What is Fontan Procedure?
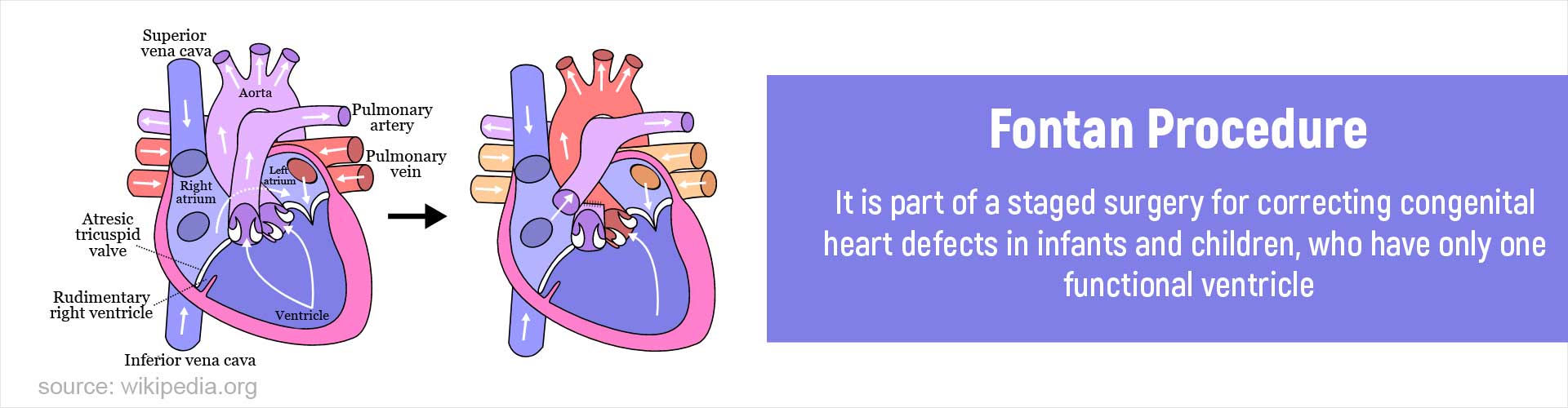
- The Fontan procedure or Fontan-Kreutzer procedure is the final stage of a radical palliative surgical procedure used in infants and children who have only one functional ventricle.
- In the Fontan completion procedure described below, venous blood entering the right atrium via the inferior vena cava (IVC) is diverted to the pulmonary artery without passing through the morphologic right ventricle (which, along with the left ventricle, is functionally a single ventricle). It is done between 2-3 years of age.
- The first stage or the Glenn operation is done before 2 years and redirects blood from the superior vena cava (SVC) directly into the lungs via the pulmonary artery.
- The procedure was first described in 1971 by Dr. Francois Marie Fontan (France) and Dr. Guillermo Kreutzer (Argentina) separately as a surgical therapeutic procedure for tricuspid atresia.
Anatomy & Physiology of the Heart in Brief
The normal human heart is four-chambered, consisting of two atria and two ventricles. The venous return from the body is emptied into the right atrium via the two great veins namely the superior vena cava (SVC) and the inferior vena cava (IVC). This venous blood in the right atrium then flows into the right ventricle via the tricuspid valve. The right ventricle pumps this deoxygenated blood through the pulmonary artery to the lungs, where it gets oxygenated. The purified blood then returns to the left atrium via the pulmonary veins and flows into the left ventricle, which contracts and pumps the blood into the aorta to be carried to the rest of the body.
Overview of the Surgical Treatment
For children born with only a single functional ventricle, the single chamber is overworked, pumping blood both to the lungs as well as to the rest of the body. As enough blood is not reaching the lungs for oxygenation, the child becomes blue and cyanotic and surgery becomes necessary to improve oxygenation of the blood. The correction is done in stages as it is not possible to undertake the entire correction in a single sitting.
Following these surgical procedures, the child will appear healthier and the skin will assume a rosy-pink appearance since almost all of the blood returning to the heart goes to the lungs first for oxygenation.
What are the Types of Fontan Procedure?
Three types of Fontan procedure have been described:
- The original Fontan procedure is also known as the atriopulmonary connection technique, where a connection is made between the right atrium and the pulmonary artery.
