- Liver Transplant - (https://www.niddk.nih.gov/health-information/liver-disease/liver-transplant)
- Harrison’s Principles of Internal Medicine 19th edition
- What is cirrhosis? - (https://www.niddk.nih.gov/health-information/liver-disease/cirrhosis)
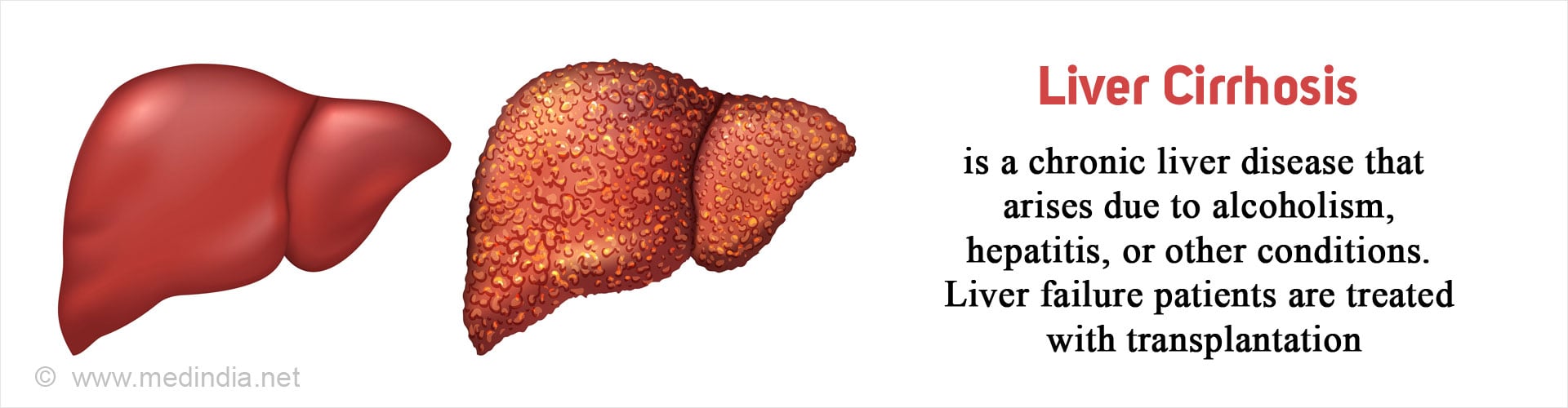
What is Liver Cirrhosis?
Liver cirrhosis is a form of advanced liver disease where the liver becomes dysfunctional with the formation of scar tissue and nodules.
The liver is one of the most important organs of our body. It is a large organ located just below the ribcage on the right side of the abdomen. It performs multiple functions – production of bile, processing of food, detoxification of blood, formation of clotting factors, and providing immunity from diseases. Thus, diseases affecting the liver have a wide range of consequences throughout the body.
What are the Causes of Liver Cirrhosis?
Liver or hepatic cirrhosis occurs due to chronic damage to the liver resulting in the formation of scar tissue. The liver tries to regenerate to replace the damaged cells, which however are replaced by scar tissue instead, giving the cirrhotic liver a nodular appearance. As more scar tissue replaces functional liver tissue, the patient can go into liver failure due to inability of the remaining liver to perform all the functions.
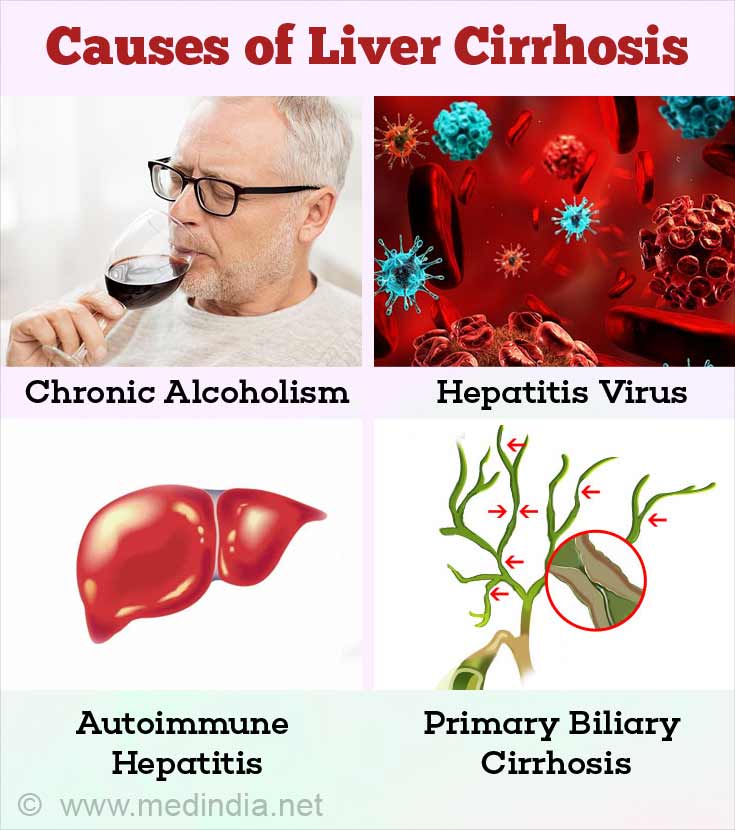
In some cases, the cause of liver cirrhosis is not known. Others may be due to one of the following causes:
- Chronic alcoholism: Liver cirrhosis has often been associated with alcoholism. The initial changes in the liver due to alcoholism include alcoholic fatty liver, which later progresses to alcoholic hepatitis and then cirrhosis. Alcoholism can also worsen other pre-existing liver diseases, thus accelerating cirrhosis.
