New study findings have significant implications for developing new and potentially more effective therapies to treat oral cancer at an early stage.
‘The protein called lysine-specific demethylase 1 could be a potential target in chemotherapy and immuno-oncology therapies to take down oral cancer.’





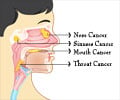
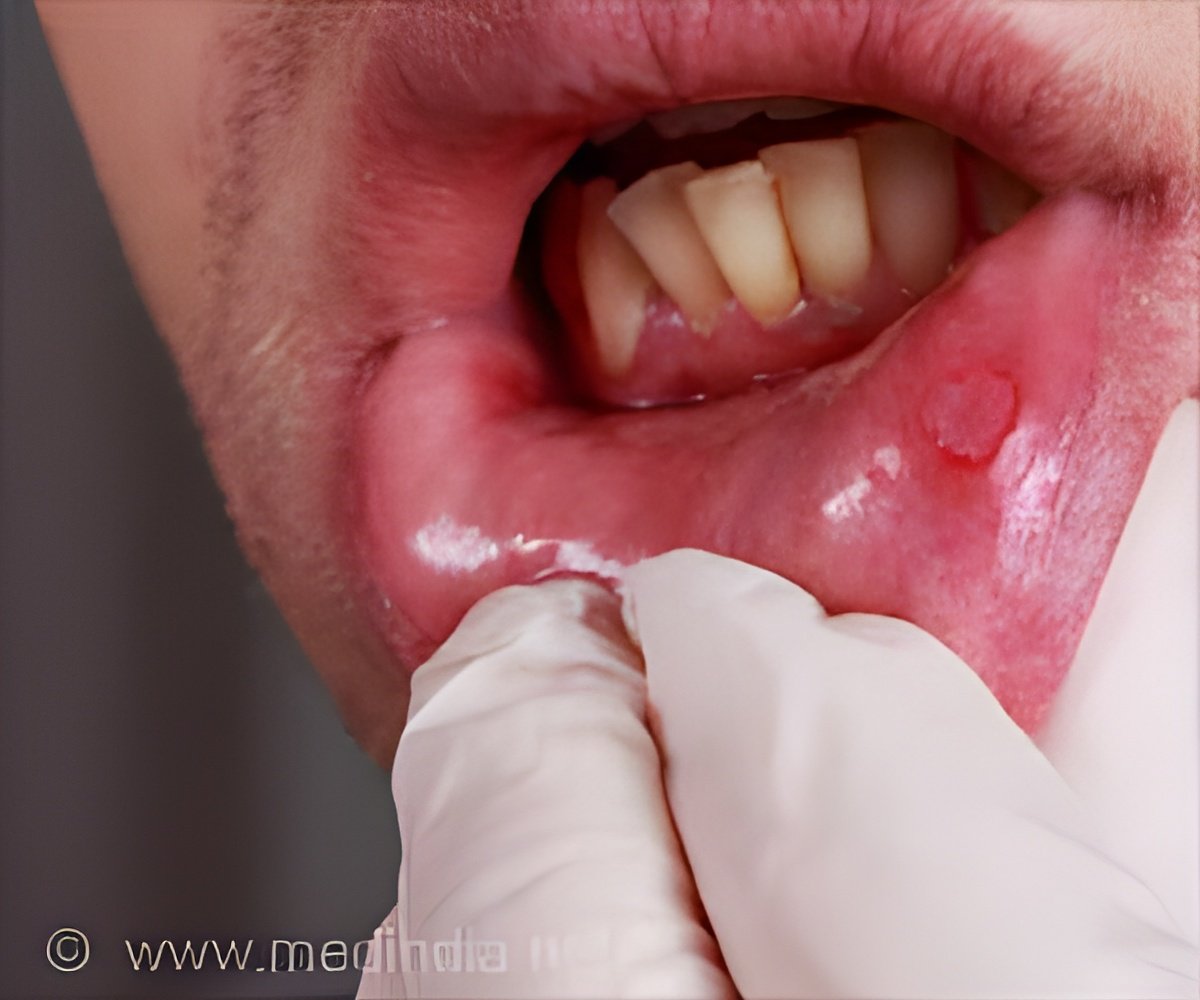
Oral cancer often starts, as many other cancers do, quite innocently. Perhaps as a little white patch in the mouth or a small red bump on the gums. But then something changes, and the little blotch becomes more ominous, starts growing, burrowing into the underlying bone.Patients who are lucky enough to see a dentist before things take a nasty turn to have a shot at being able to prevent the lesions from turning cancerous or can at least make sure treatment starts when it’s most effective.
But for those who aren’t that lucky, the outlook can be bleak: the five-year survival rate of oral cancer is around 66 percent. More than 10,000 Americans die of oral cancer every year; smokers and drinkers are the hardest hit.
Given that at least one-third of Americans don’t visit a dentist regularly, according to the Centers for Disease Control and Prevention, this discovery could be a future lifesaver for those who miss out on preventative care.
Maria Kukuruzinska, SDM’s associate dean for research and a co-author of the study, says “it was rare in the past for dental schools to be diving into the science behind head and neck cancers, with most of the research happening in cancer centers. But that’s changing and dental schools have an advantage over traditional cancer centers when it comes to investigating the science behind the development of OSCC”.
Advertisement
Helping the Body Fight Back - Anti-Tumor Immunity
Once OSCC takes hold, there’s little chance of eliminating it. Clinicians can try chemotherapy and radiotherapy, even cutting out a tumor. There is no cure, only the tumor will shrink but it will not eliminate it.
Advertisement
Later, researchers started to test what would happen to tumors in the tongue if LSD1 was blocked. To restrict the enzyme, the researchers either knocked it out by manipulating genes so LSD1 is effectively switched off or used a type of drug called a small molecule inhibitor, which impedes its normal function.
The aggressiveness, or bad behavior, of the tumor went down and they also found that inhibiting this protein promotes anti-tumor immunity—our body tries to fight by itself.
When regulating LSD1, it messes with a cell communication process that normally helps control organ growth and tissue regeneration. Researchers need to break this cycle.
To find a new way, researchers coupled the effort to inhibit LSD1 by targeting YAP with a different inhibitor, a drug called verteporfin. Originally developed to help treat serious eye conditions like macular degeneration, verteporfin is being tested by other researchers as a potential cancer treatment, including in ovarian cancer.
The combination proved effective, using the LSD1 inhibitor in combination with a common immunotherapy drug that helps white blood cells in the immune system kill cancer cells.
These findings provide a basis for future clinical studies based on the inhibition of LSD1, either as monotherapy or in combination with other agents to treat oral cancer in humans. Although the studies are preclinical, and restricted to mice and some human tissue, researchers want to expand to look at human clinical trial samples.
Source-Medindia