There are two other types of Fontan procedure that are currently used:
- Lateral Tunnel Method: This method is technically known as intracardiac total cavopulmonary connection. Here, a lateral tunnel connects the upper part of the right atrium and the underside of the pulmonary artery that goes to the lungs.
- Extracardiac Method: This method is also known as extracardiac total cavopulmonary connection. Here, the IVC is cut from the heart and attached to a tube that connects it to the underside of the pulmonary artery, thereby diverting the blood flow outside the heart.
Why it is Done?
The major heart defects where the Fontan procedure is recommended include the following:
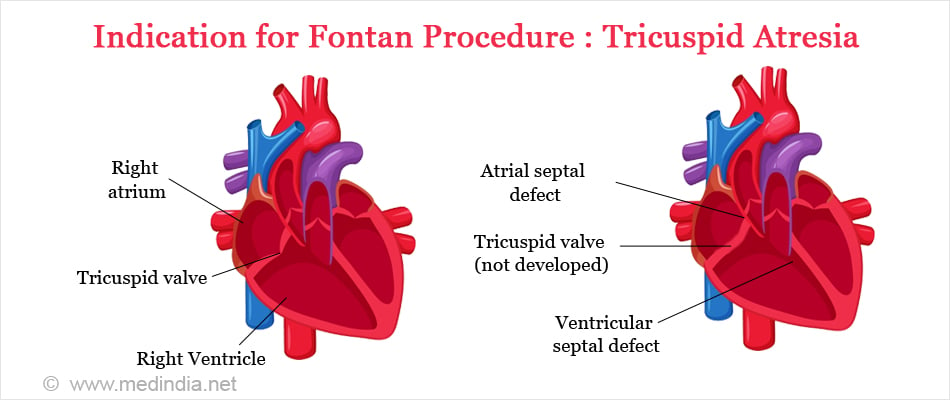
- Tricuspid atresia with no blood reaching the right ventricle
- Hypoplastic left heart syndrome
- Pulmonary atresia with underdeveloped right ventricle
- Double inlet left ventricle
- Double outlet right ventricle with associated defects that prevent repair.
How do you Prepare before Fontan Procedure?
Before your child undergoes the Fontan procedure, some routine tests will need to be done.
Routine Tests
All patients who undergo an elective surgery (which is more planned), routine tests are required and include the following:
- Blood tests like hemoglobin levels, blood group, liver and kidney function tests
- Urine tests
- ECG to study the electrical activity of the heart
- Chest X-ray
Specific Tests
Patients, who require a Fontan surgery, very often have liver problems. Therefore, besides the standard liver function test (LFT) certain specific tests are also recommended.
Blood Tests: These tests measure the levels of certain chemical substances that are specific for liver disease in Fontan patients. Liver function tests include the enzyme gamma-glutamyl transferase (GGT), serum bilirubin, total protein, serum albumin, and prothrombin time (PT), which is a blood clotting test.
Ultrasound Scan: Ultrasonography (USG) uses a machine that emits ultrasound waves (above the audible range) that penetrate the patient’s body and deflects back to a receiver, which form images of the internal organs. USG can detect swelling and inflammation of the liver (hepatomegaly). Other abnormalities include dilation of the hepatic vein, accumulation of fluid in the peritoneal cavity of the abdomen (ascites), as well as formation of nodules on the surface of the liver.
CT Scan: A computed tomography (CT) scan can be used to confirm and corroborate the USG findings such a hepatomegaly. In this procedure you will be asked to lie down still on a special table for a few minutes. A doughnut-shaped instrument will pass over the chest, and images of the heart will be taken. A contrast may be injected into your vein; therefore you should inform the radiologist if you suffer from any allergies.
Liver Biopsy: This technique studies thin slices of diseased tissue on a microscopic glass slide by staining with colored dyes, followed by viewing under a microscope. The most distinctive feature of the liver tissue is the color, which is usually reddish-brown with a yellow background. For this reason, this type of liver is termed as “nutmeg liver”.
What Happens During the Fontan Procedure?
Pre-operative Check-up: Routine tests as indicated above are ordered a few days before the surgery. Admission is required a day or two before the surgery. If your child is on blood thinners or aspirin, these should be stopped a few days before the procedure.
