Highlights:
- First ever living donor HIV-to-HIV kidney transplant performed by John Hopkins in the US
- Availability of highly effective anti-retroviral therapy options will help long-term HIV control and excellent kidney function
- The donor hopes to inspire many such donations in the future
Read More..
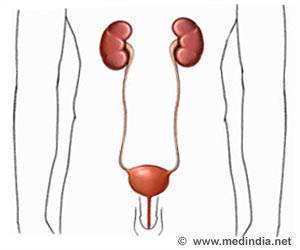
HIV and Kidney Transplantation
Until now people living with HIV have not been able to donate as there were concerns that HIV could be a great risk factor for kidney disease in a donor. However, a research team from John Hopkins led by Dr. Dorry Segev, Professor of Surgery, recently studied over 40,000 people living with HIV. The results of the study show that the new anti-retroviral drugs are safe for the kidney and those with well-controlled HIV would be healthy enough to donate. Furthermore, the risks following donation will be the same for those without HIV and those with it.Commenting on the success of the transplant, Dr. Segev said, “This is the first time someone living with HIV has been allowed to donate a kidney, ever, in the world, and that's huge.”He added, “A disease that was a death sentence in the 1980s has become one so well-controlled that those living with HIV can now save lives with kidney donation--that's incredible.”
Why is this Transplant Significant?
Dr. Christine Durand, Associate Professor of Medicine and Oncology and member of the Johns Hopkins Sidney Kimmel Comprehensive Cancer Center said, “What's meaningful about the first living kidney donor--who is also living with HIV--is that this advances medicine while defeating stigma, too. It challenges providers and the public to see HIV differently.” Speaking about the impact of the transplant, she mentioned, “As patients waiting for a transplant see that we're working with as many donors as possible to save as many lives as possible, we're giving them hope. Every successful transplant shortens the waitlist for all patients, no matter their HIV status.”HOPE in Action
Dr. Durand and Dr. Segev are leading an initiative called HOPE in Action which brings together numerous national studies investigating the feasibility, safety and effectiveness of HIV-to-HIV transplantation. This initiative came into being following Dr. Segev’s work and advocacy for the 2013 federal HIV Organ Policy Equity Act (the HOPE Act).In 2016, Dr. Durand and Dr. Segev had led the team that performed first deceased donor HOPE transplants in the US. Following this, they are now leading two NIH-funded trials of HIV-to-HIV kidney and liver transplants. This first-ever living kidney donor transplant is a major landmark for HOPE.
The Donor’s Experience
“Don't call me a hero, call me the first. I want to see who comes next,” says Nina Martinez, the 35-year-old kidney donor living with HIV. She first came to know about the HOPE Act in 2013 when it was passed. She did not realize that this would affect her personally until she watched the medical drama Grey's Anatomy a few months later. The writers of the TV drama had created a storyline about the first living kidney donor with HIV which allowed Martinez to think about a possibility in her future. “I was also inspired by a friend and neighbor who herself became a living kidney donor,” she added.About being a part of HOPE for Action’s research, she said, “Participating in clinical research is, for me, extremely important. I bore witness to my friend providing a lifesaving transplant, and in watching her I knew that if there was a way for me to help someone else, I had to do it. Doing so under a research protocol was very comfortable for me.”
Life Beyond HIV – Nina’s Journey to Donation
Nina Martinez, a resident of Atlanta, is a public health consultant, clinical research volunteer and policy advocate keen on eliminating the stigma around HIV.“Some people believe that people living with HIV are ‘sick,’ or look unwell,” she says. Martinez also stated, “For me, I knew I was in good health. HIV was no longer a legal barrier to organ donation, and I never considered HIV to be a medical barrier either. As a policy advocate, I want people to change what they believe they know about HIV. I don't want to be anyone's hero. I want to be someone's example, someone's reason to consider donating.”
In July 2018 through Facebook, Martinez found that a friend living with HIV was in need of a kidney transplant. As someone familiar with the medical research process and public health policy, she reached out to John Hopkins as she felt obliged to help her friend.
After discussing the possibility of donating a kidney with Dr. Segev, Martinez traveled to The Johns Hopkins Hospital in Baltimore in October 2018 to undergo a medical evaluation. Multiple trips were made for analysis to ensure that she was healthy enough to donate, a standard procedure followed in all potential living kidney donations.
Unfortunately, before Martinez was declared fit for the surgery, her friend passed away. After the funeral, Martinez contemplated the options available and decided that she was willing to donate to an anonymous recipient, while she was grieving her friend.
About her decision, Martinez remarked, “Despite losing my friend to kidney disease, I wanted to move forward with a donation as a way to honor them. I could do this for someone else, not because I'm special but because I'm strong. Other people living with HIV before me participated in clinical research so that I could not just survive but thrive. It was my turn to do this, for both my friend that I cared about and all people waiting on a transplant.”
Following the medical evaluation, the surgical team found Martinez to be having healthy kidneys and a low viral load, meeting the criteria laid down by the HOPE federal safeguards. After being cleared, Martinez successfully donated a kidney to an anonymous recipient.
HIV-to-HIV Living Donation – The Background
In a study, whose results appeared in a 2018 American Journal of Transplant article, surgeons studied the factors that could help identify candidates healthy enough to donate a kidney. Potential donors should have well-controlled HIV, no history of diabetes, blood pressure under control and normal protein levels in their urine.Both the donor and recipient will be closely monitored by the physicians. With the availability of highly effective antiretroviral therapy options and prediction factors, the HOPE in Action team is positive that long-term HIV control and kidney function will be exceptional.
HIV Organ Donation – Why is it Important Today?
According to the data available from United Network for Organ Sharing, as on March 2019, there are about 113,000 people on the transplant waiting list in the US. The longest waitlist is for kidneys and an average of 20 Americans die due to organ unavailability. In this scenario, people living with HIV, volunteering to donate, could potentially save the lives of thousands of others living with HIV, requiring transplants every year.Following the Johns Hopkins' breakthrough transplant in 2016, under the HOPE Act, there have been more than 50 deceased donors and over 100 transplant recipients, under a HOPE protocol in the US.
References:
- First Ever Living Donor HIV-To-HIV Kidney Transplant- (https://www.hopkinsmedicine.org/news/newsroom/news-releases/first-ever-living-donor-hiv-to-hiv-kidney-transplant)
Source-Medindia