For patients that are diagnosed in the late stages of skin cancer, treatment with a combination of targeted treatments with immunotherapy is ideal.
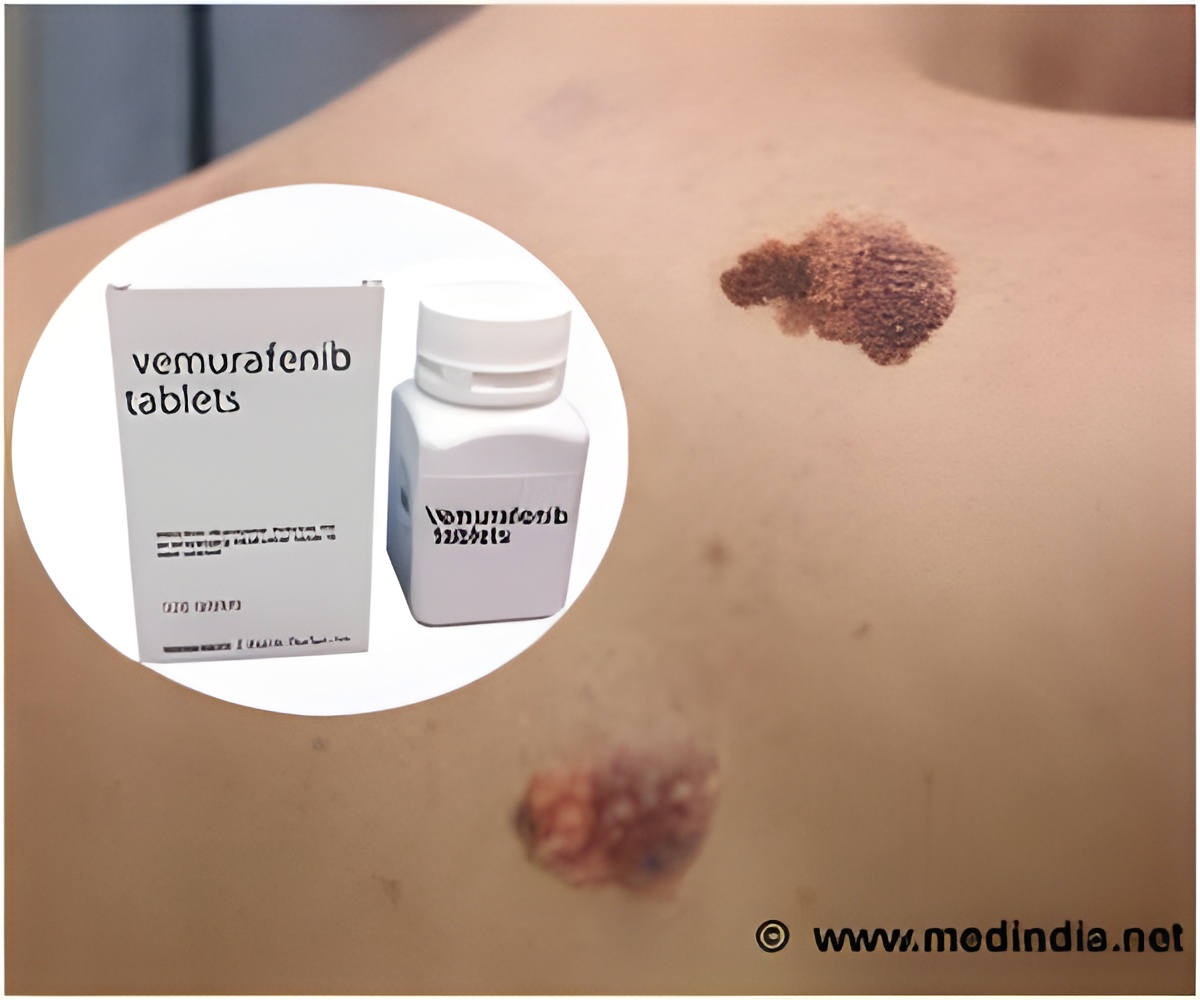
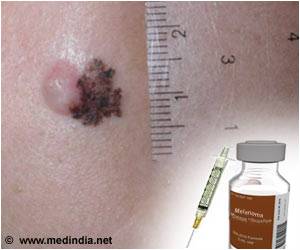
- Melanoma is the deadliest form of skin cancer, most of which have a BRAF mutation.
- The study looked at the most effective treatment for patients diagnosed with advanced BRAF-mutated melanoma but not yet received any treatment.
- Targeted therapy with chemotherapy drugs was effective in improving progression-free survival.
- Immunotherapy was associated with lowest risk of life-threatening events.
In its early stages, melanoma is often cured with surgery alone, however most patients who are diagnosed in the late stages of disease are not candidates for surgery and drug therapy is the main course of treatment.
The study was conducted by researchers from the McMaster University and published in JAMA Oncology.
"This is the first analysis to draw comparison between targeted and immune therapies for BRAF-mutated melanomas," said Feng Xie, principal investigator of the study, who is an associate professor in the Department of Clinical Epidemiology and Biostatistics at McMaster's Michael G. DeGroote School of Medicine.
"Our results will help patients and clinicians choose treatments." Xie added.
A number of effective treatment options are available for patients with advanced BRAF-mutated melanoma, which fall under two classes of drug therapies:
- targeted therapy, like chemotherapy, which stops cancer from growing and spreading
- immunotherapy, which works by stimulating the immune system to attack tumor cells.
The team evaluated 15 randomized controlled trials published between 2011 and 2015, assessing the benefits and harms of targeted or immune checkpoint inhibitors in 6,662 patients with cancer that had spread to the lymph nodes and surgery was not an option, or distant metastatic melanoma.
They found that combined BRAF and MEK targeted therapy and PD-1 immunotherapy were both equally effective in improving overall survival.
Combined BRAF and MEK inhibition was most effective in improving progression-free survival.
PD-1 inhibition was associated with the lowest risk of life-threatening events.
PD-1 is a checkpoint protein on immune cells called T cells.
It normally acts as a type of “off switch” that helps keep the T cells from attacking other cells in the body. It does this when it attaches to PD-L1, a protein on some normal (and cancer) cells.
When PD-1 binds to PD-L1, it basically tells the T cell to leave the other cell alone. Some cancer cells have large amounts of PD-L1, which helps them evade immune attack.
Monoclonal antibodies that target either PD-1 or PD-L1 can boost the immune response against cancer cells and have shown a great deal of promise in treating certain cancers.
"While the data in our study represents best available evidence, using more than one kind of immunotherapy shows promise in early outcomes in clinical trials and could change the treatment landscape once longer-term results are published," said Feng Xie.
They concluded that the safety of PD-1 inhibitors supports using this treatment option as first-line therapy in circumstances where quick action is not a priority.
References
- Immune checkpoint inhibitors to treat cancer - (http://www.cancer.org/treatment/treatmentsandsideeffects/treatmenttypes/immunotherapy/cancer-immunotherapy-immune-checkpoint-inhibitors)
Source-Medindia