- Cecil Medicine, 23rd Ed.
- Harrison's PRINCIPLES OF INTERNAL MEDICINE, 17th Edition
About
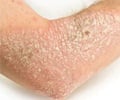
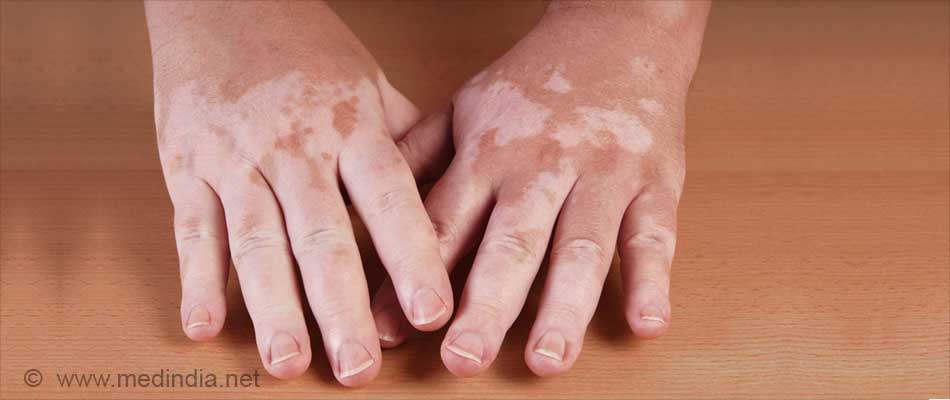
Vitiligo is a skin disease characterized by patches of unpigmented skin. The skin loses melanin, the pigment that determines the color of your skin, hair and eyes. Vitiligo is usually slowly progressive. Principal areas affected includes periorificial areas (around the eyes, nose, lips, genitalia) and the hands, feet, flexor surface of the wrists, ankles, elbows, knees, and major body folds. Vitiligo affects all races. It is more noticeable and disfiguring in people with darker skin. About 0.5 to 1 percent of the world's population have Vitiligo.
Causes
In Vitiligo, melanin is either destroyed or not produced. The exact cause of Vitiligo is not known yet. A number of theories exist. The most widely accepted view is that Vitiligo is an autoimmune disease, i.e. one in which the person’s immune system attacks the organs and tissues of the body. Heredity may be a factor since Vitiligo runs in certain families. However, only 5 to 7 percent of children will get Vitiligo even if a parent has it.
Sometimes, a single event, such as sunburn or emotional distress, can trigger the condition.
The main sign of Vitiligo is pigment loss. Vitiligo causes milky-white patches (depigmentation) on skin. The diagnosis of Vitiligo is made based on a physical examination, medical history, and laboratory tests. Medical treatment for Vitiligo is not always necessary. Treatment includes topical corticosteroids, topical immunomodulators (e.g., tacrolimus), phototherapy etc. Surgical modalities are also available.