AML - Diagnosis
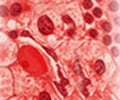
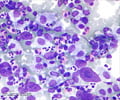
A microscopic examination of the morphology and numbers of the blood cells helps to diagnose AML. Bone marrow aspiration should reveal at least 20% blasts to confirm diagnosis of AML
If the symptoms indicate that a patient has leukemia, the doctor will need to check samples of cells from the patient's blood and bone marrow to be sure of the diagnosis.
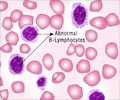
Blood Test / Blood cell examination: When observed under the microscope, changes in the morphology and numbers of different types of blood cells help to diagnose leukemia. Blood cell analysis of most patients with AML show the following -
- Increased numbers of white cells
- Decreased numbers of red blood cells
- Decreased numbers of platelets
- Increased number of immature WBC
Bone marrow examination: A sample of bone marrow cells confirms the diagnosis. A sample is taken from the hipbone by inserting a special needle and navigating it through the bone using a twisting motion. A small amount of aspirate is collected for microscopic examination. This is followed by a bone marrow biopsy by moving the needle further into the bone and removing a portion of the core tissue to be examined microscopically.
The percentage of ‘blasts’ in the bone marrow is particularly vital. At least 20% blasts in the marrow are required for a diagnosis of AML. The bone marrow analysis helps to diagnose leukemia and also to tell if the patient is responding to treatment. In order for a patient to be considered to be in remission after treatment, the blast percentage must be no higher than 5% .
Other diagnostic studies undertaken to guide treatment are -
- Blood chemistry tests: In patients with leukemia, these tests help to identify liver or kidney problems due to the spread of leukemic cells or due to the side effects of certain chemotherapy drugs.
- Lumbar puncture or spinal tap: In this procedure, a small needle is used to withdraw cerebrospinal fluid (CSF) from the spinal cavity to be examined for leukemia cells. This is not routinely done for patients with AML.
- Chromosomal aberrations: AML can also be diagnosed if the blasts have a chromosome aberration that is specific to an AML subtype. This is considered even if the percentage of blasts is less than 20%. In certain types of leukemia, exchange of DNA may take place between two chromosomes. This is called a translocation, and can be seen under a microscope. Other aberrations such as inversions, deletions, or additions, are also possible. Recognizing these changes helps to identify the type of AML and is important in determining the prognosis of the patient.
- Cytochemistry: This study involves placing the sample on a microslide and exposing them to chemical stains. These stains react with only certain types of leukemia cells. For example, one-stain causes the granules of AML cells to appear as black spots when observed under the microscope and does not cause changes in ALL cells. These changes that can be seen only under a microscope.
- Flow cytometry: This technique is often used to examine the cells from bone marrow and blood samples. It is very accurate in determining the exact type of leukemia. Special antibodies are created which stick to certain molecules on the leukemic cells. The cells are then passed in front of a laser beam. If the sample contains leukemic cells they emit light, which is measured and analyzed by a computer.
- Immuno cytochemistry: As in flow cytometry, cells from the bone marrow aspiration or biopsy sample are treated with special antibodies that react only to certain molecules. But instead of a laser, the sample is treated in such a way so that certain cells types change color, which can be seen only under a microscope. It is helpful in distinguishing different types of leukemia from one another and from other diseases.
- Molecular genetic studies: Special molecular studies, such as FISH, are also employed
- Imaging Studies: Imaging tests are of limited value as no visible tumors are usually formed. Imaging studies such as X-ray, CT scan, MRI scan and ultrasound are usually done to look for infections or other problems cells.