Ultra-low-power sensors designed to carry genetically engineered bacteria can detect gastric bleeding and other gastrointestinal problems.
- An ingestible sensor can detect bleeding in the stomach and other gastrointestinal diseases.
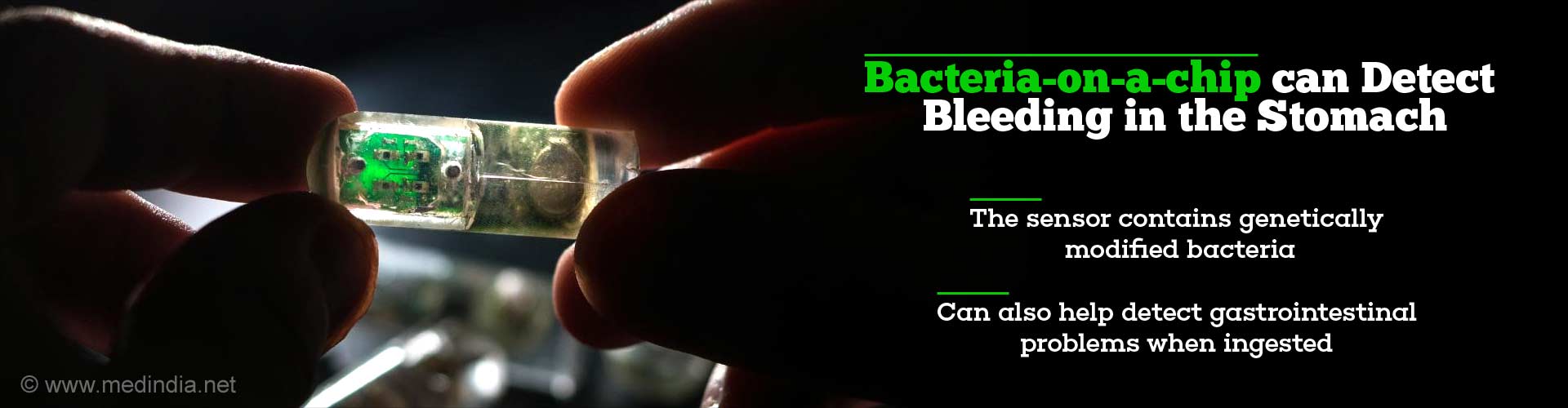
- The sensor contains genetically modified bacteria that can sense environmental conditions and relay information to an electronic circuit.
- The sensor requires very low-power and enables us to detect biological signals in the body and in real-time.
TOP INSIGHT
An ingestible sensor with bacteria programmed to sense environmental conditions and relay the information to an electronic circuit can detect bleeding in the stomach.
Bacteria-on-a-chip
The team used living cells to make the ingestible sensor. It uses ultra-low-power electronics that convert the bacterial response into a wireless signal that can be read by a smartphone. "By combining engineered biological sensors together with low-power wireless electronics, we can detect biological signals in the body and in near real-time, enabling new diagnostic capabilities for human health applications," says Timothy Lu, an MIT associate professor of electrical engineering and computer science and of biological engineering.Study Overview
We have come a long way using bacteria to respond to stimuli such as environmental pollutants or markers of disease. The bacteria are engineered to produce outputs such as light when they detect the target stimulus. However, specialized equipment is usually required to measure this response.The team at MIT wanted to create a sensor that could translate the bacterial response into a wireless signal.
The cylindrical, 1.5 inch sensor was created to respond to heme, a component of blood and requires about 13 microwatts of power. The team has also designed sensors that can respond to a molecule that is a marker of inflammation.
The initial demonstration was focused on detecting bleeding in the GI tract. A probiotic strain of E. coli was engineered to express a genetic circuit that causes the bacteria to emit light when they encounter heme.
The bacteria were placed into four wells on their custom-designed sensor and covered by a semipermeable membrane. The membrane allows small molecules from the surrounding environment to diffuse through. A phototransistor under each cell measures the amount of light produced by the bacteria and relays the information to a microprocessor that sends a wireless signal to a nearby computer or smartphone. An Android app was also developed to analyze the data.
Testing the Sensor
The ingestible sensor was tested in pigs and the team showed that it could correctly determine bleeding in the stomach.Patients suspected to be bleeding from a gastric ulcer currently have to undergo an endoscopy to diagnose the problem, which often requires sedation.
"The goal with this sensor is that you would be able to circumvent an unnecessary procedure by just ingesting the capsule, and within a relatively short period of time you would know whether or not there was a bleeding event," says Mark Mimee, coauthor of the study.
Future Prospects
The team is working to reduce the size of the ingestible sensor and increasing the time that bacteria can survive in the GI.The team has also developed other sensors; one which detects a sulfur-containing ion called thiosulfate, linked to inflammation. This could be used to monitor patients with Crohn's disease or other inflammatory conditions. The second sensor detects a bacterial signaling molecule called AHL, which can serve as a marker for gastrointestinal infections.
References:
- Ingestible "bacteria on a chip" could help diagnose disease - (http://news.mit.edu/2018/ingestible-bacteria-on-a-chip-help-diagnose-disease-0524)
- An ingestible bacterial-electronic system to monitor gastrointestinal health - (http://science.sciencemag.org/content/360/6391/915)
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email




