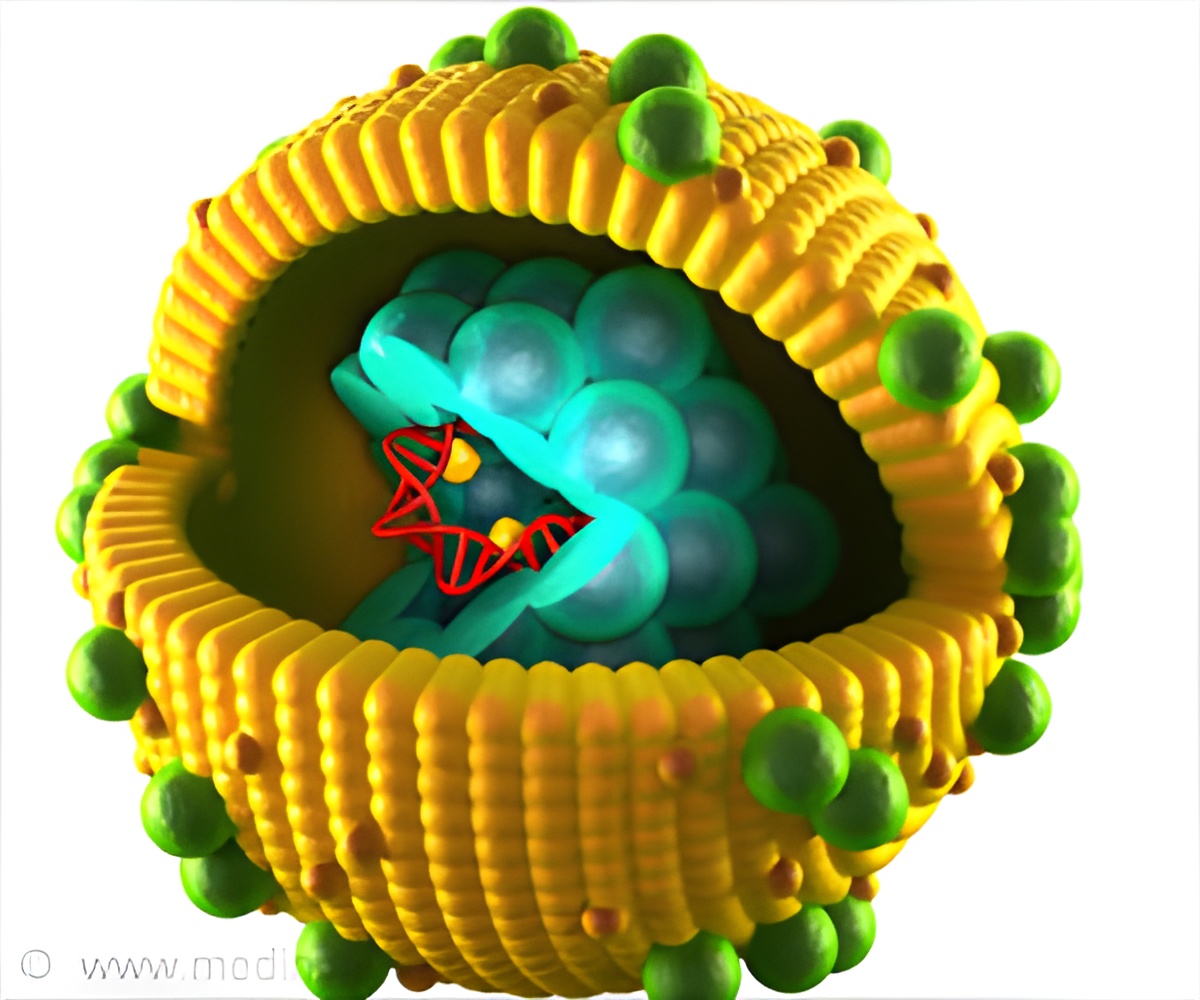
HDV (hepatitis D) virus can only infect individuals at the same time as HBV (co-infection) or superinfect individuals who are already chronic carriers of HBV, reports a new study.
New study has identified the role of a key process in the replication cycle of the hepatitis D virus, an infection that is still very difficult to cure and affects 15 to 20 million people globally. The findings of the study are published in the
Journal of Virology.
The hepatitis D virus (HVD) has a specific target: it infects only people carrying the hepatitis B virus (HBV). As with other co-infections, the combination of hepatitis B and D causes more liver damage than hepatitis B alone.
TOP INSIGHT
Hepatitis D virus is a defective RNA virus that requires hepatitis B virus envelope proteins (HBsAg) to fulfill its lifecycle.
"HDV needs HBV to survive; it's like a parasite," says researcher Patrick Labonté who specializes in liver viruses (hepatitis). However, cure rates are low because treatments for hepatitis B are ineffective against HDV."
"It may seem contradictory since the virus cannot survive on its own," he adds. "In fact, drugs target a specific enzyme to control hepatitis B, but treatment does not completely eliminate the virus. The VHD survives normally and can continue its damage."
The challenge for Professor Labonté and his research team is thus to find a treatment that will fight both viruses, and it seems they are on the right track.
In a study, the team showed that VHD was exploiting the same cellular protein as HBV, called ATG5, to promote its development, particularly its replication in the nucleus of the host cell. This protein is essential for what is called autophagy, a process that is used for cleaning cellular waste. In theory, autophagy should be able to destroy invaders, but most viruses, such as hepatitis C or influenza, have evolved to avoid this degradation and even use autophagy to their advantage.
"Several studies have looked at the role of autophagy in viruses, but it varies from one virus to another depending on its replication process. We are the first to determine the effect of the process on the hepatitis D virus," says Professor Labonté, who is also the study's corresponding author. He was not surprised that ATG5 protein benefits these two hepatitis viruses since they are closely linked.
Towards a Potential Treatment
With this common protein, the autophagic process could be a solution since it is essential to the life cycle of these viruses. However, the situation is not that simple. "If we block autophagy, then we are blocking an important function for all cells in the body. We do not know what the long-term effects might be. Autophagy should be inhibited in a targeted and temporary manner," warns Patrick Labonté;
According to the World Health Organization, at least 5% of people with chronic HBV infection are also infected with HDV. HBV-HDV co-infection is the most severe form of chronic viral hepatitis because it progresses very quickly and can even be fatal. "Hepatitis B virus alone can cause cirrhosis or liver cancer. When combined with the hepatitis D virus, the development of these diseases happens more frequently and more rapidly," he says.
In the course of this research, Professor Labonté;'s team made an interesting discovery: some autophagy proteins travel outside their usual area. "Autophagy usually occurs in the cell's cytoplasm, but the process contributes to the replication of the HDV genome, which takes place in the nucleus. Are there any autophagic proteins present in the nucleus in the case of an infection?" wonders the researcher. This is an area that the team is currently studying and will hopefully provide a more in-depth understanding of the role of autophagy in HDV.
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email