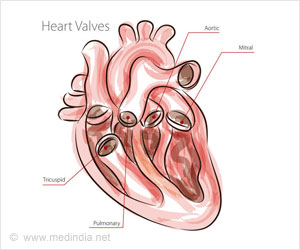
New Bioprosthetic Aortic Scallop Intentional Laceration to prevent Iatrogenic Coronary Artery obstruction (BASILICA) technique makes heart valve procedures safer for high risk patients.
- New Bioprosthetic Aortic Scallop Intentional Laceration to prevent Iatrogenic Coronary Artery obstruction (BASILICA) technique reduces mortality in high risk patients undergoing heart valve replacement.
- According to the American Heart Association, 5 million people in the United States are diagnosed with heart valve disease annually, and more than 20,000 die.
Aim of the BASILICA Technique
The BASILICA procedure was developed by Jaffar M. Khan, M.D., at the National, Heart, Lung, and Blood Institute (NHLBI), part of NIH, to make the TAVR procedure safer in some patients who experience coronary vessel obstruction during this procedure, many of whom die.The BASILICA Procedure
During this procedure, the interventional cardiologist introduces an electrified wire, the size of a sewing thread through the catheter and uses it to cut the original leaflet into two, so that it can no longer block the coronary artery when the new transcatheter aortic valve is positioned in the heart.Findings of the Current Study
- In the current study, the scientists found the BASILICA procedure to be successful in seven critically ill patients who qualified for the procedure on compassionate grounds—until then untested in humans, and no other treatment options available at that stage.
All patients had a successful TAVR with no coronary obstruction, stroke or any major complication," said Dr Robert J Lederman, M.D., the senior investigator in NHLBI's Division of Intramural Research who led the study with Khan. "They were doing well as they reached the 30-day-mark after the procedure."
What is TAVR Procedure?
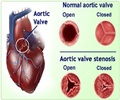
- TAVR, a procedure used to treat aortic valve stenosis involves maneuvering a long, thin, flexible tube through an artery in the leg up into the heart.
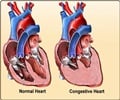
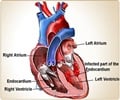
- Aortic valve stenosis refers to severe narrowing of the valve that regulates blood leaving the heart to the rest of the body. Thus this narrowing reduces blood flow to vital organs, leading to chest pain, fatigue, breathlessness, blackouts, and heart failure.
- For elderly or frail patients with aortic valve stenosis, TAVR provides a highly effective and less invasive alternative to open heart surgery.
Why Is TAVR Considered Unsafe In Some Patients?
During TAVR, the cardiologist guides a catheter inside the heart and uses a balloon to replace a new valve inside the damaged aortic valve.However, in some patients having abnormal or unusual physical heart structure, such as very large valve leaflets or small aortic roots (site of origin of the coronary vessel), the large leaflets block blood flow to the coronary arteries (cutting off blood supply to heart) as the new valve's scaffolding releases open.
Says Dr Lederman, "These patients are either not eligible for conventional TAVR, or they are at high risk for it. Additionally, there is no good treatment or prevention strategy for TAVR-induced coronary obstruction. The previous technique of using a stent to open the coronary artery appears to have poor long-term outcomes."
Future Plans
In an early multiple center feasibility study backed by the National Heart, Lung and Blood Institute (NHLBI), which began enrolling patients in January the efficacy of the BASILICA procedure will be reassessed.In conclusion, it is hoped the BASILICA technique will eventually help reduce the number of deaths from heart valve disease or related procedures.
References:
- New technique makes heart valve replacement safer for some high-risk patients - (https://www.nih.gov/news-events/news-releases/new-technique-makes-heart-valve-replacement-safer-some-high-risk-patients)
- Jaffar M. Khan, Danny Dvir, Adam B. Greenbaum, Vasilis C. Babaliaros, Toby Rogers, Gabriel Aldea, Mark Reisman, G. Burkhard Mackensen, Marvin H.K. Eng, Gaetano Paone, Dee Dee Wang, Robert A. Guyton, Chandan M. Devireddy, William H. Schenke, Robert J. Lederman. “Transcatheter Laceration of Aortic Leaflets to Prevent Coronary Obstruction During Transcatheter Aortic Valve Replacement.”, JACC: Cardiovascular Interventions, (2018); 11 (7): 677 DOI: 10.1016/j.jcin.2018.01.247