- Hepatitis C infection: Infection with the hepatitis C virus is a common cause of liver cirrhosis. The virus spreads through blood products, infected needles, sexual contact, and from mother-to-child during childbirth
- Hepatitis B infection: Hepatitis B infection is another viral infection that affects the liver and can cause cirrhosis. It spreads in ways similar to the hepatitis C virus. Vaccination has reduced the incidence of this virus as a cause of cirrhosis. Patients who suffer from hepatitis D infection on top of hepatitis B infection are especially prone to developing cirrhosis
- Nonalcoholic fatty liver disease (NAFLD) and Non-alcoholic steatohepatitis (NASH): NAFLD and NASH occur following accumulation of fat in the liver due to causes other than alcoholism. Obesity is a common cause of NAFLD and NASH
- Autoimmune hepatitis: Autoimmune hepatitis is a condition where the immune system of the body launches an attack against the liver, which could progress to cirrhosis. Genetic factors may be responsible
- Bile duct disease: The bile ducts are small tubules in the liver which join to form larger ducts, and then a single hepatic duct that arises from the liver. The hepatic duct joins the cystic duct from the gall bladder to form the bile duct. The bile duct carries out the secretion of the liver called bile. Damage to the bile ducts can cause accumulation of bile in the liver, which can give rise to liver cell damage progressing to cirrhosis. Conditions affecting the bile ducts that give rise to cirrhosis include primary biliary cirrhosis, primary sclerosing cholangitis, biliary atresia and autoimmune cholangiopathy
- Genetic conditions: Genetic conditions that can affect the liver resulting in cirrhosis include alpha-1 antitrypsin deficiency, hemochromatosis, Wilson disease, galactosemia, and glycogen storage diseases. The liver cells become damaged by abnormal accumulations of certain products of metabolism due to the genetic defect.
- Drugs: Drugs like methotrexate and amiodarone can cause liver cirrhosis as a side effect
- Cardiac cirrhosis: Congestion of the liver following cardiac conditions like chronic heart failure can result in damage of the liver cells and cirrhosis
What are the Signs and Symptoms of Liver Cirrhosis?
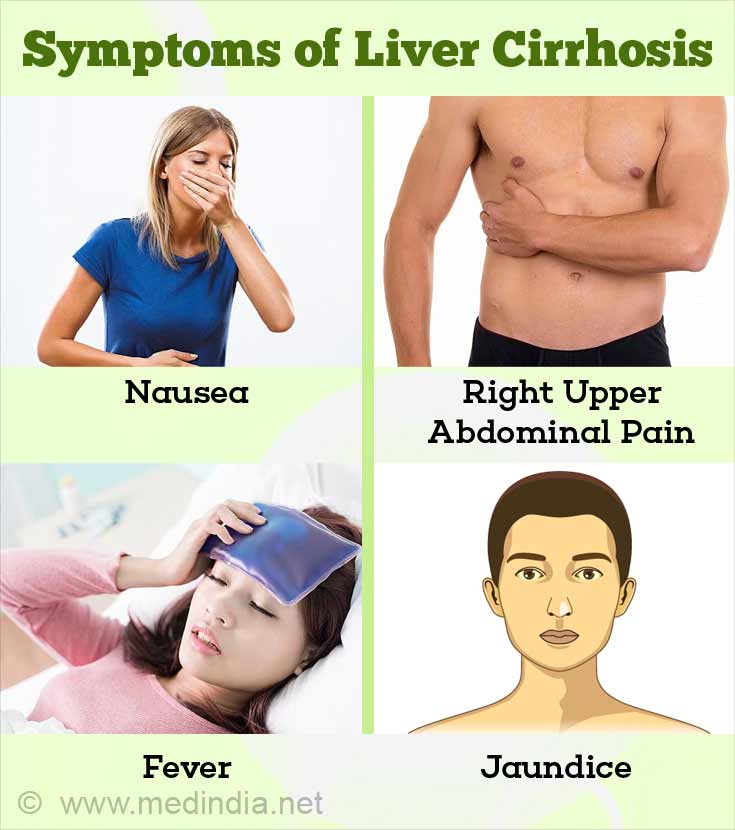
Symptoms and signs of liver cirrhosis include the following:
- Nausea, vomiting, diarrhea, loss of appetite, fatigue
- Pain in right upper abdomen
- Fever
- Jaundice with yellowing of the skin and the eyes
- Itching
- Reddening of the palms and spider web-like reddening of the skin (called palmar erythema and spider nevi, respectively)
- Enlargement of the salivary glands
- Enlarged liver and spleen on examination
- Reduced body hair, smaller testes and enlarged breasts in males
- Menstrual irregularities in females
What are the Complications of Liver Cirrhosis?
