- Glioblastoma - (http://neurosurgery.ucla.edu/glioblastoma)
- Glioblastoma Multiforme - (http://www.aans.org/patient%20information/conditions%20and%20treatments/glioblastoma%20multiforme.aspx)
- About Glioblastoma - (https://en.wikipedia.org/wiki/glioblastoma_multiforme#treatment)
- Glioblastoma (GBM) - (http://www.abta.org/brain-tumor-information/types-of-tumors/glioblastoma.html)
What is Glioblastoma Multiforme?
Glioblastoma multiforme (GBM) is the most common and aggressive type of tumor arising from star shaped cells called as astrocytes that make up supportive tissue of the brain. GBM has long baffled oncologists because of its strong resistance to current treatments options. Despite surgery being the current standard treatment for glioblastoma, which is followed by external beam radiation and the chemotherapeutic medication , the survival rate of glioblastoma patients is less than 5–10% at five years. These tumors are cancerous (malignant) as reproduction of cells is quick and is usually supported by large network of blood vessels.
As these tumors come from normal cells of the brain, invasion is relatively easy and the tumor lives within normal brain tissue. Glioblastomas rarely spread elsewhere in the body.
What are the Different Types of Glioblastoma Multiforme?
- Primary or de Novo: This form makes its presence known quickly and is very aggressive.
- Secondary: This form has a long and somewhat slender growth history, though it is very aggressive. It starts as a low grade, eventually becoming a higher grade tumor. It is seen in people 45 years of age and younger.
What are the Causes of Glioblastoma Multiforme?
Cause is mostly unclear. Risk factors uncommon include genetic disorders like neurofibromatosis and Li Fraumeni syndrome and any previous radiation therapy.
What are the Symptoms and Signs of Glioblastoma Multiforme?
Symptoms vary depending on tumor location.
- Due to its rapid progress, common symptoms seen due to increased pressure in the brain are headache, nausea, vomiting, drowsiness, and seizures.

- Depending on tumor location, there can be weakness on one side of the body, memory defects, visual changes, change in mood and personality, change in ability to think and learn, and speech difficulties.
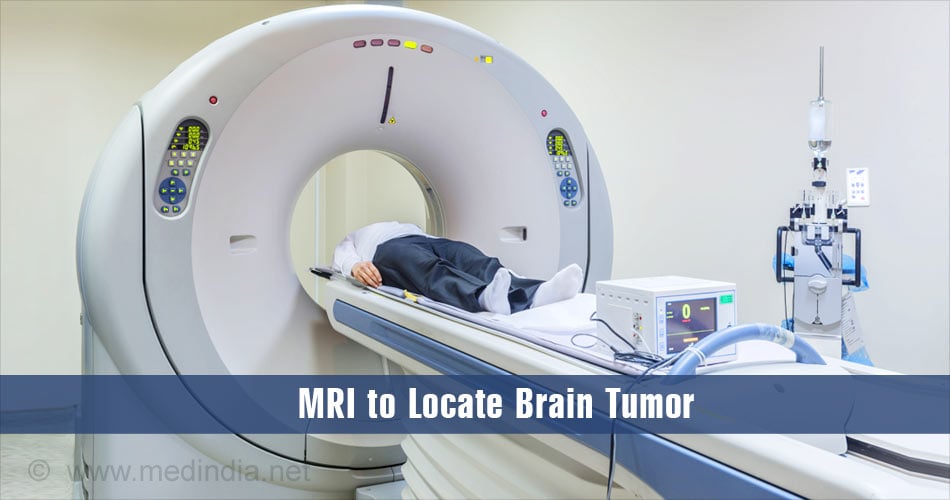
How Do You Diagnose Glioblastoma Multiforme?
Brain tumors can be accurately located by using sophisticated imaging techniques. These include:
- Computed tomography (CT or CAT scan)
- Definitive diagnosis can be done by doing tissue biopsy and removal of tumor, where intraoperative MRI may also be helpful.
- Magnetic resonance spectroscopy (MRS): to examine tumor's chemical profile
- Positron emission tomography (PET scan) to detect tumor recurrence
- Magnetic resonance imaging (MRI)
How Do You Treat Glioblastoma Multiforme?
