- Leukoplakia - (https://my.clevelandclinic.org/health/diseases/17655-leukoplakia)
What is Leukoplakia?
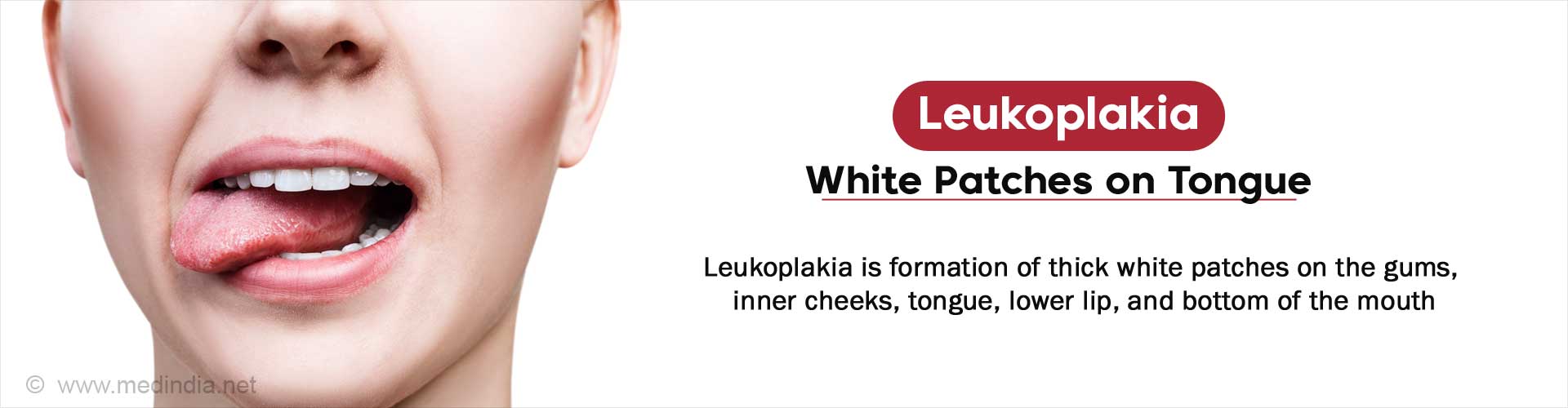
Leukoplakia is a precancerous condition, that is, the stage before cancer development of the mouth. It leads to thick white patches on the gums, inner cheeks, tongue, lower lip, and bottom of the mouth. These thick white patches develop slowly and cannot be scraped off.
Oral leukoplakia usually develops when something constantly irritates the area inside the mouth. Irritation is commonly caused by tobacco chewing and smoking or may be due to rough teeth, ill-fitting dentures, or dental fillings.
Leukoplakia is hyperplasia or an uncontrolled overgrowth of the squamous epithelium (the flat epithelium that lines the oral cavity structures) and can lead to oral leukoplakia lesions. Although it is benign (noncancerous) in the initial stages, various studies have shown that up to 20% of lesions become malignant (cancerous) in a span of 10 years.
Almost 3% to 17.5% of patients with leukoplakia tend to develop squamous cell carcinoma (a common type of skin cancer) within 15 years. This condition is most seen in the elderly patients between 50and 70 years. The risk of leukoplakia evolvement into cancer depends on the cell’s shape, size, and appearance.
What are the Causes / Risk Factors of Leukoplakia?
The exact cause of leukoplakia is unknown. Many cases may not have an identifiable cause (idiopathic). However, it is commonly seen in patients who are in the habit of constantly chewing tobacco or smoking cigarettes, which leads to chronic irritation of the oral tissues. The following are the risk factors that can cause leukoplakia:
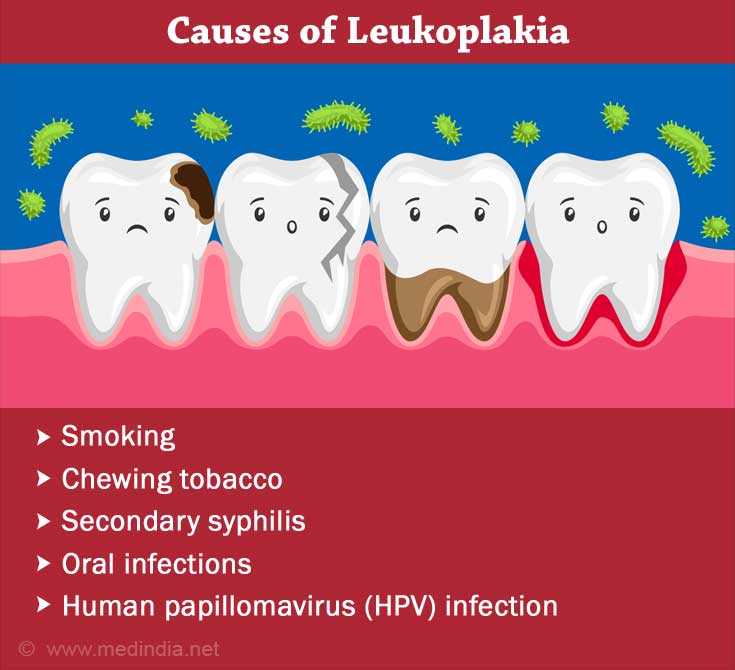
- Tobacco chewing or smoking (especially pipes)
- Vitamin A or vitamin B deficiency
- Holding and chewing tobacco in the mouth for a long period of time
- Sharp or broken teeth rubbing against the tongue or cheeks constantly
- Rubbing of the oral mucosa against ill-fitting dentures and filling
- Secondary syphilis (bacterial infection)
- Human papillomavirus (HPV) infection
- Excessive alcohol intake
- Oral lichen planus – non-infectious rash occurring in the mouth
- Oral thrush– fungal infection of the mouth caused by Candida
What are the Types of Leukoplakia?
