- Monteiro DLM, Trajano AJB, Menezes DCS, Silveira NLM, Magalhães AC, Dias de Miranda FR, Caldas B. Breast cancer during pregnancy and chemotherapy: a systematic review. Revista da Associação Médica Brasileira (English Edition). Volume 59, Issue 2, January–February 2013, Pages 174-180 - (Doi:10.1016/S2255-48231370452-1)
- Blanquisett AH, Vicent CH, Gregori JG, Zotano AG, Porta VG, Simón AR. Breast cancer in pregnancy: an institutional experience. ecancer 9 551 - (DOI: 10.3332/ecancer.2015.551)
Breast Cancer and Pregnancy
Pregnancy is a very delicate time in the life of a woman, physically as well as emotionally. Therefore, when a woman detects a breast lump and is diagnosed with breast cancer during pregnancy, it could have a devastating effect on her and her family. The joy of looking forward to being a mother could be replaced with concern for the self as well as the baby.
However, with the right treatment at the right time, cancer could be kept under control.

Breast cancer is a common cause of cancer in women, and cases of breast cancer have been noted during pregnancy, with an incidence of 1 in 3000 to 1 in 10 000. A term called pregnancy-associated breast cancer or gestational breast cancer is often used, which includes women diagnosed with breast cancer during pregnancy, during breastfeeding or during the first 12 months following delivery.
Diagnosis of breast cancer during pregnancy is often delayed by normal changes in the breast during pregnancy like tender breasts that may mask the lump in the breast. This could result in a delay of treatment and also worsen cancer outcomes.
What are the Chances for Breast Cancer during Pregnancy?
The hormonal changes during pregnancy and breastfeeding may provide a conducive environment for the growth of breast cancer.
- Pregnancy at an older age is an important risk factor for breast cancer during pregnancy.
- Breast cancer is more common in women who are pregnant between the ages of 32 and 38 years.
- The risk for hormone-positive breast cancer is less for those women who have had a full-term delivery at a younger age.
What are the Symptoms and Signs of Breast Cancer during Pregnancy?
Signs and symptoms of breast cancer during pregnancy are similar to those that occur in a non-pregnant state. However, since changes in the breast take place during pregnancy with enlargement of the breasts and increase in density, the lump may not be felt and diagnosis may be delayed. Common signs and symptoms include:
- Asymmetry between the two breasts
- Inward turning of the nipple
- Puckering of the skin of the breast
- Blood-stained discharge from the breast
- Lump in the breast or the underarm
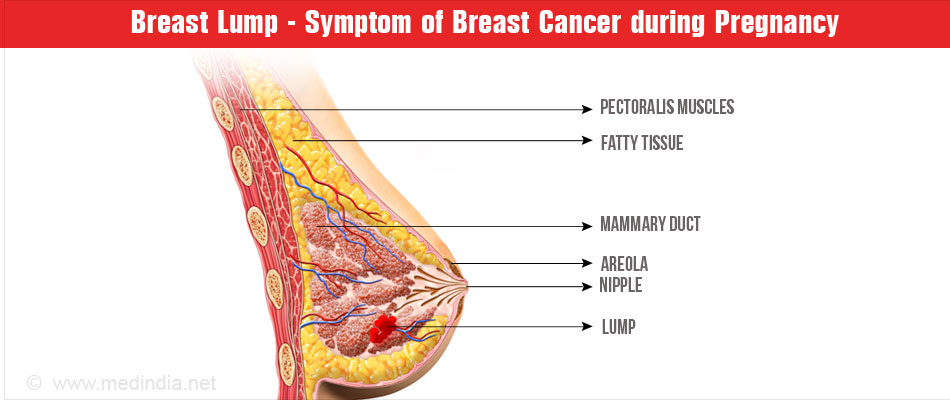
How do you Diagnose Breast Cancer during Pregnancy?
Breast cancer during pregnancy is based on the following:
- Reporting of a Lump in the breast by the woman
- Examination of the Breast: A routine clinical breast examination should be conducted during pregnancy to detect for any lumps
- Imaging Tests: Radiation exposure should be minimized during pregnancy and should be particularly avoided during the first trimester during pregnancy. PET scan, bone scan and CT scan should be avoided due to their associated radiation. Tests that may be performed during pregnancy include:
- An ultrasound of the breast, which is usually safe during pregnancy.
- MRI (Magnetic resonance imaging). Contrast dye during MRI should be avoided.
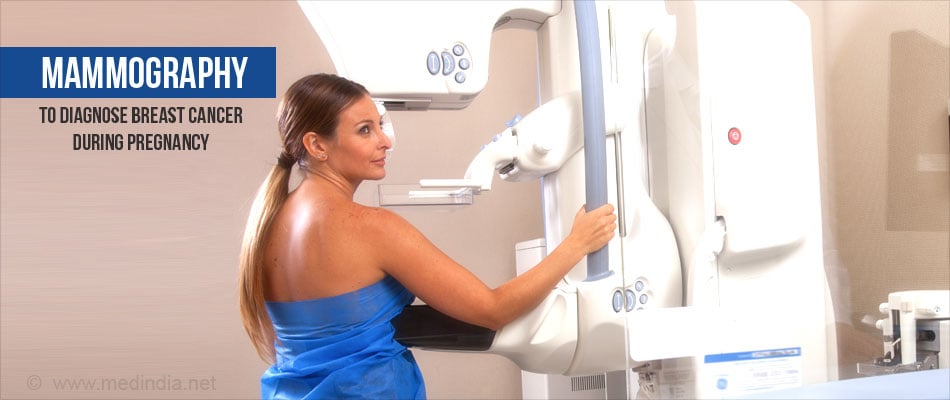
- Mammography. The abdomen may be shielded during the procedure to prevent damage to the fetus. However, the diagnosis may be missed on mammography due to increased density of the breast during pregnancy.
