What is Iridectomy?
Iridectomy, is a procedure to remove a part of the iris, which is the colored circular membrane behind the cornea of the eye. Earlier this was performed surgically (surgical iridectomy). However, now the procedure is in most cases performed with a laser (laser iridotomy).
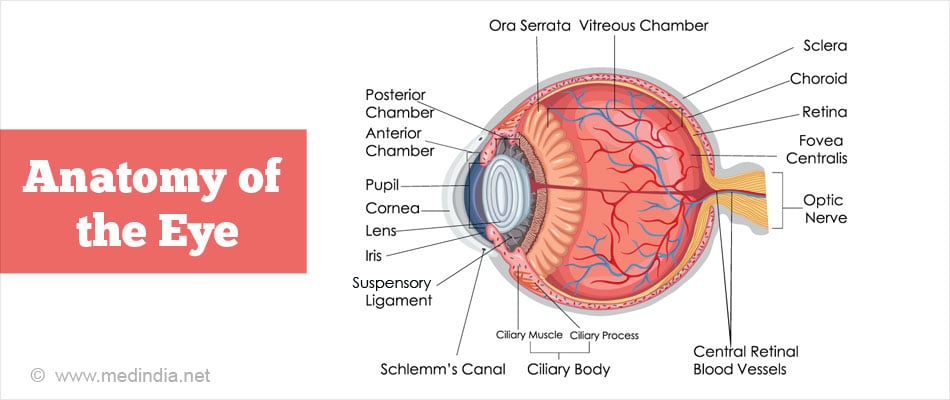
The human eye is separated into anterior and posterior segments, with the lens included in the anterior segment. The lens is responsible for focusing the light entering the eye. The posterior segment of the eye is filled with a transparent, jelly-like fluid called the vitreous humor that maintains the shape of the eyeball and provides a clear path for light to travel to the retina, which is the photosensitive coating on the inner aspect of the posterior part of the eye. The optic nerve is connected to the retina at the back of the eye and carries nerve impulses to the brain, which interprets these signals as images. The front part of the eye or the anterior segment is filled with a watery fluid called aqueous humor which provides nutrients to the tissues of the eye. It is divided into an anterior chamber and a posterior chamber. Separating these two chambers is the iris, which is the colored part of the eye. The central opening of the iris is called the pupil, which appears black. The transparent dome through which the iris can be seen is called the cornea. The angle is the place where the cornea meets the iris. In this space is the trabecular meshwork which forms a drainage system through which the aqueous humor drains. The angle may become narrowed causing pressure build-up and damage to the optic nerve, which is called narrow-angle glaucoma or angle closure glaucoma.
![Anatomy of the Eye Anatomy of the Eye]()
There are several types of iridectomy depending on its location on the iris:
- Peripheral Iridectomy: In this type of iridectomy an opening is made in the periphery (away from the centre) of the iris either surgically or by a laser. The pupil is kept intact.
- Sector Iridectomy: This type of iridectomy removes a radial section of the iris, extending from the pupil to the periphery. As a result, the pupil appears like a keyhole. Nowadays this is used only for iris or Ciliary Body Melanomas.
- Optical Iridectomy: This type of iridectomy is performed for the purpose of improving vision by enlarging the existing pupil or creating an artificial pupil, in cases of central opacity of the cornea. This procedure is not performed today because of improved techniques of corneal transplantation.
Patients suffering from the following eye conditions should undergo this procedure:
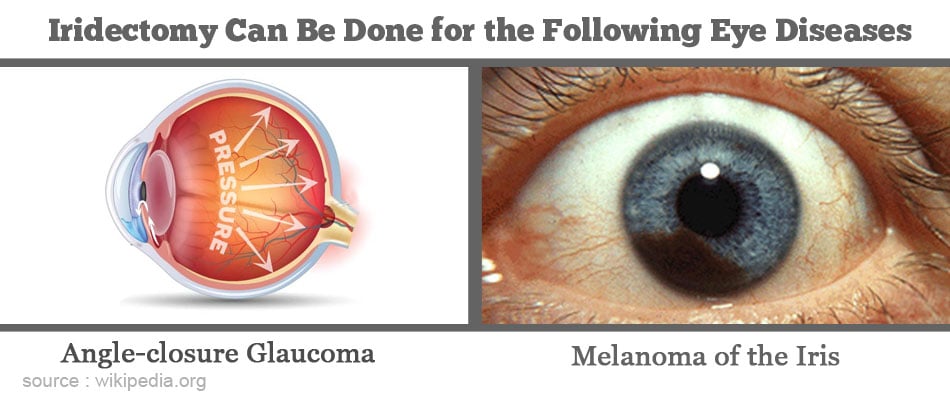
- Angle-closure Glaucoma: In certain people, more commonly women, especially those with a small eye and hypermetropia (commonly referred to as far sightedness), there is a tendency for the drainage angle in the anterior chamber of the eye (that provides passage for aqueous to reach the trabecular meshwork) to get closed when the pupil dilates. This prevents drainage of aqueous, the buildup of which results in a very high pressure in the eye. This is referred to as acute angle closure or acute congestive glaucoma.
- Acute angle closure causes a severe pain in the eye with diminished vision and headache.
- Sometimes attacks of rise of pressure that resolve spontaneously occur: this is referred to as intermittent angle closure.
- Sometimes one comes across a person with a dangerously narrow angle (which is capable of closure) without any symptoms this person is referred to as an angle closure suspect.