Portal hypertension is a common complication associated with liver cirrhosis. The portal vein connects the digestive tract and the spleen to the liver. Scarring of the liver causes high pressure in the portal circulation, which could result in the following:
- Esophageal varices and variceal bleeding: Portal hypertension causes dilation of blood vessels at the base of the food pipe as well as at other sites. The blood vessels can rupture resulting in vomiting of blood and black tarry stools.
- Ascites: The increased portal pressure also causes fluid accumulation in the abdomen (ascites) and in subcutaneous tissues (edema). The person develops an enlarged and tense abdomen. The ascites fluid can get infected resulting in a condition called spontaneous bacterial peritonitis, which requires treatment with antibiotics.
Other complications of liver cirrhosis include the following:
- Hepatic encephalopathy: Cirrhosis can cause brain dysfunction. The patient may suffer from confusion, drowsiness, somnolence and even coma.
- Hepatorenal syndrome: Hepatorenal syndrome refers to kidney dysfunction as a consequence of liver disease. Patients with liver cirrhosis can develop kidney dysfunction, further complicating the situation.
- Problems with blood clotting: The liver normally produces proteins called clotting factors that help in blood clotting. Liver cirrhosis reduces the availability of clotting factors, which may result in excessive bleeding following injury.
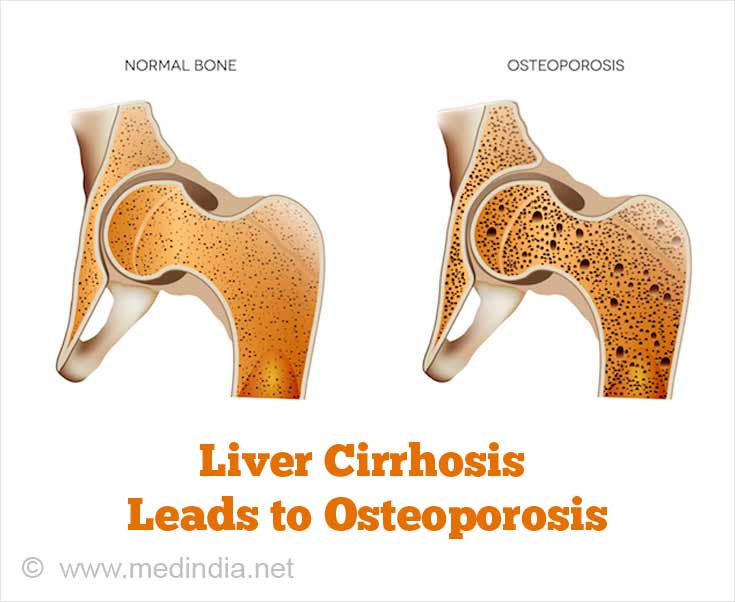
- Osteopenia and osteoporosis: The patient may suffer from thinning of bones, referred to as osteopenia or osteoporosis, thereby increasing the risk of fractures.
How do you Diagnose Liver Cirrhosis?
The patient may give a history of alcoholism or some other cause of liver disease. Tests which help in the diagnosis of liver cirrhosis include the following:
- Blood tests: Blood tests may indicate the following abnormalities:
- Abnormal liver function tests are marked by high bilirubin levels, increased liver enzymes and prolonged blood clotting times. Anemia may also be present
- Blood tests for hepatitis B and hepatitis C may be positive in those suffering from the infections
- Antibodies may be present in those with cirrhosis following autoimmune hepatitis and other autoimmune disorders
- Imaging tests: Imaging tests like ultrasound, CT scan and MRI may be used to study the condition of the liver as well as associated complications. Elastography is a test that is performed either with ultrasound or MRI and is used to detect the stiffness of the liver and the extent of the cirrhosis.