- Biopsy: During a biopsy, cells from the lump may be aspirated with the help of a special needle (fine needle aspiration biopsy), or a part or the whole lump may be surgically removed. Once the cancer is confirmed, the tissue is subjected to additional tests for the presence of estrogen and progesterone receptors, human epidermal growth factor type 2 receptor (HER2/neu), and multigene tests which include Oncotype DX and MammaPrint. These tests predict the spread of cancer and the likely treatments to be effective. Biopsy of the lymph nodes will help to understand if cancer has spread. Sentinel lymph node biopsy, a normal procedure where the first draining lymph node is removed to test for cancer, should not be done since it requires the injection of a dye, which should not be used during pregnancy.
How do you Treat Breast Cancer during Pregnancy?
Breast cancer per se does not affect the baby. Breast cancer during pregnancy should be treated early to prevent its spread. At the same time, treatment should be modified from normal breast cancer guidelines to prevent any harm to the fetus. Most of the available guidelines are based on limited experience with the condition. The benefits and risks of each treatment should be explained to the patient so that she can take part in the decision-making process.
Treatment of breast cancer during pregnancy depends on the:
- Stage of Cancer: Staging of cancer is necessary to understand the extent of cancer, to assess the treatment options and the likely outcome for the patient. A cancer at a later stage indicates that cancer has spread and the outlook may not be favorable for the woman
- Duration of the Pregnancy: Treatment of breast cancer that is discovered during late pregnancy may be postponed for a short duration till the delivery of the baby. Breast cancers discovered early in pregnancy may require some tough decisions
- Overall health of the patient and the baby
- Preference of the woman
Surgery
Breast cancer during pregnancy is usually treated with surgery through the procedure of modified radical mastectomy. The surgery removes the entire affected breast along with draining lymph nodes, lining of chest wall muscles and sometimes some of the chest wall muscles. Risks of surgery include miscarriage of the baby or preterm delivery.
The other surgical option is to use conservative treatment, where only the cancer is removed and the remaining breast is retained. If this approach is used, radiation which is normally used along with conservative surgery should be delayed to after the delivery of the baby to prevent any harm to the baby.
Chemotherapy
Chemotherapy should not be administered during the first trimester due to the risk of fetal malformations. It may be given later during pregnancy, but there could be some risks like risk of premature delivery. Chemotherapy should also be avoided after 35 weeks of pregnancy and within 3 weeks of delivery due to a risk of reducing of blood counts. Drugs belonging to the taxanes group (e.g. docetaxel. paclitaxel) should be avoided.
Hormonal Therapy
Hormone therapy with the use of drugs like tamoxifen is used in the treatment of hormone receptor positive-breast cancer. Hormone therapy should not be used during pregnancy but should be delayed till after delivery.
Targeted Therapy
Targeted therapy with drugs like trastuzumab is used for aggressive human epidermal growth factor type 2 receptor (HER2/neu) positive breast cancer. It should not be used during pregnancy because of possible harmful effects on the fetus, but can be used after delivery.
Radiation Therapy
Radiation is not used during pregnancy to avoid its harmful effects on the fetus, but can be used after delivery if a conservative surgery to preserve the breast is performed.
Termination of Pregnancy
Termination of pregnancy does not alter the course of the breast cancer and is not recommended as treatment for breast cancer during pregnancy. It may be offered as an option in case of aggressive cancers that require immediate treatment with medications or radiation that could be harmful to the baby.
Breastfeeding
Lactation may have to be suppressed to reduce the vascularity of the breast and facilitate surgery. Chemotherapy drugs may pass on through the breast milk to the baby and can harm the baby. Therefore, breastfeeding during chemotherapy treatment is not advised.

Management of Pregnancy in Women Undergoing Breast Cancer Treatment
Another scenario that has to be considered is if a woman on treatment for breast cancer with chemotherapy or hormonal medications becomes pregnant. Under such circumstances, the option of termination of pregnancy may have to be offered due to the risk of congenital malformations with these drugs. If the woman was on trastuzumab, which does not cross the placenta in early pregnancy, there is a chance that the fetus may not be affected and the pregnancy can be allowed to continue if trastuzumab is stopped immediately. These recommendations are, however, based on observations of a limited number of similar cases.
Health Tips
- Women at a genetic risk for breast cancer should be monitored regularly, even during pregnancy.
- Any breast lump during pregnancy should be immediately reported to the treating doctor.
 MEDINDIA
MEDINDIA
 Email
Email