonly referred to as biochemical recurrence. In the case of prostate surgical removal, the presence of prostate-specific antigens in the blood means that some prostate cancer cells remain in the body even after prostate removal.
In contrast, the prostate-specific membrane antigen imaging technique tracks the antigens’ protein expression levels. Since prostate cancer cells overexpress a high level of prostate-specific membrane antigens in comparison to normal cells, this imaging method can determine the location of the cancer cells by tracking these cell surface proteins.
To compare the effectiveness of these two imaging methods, UCLA researchers studied 50 patients. All of the men in the clinical trial had previously had a radical prostatectomy where surgeons removed the prostate gland and surrounding tissue due to cancer. They all had a biochemical recurrence of prostate cancer with low prostate-specific antigen levels which indicated that their cancer recurrence was at an early stage.
The men each received a fluciclovine scan as part of their post-surgical recurrence standard-of-care treatment. The men also agreed to receive an additional prostate-specific membrane antigen imaging scan within 15 days before or after their fluciclovine scan.
For the purpose of the study, UCLA researchers removed each individual’s personal information from the scan images. These images were sent to three independent physician readers. The scans were read three times by each reader. The readers were unaware of the findings of the others.
The results showed that the prostate-specific membrane antigen imaging was able to detect the recurrence of prostate cancer in 56 percent of the scans. In comparison, the fluciclovine scan was able to detect prostate cancer in 26 percent of the scans.
IMPACT
Prostate-specific membrane antigen imaging should be the positron emission tomography imaging agent of choice for men who have a prostate cancer recurrence after radical prostatectomy, which needs to be detected and located. For these men, it should become the standard of care, the researchers recommended.
AUTHORS
The team members included: Jeremie Calais, first author; Francesco Ceci; Matthias Eiber; Thomas Hope; Michael Hofman; Christoph Rischpler; Tore Bach-Gansmo; Cristina Nanni; and Bital Savir-Baruch. The complete list of authors may be found in the journal article. JOURNAL
The research was published online in The Lancet Oncology.
Source-Newswise
 MEDINDIA
MEDINDIA

 Email
Email




![Prostate Specific Antigen [PSA] Prostate Specific Antigen [PSA]](https://www.medindia.net/images/common/patientinfo/120_100/prostate-specific-antigen.jpg)