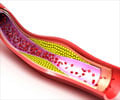
Recent guidelines indicate that a non-fasting cholesterol or lipid profile may be more accurate and convenient than when done in the fasting state.
- A lipid profile is commonly done to measure blood levels of cholesterol, which increases the risk of heart disease.
- Lipid profile test is usually done after overnight fasting.
- Recent guidelines indicate that a lipid profile test in the non-fasting state may be more accurate and convenient than when done in the fasting state.
TOP INSIGHT
A cholesterol test can be done in the non-fasting state, and in fact may be even more accurate than when done in the fasting state.
Recommendations in Denmark suggest that lipid levels should be measured in the non-fasting state rather than in the fasting state. Since people eat several meals a day with snack breaks in between, on an average, more time is spent in a non-fasting than a fasting state. Therefore, non-fasting levels may provide a more accurate picture of the lipid profile. A repeat test in the fasting state may be required in patients with very high triglyceride levels.
Some studies indicate that measurement of non-fasting levels is more indicative of cardiovascular risk as compared to fasting levels. Measurement of cholesterol in the non-fasting state has some practical advantages as well.
The patient can combine the testing with a routine visit to the doctor and does not have to go in separately only for the test. The trouble of going to the laboratory in a fasting state, only to find out that you are not the first and will have to bear the rumbles in your stomach for some more time can be avoided. A diabetes patient is saved from the risk of hypoglycemia or low blood sugar levels.
Thus, non-fasting lipid test may be more convenient for the patient, who is likely to do it more regularly and thereby receive appropriate and adequate treatment. Several other blood tests like hemoglobin A1c also do not require fasting and can be done together.
- Fasting before a lipid test is not routinely required. Several studies indicate that lipid levels do not change much under most circumstances with normal food. However, a high-fat fast food meal may be avoided on the day of the testing to prevent high triglyceride levels.
- A minor decrease in LDL concentration has been noted when the levels were measured 1 to 3 hours following a meal. However, this decrease has also been noted when water is permitted during a fasting state due to dilution of blood. Therefore, the test can be done in the non-fasting state, but the patient should be asked to restrict water intake before the test.
- Measurement of triglycerides may be repeated in fasting state if the non-fasting plasma triglyceride concentration is more than 5 mmol/L (440 mg/dL). A fasting test may be necessary for those recovering from hypertriglyceridemic pancreatitis. Children may also require the test to be repeated in a fasting state to diagnose a lipid disorder that requires treatment.
- Very high levels require immediate referral for treatment.
Fasting may not be required for screening for lipid disorders but may be needed for coming to a specific diagnosis of the cause of abnormal lipids. The reference levels for lipids may differ in a non-fasting and fasting state. Therefore, discuss with your laboratory if you can come in the non-fasting state before going for the lipid profile test.
- B.G. Nordestgaard et al. Fasting is not routinely required for determination of a lipid profile: clinical and laboratory implications including flagging at desirable concentration cut-points-a joint consensus statement from the European Atherosclerosis Society and European Federation of Clinical Chemistry and Laboratory Medicine. European Heart Journal doi:10.1093/eurheartj/ehw152
 MEDINDIA
MEDINDIA


 Email
Email