University of Texas Medical Branch researchers have developed a new model to predict early rehospitalization among patients hospitalized for complications of chronic obstructive pulmonary disease.
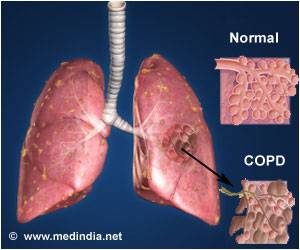
COPD is a major public health concern that affects 12 million to 24 million individuals and is the third leading cause of death in the United States. Each year, thousands of people have acute COPD flare-ups that require hospitalization. About 20 percent of these patients require readmission within 30 days of discharge.
High rates of hospital readmissions and differences in those rates may stem from patient-specific factors, including severity of COPD and the presence of other aggravating health conditions, factors related to health care providers and quality of care, as well as outpatient follow-up and availability of subspecialty referrals. These early readmissions result in overuse of health care resources and impose a heavy financial burden.
Reducing hospital readmissions has been an objective of the Affordable Care Act and Accountable Care Organizations. In 2009, the U.S. Centers for Medicare and Medicaid Services began to publicly report 30-day readmission rates for heart attacks, pneumonia and congestive heart failure as a quality performance measure. In 2012, the CMS started to reduce Medicare payments to hospitals with high readmission rates for patients admitted with these conditions. Beginning in October 2014, COPD will be added to this list.
"This study analyzed a nationwide sample with robust design methods to confirm patient factors as a predictor of early readmission after initial hospitalization for COPD, as well as to show how a combination of different factors can independently contribute to early readmission," stated lead author Dr. Roozbeh Sharif. "Guideline-adherent management and early follow up has the potential to reduce early rehospitalization among COPD patients," added Sharif.
COPD patients with coexisting congestive heart failure, lung cancer, anxiety, depression or osteoporosis were associated with a higher likelihood of early readmission. Health care provider and system factors including prescriptions for bronchodilator inhalers, oral corticosteroids, antibiotics at discharge and an early outpatient follow up after discharge were associated with a lower likelihood of readmission.
Advertisement
The findings of this work have received international attention. It was presented at the World CHEST conference in Madrid, Spain in March 2014 and was quoted at the annual American Thoracic Society conference in May 2014.
Advertisement
Source-Eurekalert