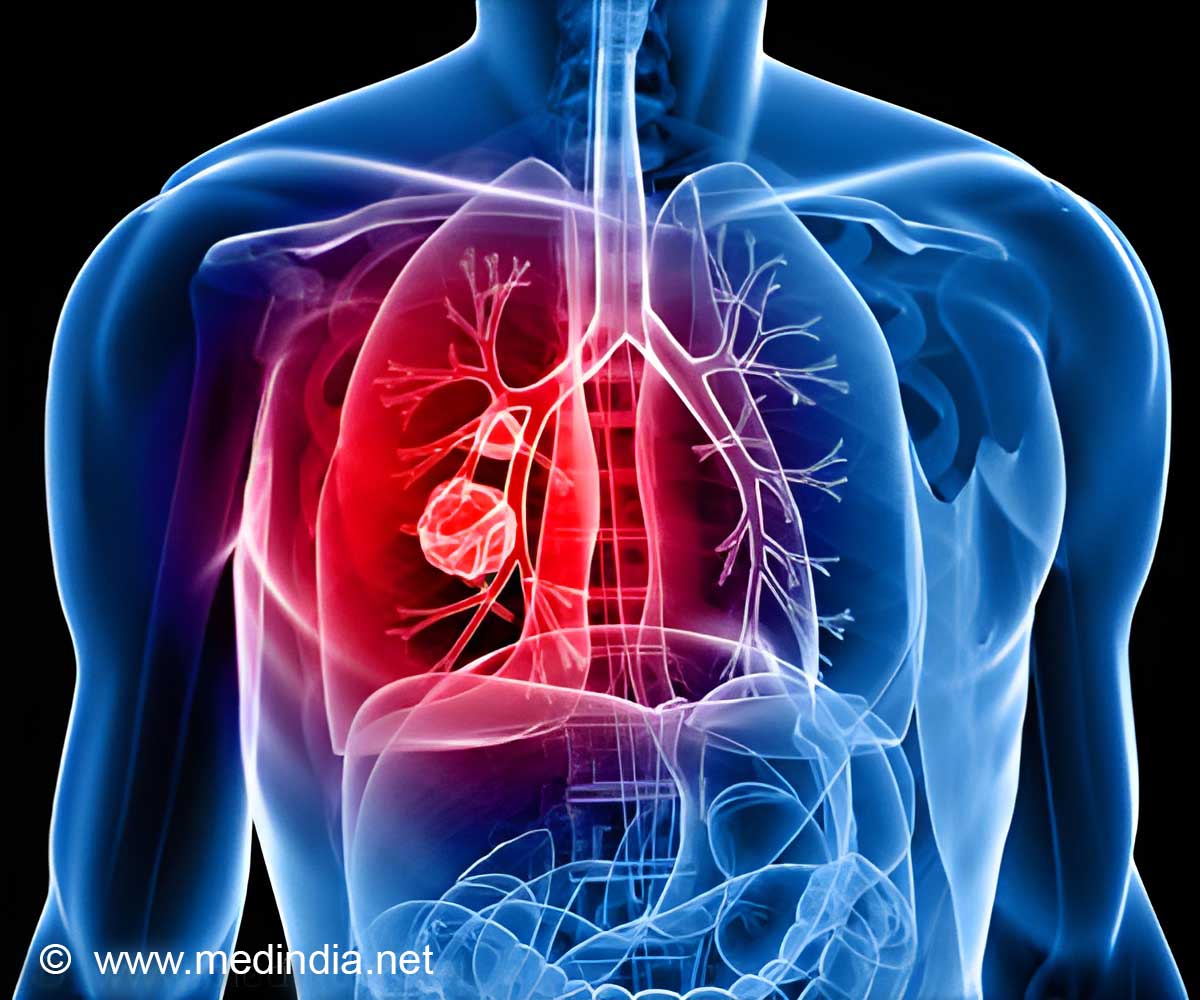
Interstitial lung abnormalities were strongly associated with an increased risk of death, according to a prospective analysis of four separate research cohorts.
TOP INSIGHT
Interstitial lung abnormalities on CT scans signal higher-than-average mortality within 3-9 years.
Lead author Rachel K. Putman, M.D., from the Brigham and Women's Hospital in Boston, and her associates analyzed data from four prospective cohort studies to investigate whether interstitial lung abnormalities are associated with increased mortality.
The study participants were middle-aged to older people from four separate research cohorts as follows:
- 2,633 from the Framingham Heart Study (FHS)
- 5,320 from the Age Gene/Environment Susceptibility (AGES)-Reykjavik Study
- 2,068 from the Chronic Obstructive Pulmonary Disease (COPD) Gene study
- 1,670 from the Evaluation of COPD Longitudinally to Identify Predictive Surrogate Endpoints (ECLIPSE) study
It was seen that interstitial lung abnormalities were found to be present in 177 (7%) of the participants from FHS, 378 (7%) in the AGES-Reykjavik study group, 156 (8%) in COPD Gene group, and in 157 (9%) participants from ECLIPSE study.
The authors reported that the presence of interstitial lung abnormalities were linked to a greater risk of death in all four cohorts over a median follow-up times ranging from 3 to 9 years when compared with those who did not have interstitial lung abnormalities. This was seen after adjustment was made for smoking, chronic obstructive pulmonary disease (COPD), cancer and other co-existing conditions.
Putnam and his associates reported in the journal JAMA that the pattern of abnormalities may be an important risk factor for death in older populations, rather than being merely a precursor to more advanced fibrosis.
They noted that while additional studies were needed to confirm the findings and to determine the risk factors for interstitial lung abnormalities and the events that lead to the death of the patient.
The authors commented, "Although the survival rate of people with idiopathic pulmonary fibrosis (IPF) appears to have increased slightly in recent years, median survival times after diagnosis is 3 to 5 years, which is worse than that of most malignancies. Given the other correlations between IPF and interstitial lung abnormalities, we hypothesized that the presence of interstitial lung abnormalities would be associated with an increased rate of mortality."
The results of the study could have significant implications for clinical practice and research, however requires further investigation.
References:
1. http://jama.jamanetwork.com/article.aspx?articleid=2491637
2. http://www.mayoclinic.org/diseases-conditions/interstitial-lung-disease/basics/definition/con-20024481
3. http://www.chestphysician.org/specialty-focus/pulmonary-medicine/article/interstitial-lung-abnormalities-linked-to-higher-mortality/b7d7236095ae3a3ad5201ce6ff8c1d2a.html
Source-Medindia
 MEDINDIA
MEDINDIA

 Email
Email