Fasting Before Surgery: Overnight fasting is required and occasionally intravenous (IV) fluid may be required to keep your child well hydrated. Sedation is sometimes required for good overnight sleep before the surgery.
Type of Anesthesia: The Fontan procedure is done under general anesthesia (GA).

Shift from the Room or Ward to the Waiting Area in the Operating Room: An hour or two before the surgery, your child will be shifted to the operating room waiting area on a trolley. Once the surgical room is ready, he/she will be shifted to the operating room.
Shift to the Operating Room: The ambiance in the operating room can sometimes be very daunting and a small amount of sedation can help overcome your child’s nervousness. From the trolley, your child will be shifted on to the operating table. There may also be monitors to check oxygen levels, heart activity (ECG machine) and other vital parameters.
Anesthesia Before Surgery: The anesthetist will inject drugs through an IV line and make your child inhale some gases through a mask that will put him/her in deep sleep for anesthesia. Once your child is in deep sleep, a tube will be inserted into the windpipe to administer the anesthesia gases to overcome pain and keep him/her comfortable.
Surgical Strategy: The surgical strategy aims to optimize the so called “Fontan circulation”, which refers to the configuration where the single ventricle pumps the oxygenated blood returning from the lungs throughout the body, and the deoxygenated blood returning from the body passes directly via blood vessel connections to the lungs without any pumping mechanism. The Fontan procedure is the third and final stage in the reconstruction of a single ventricle defect and therefore, is also known as the Fontan completion operation.
Surgical Procedure: The surgery involves opening the chest or thoracic cavity by cutting through the sternum (bone to which the ribs are attached at the midline). This enables the surgeon to directly access the heart to carry out the operation.
The surgical procedure utilizes either the lateral tunnel method or the extra-cardiac method to enable the venous blood to reach the lungs. In either of these methods, a hole or “fenestration” is made between the Fontan circuit and the right atrium to ease pressure build-up. The post-operative recovery phase is more stable in patients who have fenestrations and they also have less prolonged pleural effusions, which is a common complication of the surgery. The fenestrations may close spontaneously a few months post-surgery, or can be done by cardiac catheterization, in which a long thin tube (catheter) is inserted in an artery or vein in the neck or arm and threaded through the blood vessels into the heart.
What Happens after the Fontan Procedure?
- Waking up from Anesthesia: Once the surgery is over your child will wake up and the tube down the wind pipe will be removed. Your child will be asked to open his/her eyes before the tube is removed. There may be a tube going into the stomach called a nasogastric or Ryle’s tube to keep it empty. There will also be an IV line. Your child will remain on oxygen. Once fully awake, your child will be shifted on the trolley and taken to the recovery room.
Recovery after Fontan Procedure
- Recovery Room: In the recovery room, your child’s vitals will be monitored and observed for an hour or two before shifting to the room or a ward. Painkillers may be prescribed depending on the extent of the pain.
- Post-operative Recovery: Your child will remain in the hospital for a few days following the procedure. Normally, on the first day, your child will not be allowed much to drink or eat. Once the bowels start recovering, your child will be given fluids and a light diet. This may take one to three days.
- Change of dressing will be done as required. The IV lines for fluids and drugs will continue for a few days till your child starts eating normally.
What are the Risks & Complications of Fontan Procedure?
As with any type of surgery, bleeding is an inherent risk of the Fontan procedure. Besides this general risk, there are some complications that a specific to the Fontan procedure:
- Stenosis (narrowing) of pulmonary arteries, leading to pulmonary hypertension (increased pulmonary blood pressure).
- Atrio-ventricular valve regurgitation (backflow of blood due to a defective heart valve between the atrium and ventricle).
- Stenosis (narrowing) of the surgically constructed tube or conduit.
- Formation of blood clots and emboli, including pulmonary embolism.
- Increased pressure in the IVC causing liver damage (cirrhosis), liver failure, liver cancer, and increased blood pressure in the liver blood vessels (portal hypertension).
- Ventricular failure causing inability to perform strenuous exercise (exercise intolerance), ischemia, and infarction.
- Pleural effusion or collection of fluid around the lungs leading to breathlessness and a longer hospital stay.

 MEDINDIA
MEDINDIA
 Email
Email