- Cholangiography: Cholangiography is a test used to examine the bile ducts while a dye passes through them. It can help to diagnose problems in the bile ducts, which could give rise to cirrhosis.
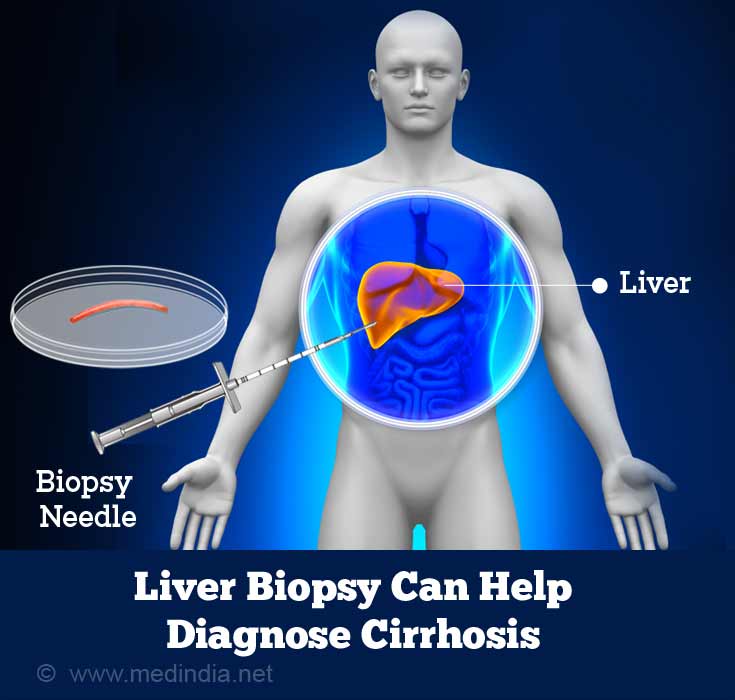
- Liver biopsy: Liver biopsy can help to diagnose cirrhosis. A needle is inserted into the liver and a small piece of the liver is obtained, and is subject to microscopic examination. The procedure is done under local anesthesia.
Blood tests should also be carried out to detect complications of cirrhosis such as renal failure.
How do you Treat Liver Cirrhosis?
The scarring of the liver cannot be reversed. The treatment aims at preventing further progression of the underlying disease and controlling the symptoms and preventing complications.
Treatment of the underlying cause:
- Hepatitis B or hepatitis C infection should be treated with specific anti-viral medications
- Pentoxyphylline may help to reduce inflammation of alcoholic hepatitis
- Primary biliary cirrhosis patients may benefit from treatment with ursodeoxycholic acid
- Autoimmune hepatitis may benefit from drugs that suppress immunity like prednisone and azathioprine
- Trientine and zinc may be used in Wilson’s disease
- The underlying heart disease should be treated in patients with cardiac cirrhosis
Treatment of the symptoms of cirrhosis: Some of the symptoms of cirrhosis should be treated. For example:
- Mild itching should be treated with antihistamines or local remedies. Severe itching may require medications like ursodeoxycholic acid, doxepin, rifampin or naltrexone
Treatment of the complications of cirrhosis:
- Ascites is treated with restriction of salt intake and diuretic therapy. Fluid removal with a needle may be necessary in patients with excess fluid accumulation in the abdomen
- Kidney disease may require treatment with albumin and fresh frozen plasma
- Medications like lactulose and antibiotics like neomycin may be used in patients with hepatic encephalopathy
- Bleeding from esophageal varices should be controlled
- Osteoporosis should be treated with drugs like alendronate and can be prevented by prescribing vitamin D and calcium supplements
- The nutritional status should be assessed and maintained to prevent and treat malnutrition
Patients with liver failure may require liver transplantation. The Model for End-stage Liver Disease (MELD) score is used to determine the eligibility of patients for liver transplantation in adults. It predicts the 90-day survival of patients with end-stage liver disease. Patients with alcoholic liver disease can undergo liver transplantation only if they remain abstinent for a few months.
How can you Prevent Cirrhosis?
Cirrhosis can be prevented taking the following steps:
- Keep your alcohol consumption under control. Avoid drinking more than two drinks a day if you are a woman, and more than three drinks a day if you are a man
- Get vaccinated against hepatitis B viral infection
- Start treatment for hepatitis C or hepatitis B infection as soon as you know you are suffering from it, preferably before any liver damage has occurred
- Treat or prevent obesity by following healthy lifestyle practices like eating a well-balanced diet and exercising regularly