Pneumonia is the single largest cause of death in children worldwide. Preventing pneumonia in children is an essential component of a strategy to reduce child mortality

Diagnosing childhood pneumonia accurately is also a challenge if compared to other disease interventions. Dr Stephen Graham informed that blood culture sensitivity for pneumonia ranges between 10-20% and lung aspirates give a much higher yield of up to 50%. Sensitivity using molecular diagnostic techniques is high from polymerase chain reaction (PCR) of lung aspirate but such services are limited to very few settings in high burden countries for childhood pneumonia.
Studies have indicated that good programmatic management of childhood pneumonia has resulted in positive public health outcomes such as reduced mortality and significantly fewer hospitalizations of children. For example a study revealed that due to good interventions to respond to childhood pneumonia, 47,000 fewer hospitalizations took place in a given setting. Similarly in Gambia good interventions to control childhood pneumonia also led to an impact on child survival, said Dr Graham.
PNEUMOCOCCAL CONJUGATE VACCINE (PCV)
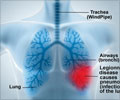
Dr Graham said that the pneumococcal conjugate vaccine (PCV) helps protect against mild and severe infections due to the bacteria Streptococcus pneumoniae. This bacteria frequently causes ear infections, meningitis, and pneumonia in children. By 2015, many high burden countries for childhood pneumonia are likely to have a programmatic roll-out of this vaccine. Ghana rolled out this vaccine last year.
Dr Graham said to Citizen News Service (CNS) that PCV has had tremendous reduction effect (25% - 45%) on all-cause pneumonia hospitalization in developed countries. Further evaluation is required in developing countries to assess impact of this vaccine on pneumonia, said Dr Graham.
Dr Mohammod Jobayer Chisti, Scientist (Centre for Nutrition and Food Security) and consultant physician, Respiratory Ward, Dhaka Hospital, ICDDR, Bangladesh said that 18% of childhood deaths are attributed to pneumonia (14% in children below 5 years of age, and 4% in neonates). Every 7 seconds a child dies of pneumonia. Dr Chisti studied the incidence of tuberculosis (TB) in children with pneumonia who also had severe acute malnutrition (SAM). Children were tested in a study in Bangladesh where blood culture was done and sputum samples (one sample each by gastric lavage and induced sputum) was sent for TB smear microscopy, culture testing and Gene Xpert MTB/ RIF. 6.8% of children were positive for TB (laboratory based confirmatory diagnosis for TB) but 16% were clinically presumptive of TB. Among these children with TB, only 19% had household TB contact. Children with TB does not necessarily present with chronic cough, said Dr Chisti.
Advertisement
Effective, integrated case management strategies ensure that children receive proper and timely treatment for pneumonia. Improving access to services and increasing awareness and demand for services within communities is crucial to controlling pneumonia.
Advertisement
Dr Enarson shared her years of experience in Malawi. When Malawi government had invited her and The Union to help respond to childhood pneumonia in 2000, then it was the third poorest country in the world. Life expectancy at birth for males was 35.7 years and for females was 36.9 years. Case fatality rates were more than 20% for severe pneumonia due to inadequate skills, poor environment, inadequate drugs, poor data collection, collation and analysis, among other factors.
Dr Enarson helped develop an information system to record and report outcomes (impact) of the interventions in Malawi. 47,228 admissions for childhood pneumonia took place in Malawi by 2005. Death rates came down and treatment outcomes significantly improved in severe pneumonia cases but for very severe pneumonia, the challenge remained.
According to the World Health Organization (WHO), pneumonia is the leading cause of death in children worldwide. Pneumonia can be caused by viruses, bacteria or fungi. Pneumonia can be prevented by immunization, adequate nutrition and by addressing environmental factors. Pneumonia caused by bacteria can be treated with antibiotics, but around 30% of children with pneumonia receive the antibiotics they need.
Preventing pneumonia in children is an essential component of a strategy to reduce child mortality. Immunization against Hib, pneumococcus, measles and whooping cough (pertussis) is the most effective way to prevent pneumonia. Adequate nutrition is a key to improving children's natural defences, starting with exclusive breastfeeding for the first six months of life. In addition to being effective in preventing pneumonia, it also helps to reduce the length of the illness if a child does become ill. Addressing environmental factors such as indoor air pollution (by providing affordable clean indoor stoves or ensuring tobacco-smoke-free indoor air environments) and encouraging good hygiene in crowded homes also reduces the number of children who fall ill with pneumonia.
Source: Bobby Ramakant, Citizen News Service – CNS