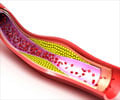
New artificial intelligence (AI) based technology can accurately identify patients with familial hypercholesterolemia (FH), a rare genetic disease that causes elevated blood cholesterol levels.
- New AI-based technology can detect patients with familial hypercholesterolemia – a genetic disease that causes high blood cholesterol
- The technology can accurately differentiate between different categories of patients with high cholesterol
- It prevents unnecessary genetic testing of all patients, thereby saving both time and money
To tackle the problem of misdiagnosis of FH, the researchers came up with a novel AI-based technology that is capable of detecting a larger number of FH patients than conventional methods.
The study, published in npj Digital Medicine, a Nature Partner Journal (NPJ), was jointly led by Dr. Joshua W. Knowles, MD, PhD and Dr. Nigam H. Shah, MBBS, PhD.
Dr. Knowles is an Assistant Professor of Medicine (Cardiovascular Medicine) at the Stanford University Medical Center, California, USA. He also holds joint appointments at Bio-X, the Cardiovascular Institute, and the Maternal & Child Health Research Institute.
Dr. Shah is an Associate Professor of Medicine (Biomedical Informatics) and Biomedical Data Science at Stanford University, California, USA. He is also the Assistant Director of the Center for Biomedical Informatics Research at Stanford. He also holds joint appointments at Bio-X, the Stanford Cancer Institute, and the Wu Tsai Neurosciences Institute.
The lead author of the study was Dr. Juan Banda, PhD, who is currently an Assistant Professor of Computer Science at Georgia State University and a former Research Scientist at Stanford.
This project is part of a large initiative called Flag, Identify, Network, Deliver FH or FIND FH. This is a collaborative effort between Stanford Medicine and the Familial Hypercholesterolemia Foundation, which is a non-profit organization that focuses on AI, Machine Learning, and Big Data to engage FH patients and their families.
TOP INSIGHT
New AI-based technology can accurately diagnose patients with familial hypercholesterolemia (FH), a rare genetic disease that causes elevated blood cholesterol levels.
Read More..
Familial Hypercholesterolemia and Risk of Heart Disease
The genetic disorder FH occurs due to a defect on chromosome 19. The defect prevents the body from clearing low-density lipoprotein (LDL), the so-called ‘bad’ cholesterol that clogs the arteries. It is believed that less than 10 percent of individuals actually realize that they have FH. An FH patient with high cholesterol is three-times more likely to develop heart disease at an earlier age than a patient having high cholesterol, but not FH. Moreover, an FH patient has a 10 times higher risk of developing heart disease compared to a normal individual.Diagnosis of Familial Hypercholesterolemia: Drawbacks of Genetic Testing
Conventionally, FH is diagnosed by genetic testing to confirm whether a patient has inherited the FH mutation on chromosome 19. However, it is neither practicable, nor financially possible to test everyone for the FH mutation. In this regard, Shah said: “The problem is, the chance that someone seen in the Cardiology Clinic has this genetic condition is somewhere around 1 in 90 or 1 in 100, so it doesn’t make sense to sequence every single person.”New AI Technology: A Game Changer
The new AI technology is a paradigm shift in the diagnosis of FH. The novelty of the new AI technology lies in its functionality. The technology works like a sieve, i.e. it filters all the medical data for each and every patient and captures only those patients who are likely to have the condition.“Theoretically, when someone comes into the clinic with high cholesterol or heart disease, we would run this algorithm,” Shah said. “If they’re flagged, it means there’s an 85 percent chance that they have FH. Those few individuals could then get sequenced to confirm the diagnosis and could start an LDL-lowering treatment right away.”
How Was the AI Technology Developed?
The algorithm was developed based on patient data accessed from the electronic health database of Stanford’s FH Clinic. The algorithm was trained to identify features that distinguish an FH patient from other patients. The health parameters that the algorithm analyzed included the following:- Family history
- Current prescriptions
- Lab test reports
- Lipid profile
The outcome of this real patient data based training was that the algorithm was able to rank the patients according to their likelihood of having FH. A patient having a higher rank would be more likely to have the disease, compared to those having a lower rank.
Next Step: Taking the AI Technology to the Clinic
The clinical applicability of the new AI technology was rigorously tested in a real clinical setting. The algorithm was run on approximately 70,000 blinded medical records, which it had never encountered before. From the medical records flagged by the algorithm as being those of FH patients, the researchers sampled 100 records and found that the algorithm was 85 percent accurate in its prediction. Then the researchers, in collaboration with Geisinger Healthcare System, tested the algorithm on 466 FH patients and 5,000 patients without FH.“The predictions came back with 85 percent accuracy, and we knew that many of the Geisinger patients had a confirmed FH diagnosis with genetic sequencing,” Shah said. “So that’s how we convinced ourselves that yes, this indeed works.”
Conclusion
This new AI technology could fill the gap in the area of FH diagnostics, particularly when used in conjunction with family screening programs, which are regularly conducted by the FH Foundation.This work is an excellent example of Stanford Medicine’s commitment towards developing precision health for accurately diagnosing and preventing disease in healthy individuals, while treating those who are afflicted by the disease.
Reference:
- AI identifies risk of cholesterol-raising genetic disease - (http://med.stanford.edu/news/all-news/2019/04/ai-identifies-risk-of-cholesterol-raising-genetic-disease.html)
Source-Medindia
 MEDINDIA
MEDINDIA




 Email
Email