Treating malignant brain tumor depends on many factors such as tumor size, rate of growth, and patient symptoms. There are various approaches to treat the tumor:
- Surgery: Open skull procedure or craniotomy is usually the first line of treatment if the patient presents with symptoms which are life threatening or ones that significantly affect the quality of life. Surgery is not performed in cases where the tumor is situated at an inaccessible location or near critical structures, which can cause further damage to other areas of brain. Also, surgery may not be carried out if the patient is unhealthy to tolerate the burden of operative procedures.
A high-powered microscope may be used during surgery; this is referred to as microsurgery. Here, surgeon uses a microscope for magnifying the surgical field.
- Ultrasonic Aspiration and Polymer Wafers: The brain tumor can be removed using ultrasonic aspiration instead of scalpel. These ultrasonic waves cut down the tumor and the broken pieces are then removed by suction. After surgical removal of tumor, BCNU polymer wafer implants may be incorporated at the site of tumor. These wafers are biodegradable and gives out chemotherapeutic agents over time.
- Stereotactic Radiosurgery is a non-invasive form of treatment done by a neurosurgeon. This is done by using Gamma Knife instrument, wherein many beams of cobalt 60 enter the brain from different sites and reach the tumor, which then act like a scalpel. The beams are not strong enough to destroy normal tissue, but can definitely damage tumor cells thereby causing them to lose their ability to reproduce and carry out another cellular activities. This type of surgery is usually carried out on benign, malignant and metastatic brain tumors and is performed in conjunction with other radiotherapy methods.
- Radiotherapy involves the use of one of many types of linear accelerators machines and is carried out by radiation oncologist. Unlike radiosurgery, this is not a one-session treatment. Further, the dose of radiation is relatively low as compared to radiosurgery. Also, targeting is not exact as compared to radiosurgery. Therefore, normal cells may be destroyed by this procedure.
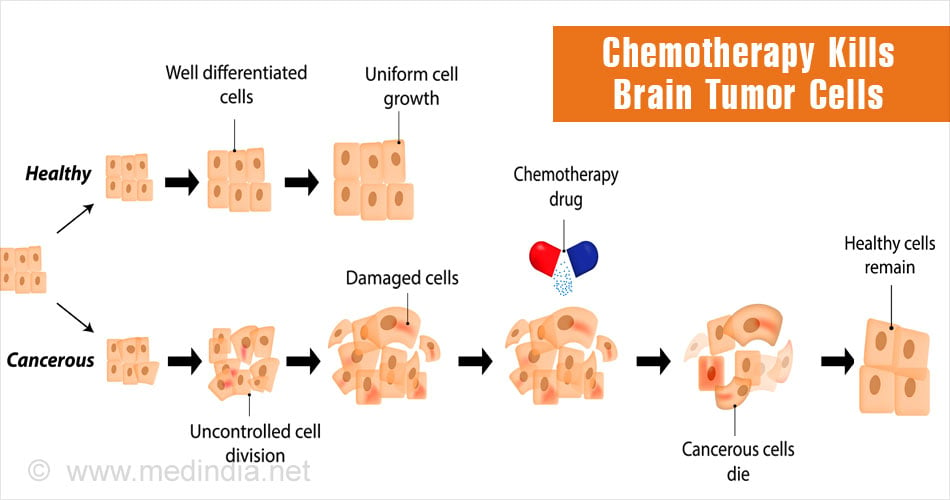
- Chemotherapy involves use of drugs to kill abnormal brain tumor cells; but the drugs can also affect normal cells. Chemotherapy may not be used in cases where tumor shows no response or patient is not in a state of good health. Temozolomide is used for chemotherapy.
- Targeted alpha therapy (TAT) is emerging as a potentially useful adjunctive treatment for glioblastoma
Prevention of Glioblastoma Multiforme
Glioblastoma multiforme may not be a preventable disease. Plenty of research is going on. However, the role of various dietary and nutraceuticals approaches are being investigated.
Health Tips
Depending on symptoms, appropriate supportive measures need to be included.
If:
- Having trouble with walking, then a walker or wheelchair should be made available at home.
- Having changing mental status, care plan has to be directed to suit individual need.
- There is a poor prognosis, then discuss the options of having hospice care, which can include effective pain and symptom relief as well as emotional and mental support for the patient and family at home. This can be under the guidance of nurses, a pharmacist, aides, a social worker, a spiritual caregiver, and counselors.

 MEDINDIA
MEDINDIA
 Email
Email