Laser iridotomy is performed in all of the three conditions above in both eyes, as angle closure glaucoma is a bilateral condition. In angle closure suspects, laser iridotomy is indicated so as to prevent an attack of acute angle closure (that may occur whenever the pupil dilates).
- Patients Suffering from Melanoma of the Iris or Ciliary Body: Melanoma is a tumor of the pigment-forming cells of the iris or Ciliary Body and if left untreated, can result in loss of vision. The melanoma can also spread to other parts of the body, most commonly the liver, and eventually cause death. The melanin pigments are responsible for the color of the iris.
- Surgical iridectomy is performed routinely in patients undergoing the following surgeries
- Glaucoma surgery (trabeculectomy)
- Phakic IOL (implantation of an intraocular lens without removing the crystalline lens)
- Implantation of an intraocular lens in the anterior chamber of the eye
Routine Tests: Patients undergoing a surgical iridectomy may need the following tests to be done.
- Blood tests like hemoglobin levels and blood sugar.
- Urine tests
- ECG to study the electrical activity of the heart
Specific Tests: The routine tests are followed by tests that are specific to the eye condition, which involve detailed examination of the eye. Two tests are of particular importance and are briefly highlighted below:
- Tonometry: This is a painless procedure that measures the fluid pressure within the eye, using an instrument called a tonometer. In this procedure, a drop of anesthetic is applied to the eye and the tonometer is touched on the eye surface to measure the fluid pressure directly. An indirect method involves use of an air puff, hence there is no direct contact of any instrument with the eye.
- Gonioscopy: This test uses a special mirrored contact lens to examine the angle between the iris and cornea. The doctor applies a drop of local anesthetic on the eye and then touches the surface of the cornea with a gonioscopic lens. He/she then uses a slit lamp to magnify the image formed on the lens.
Patients who are scheduled to undergo laser iridotomy do not require any special preparation for the procedure.
Procedure for Laser Iridotomy: In laser iridotomy, the ophthalmologist uses a laser, (Nd:YAG laser) to punch a tiny hole (0.5 mm) in your iris, through which the aqueous humor can drain. First, the doctor will put some drops of a drug called pilocarpine in your eye, which will constrict the pupil. This is followed by adding some local anesthetic drops for numbing the eye. You will be made to sit comfortably in a special chair, with your head resting on a support to prevent any movement. Then the laser is used to make the opening in the iris. This will not affect your vision, as the opening is made at the periphery of the iris, usually underneath the eyelid, so that it remains out of view. The laser procedure takes just 5 minutes to complete.
Procedure for Surgical Iridectomy:
- Pre-operative Check-up: Routine tests as indicated above are ordered a few days before the surgery. If you are on blood thinners or aspirin, your doctor may advise you to stop them a few days before the procedure. You may be prescribed some eye drops for applying to the eye for a few days before the surgery.
- This is a day care surgery and so you may reach the hospital on the day of the procedure after a light breakfast
- Type of Anesthesia: Surgical iridectomy is performed under local anesthesia wherein a local anesthetic is injected into the tissues around the eye.
![Surgical Iridectomy Is Performed Under Local Anesthesia Surgical Iridectomy Is Performed Under Local Anesthesia]()
- Shift from the Room or Ward to the Waiting Area in the Operating Room: An hour or two before the surgery, you will be shifted to the operating room waiting area on a trolley. Once the operating room is ready, you will be shifted there.
- Shift to the Operating Room: The ambience in the operating room can sometimes be very daunting and a small amount of sedation can help overcome your nervousness. From the trolley, you will be shifted onto the operating table. The operating light console will be directly above and at the head end will be the anesthesia machine. There may also be monitors to check oxygen levels, heart activity (ECG machine) and other vital parameters. A constant beeping sound may be present from the monitors, which may sometimes be irritating.
You will be made to lie on the operating table and a sterile cloth with a hole will be placed over your eye so that the eye is clearly visible to the surgeon. The surgeon will use a small microscope and special miniature surgical instruments to make an incision into the cornea, followed by excision of a portion of the iris, usually at the top of the eye on the vertical axis. The corneal wound can be stitched, but is usually self-healing.
You can return home on the same day. You may also be recommended to wear a patch over the operated eye for a few days. Avoid strenuous activity for at least 3 weeks. In the long-term, you should have regular check-ups following an iridectomy for treating angle-closure glaucoma. In case of melanoma too, regular check-ups are a must in order to prevent the recurrence of the tumor.
The risks and complications of conventional (surgical) iridectomy and laser iridotomy overlap to some extent. However, there are also some complications that are specific to each of these two procedures. These are briefly listed below:
Common Complications of Conventional Iridectomy and Iridotomy:
- Bleeding
- Scarring at the site of incision (iridectomy) or laser beam contact point (iridotomy)
- Failure to relieve fluid pressure in the eye due to closure of the iridectomy
Specific Complications of Conventional Iridectomy:
- Risk of infections
- Risk of cataract formation
Specific Complications of Iridotomy:
- Inflammation of the eye
- Temporary rise of intraocular pressure
Besides the above listed complications, there are some risks involved in an iridectomy for melanoma of the iris. These include the following:
- Glaucoma due to growth of new blood vessels near the angle
- Cataract formation
- Recurrence of the tumor
The prognosis or outlook of a conventional iridectomy or laser iridotomy is generally very good. In the long-term, the intraocular pressure (IOP) is lowered. In case of melanoma, which has a slow growth rate, if promptly treated, the survival rate can be as high as 95-97% after 5 years.