The two main types of leukoplakia are:
- Homogenous: A consistently white-colored thin patch with a smooth, ridged, or wrinkled surface throughout.
- Non-homogenous: Irregularly shaped patch in white or white-and-red color, that may be flat, nodular (having protrusions), or verrucous (elevated).
Non-homogenous leukoplakia is encountered to evolve cancerous almost seven times than the homogenous type.
Another type of leukoplakia is called oral hairy leukoplakia, which is caused by the Epstein-Barr virus and is seen in patients with a weak immune system such as HIV/AIDS patients or patients who have undergone bone marrow transplant. It can also be an early sign of HIV infection.
Your dentist or primary healthcare professional will help diagnose and identify the cause of leukoplakia.
What are the Symptoms and Signs of Leukoplakia?
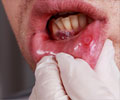
Leukoplakia usually occurs on the inner cheeks, gums, beneath the tongue, and sometimes on the sides of the tongue. Leukoplakia patches show the following characteristics:
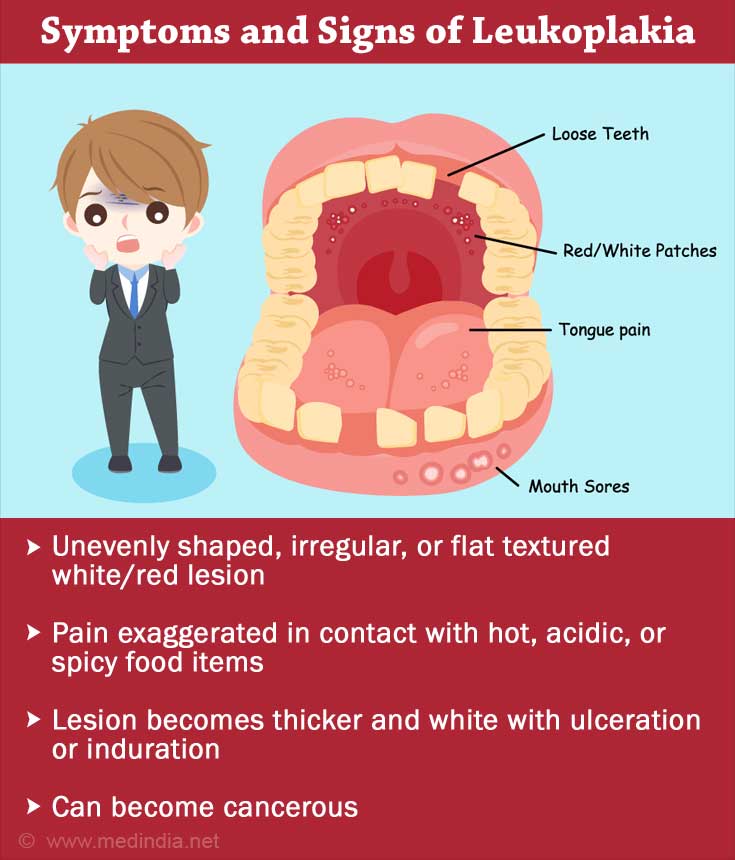
- Earliest lesion is a white or grayish faintly translucent discoloration flush with the mucosal surface
- The lesion cannot be scratched or wiped off
- It is uneven in shape, irregular, or flat textured
- With progression, the lesion becomes slightly raised, thick, or hard in certain areas
- Associated with pain when the patch comes in contact with hot, acidic, or spicy food items
- With further progression, the raised lesion becomes thicker and whiter and may show surface ulceration or induration
Sometimes raised and red lesions referred to as speckled leukoplakia or erythroplakia are seen, which are more likely to be precancerous changes.
Changes in the leukoplakia lesion more likely to be associated with malignant change
- Speckled or verrucous type of leukoplakia
- Presence of ulceration
- Occurrence of a nodule
- Lesion that feels hard around the edges
- Leukoplakia on the floor of the mouth and undersurface of the tongue
How do you Diagnose Leukoplakia?
Consult your doctor if you experience any of the above-mentioned symptoms. Your primary care physician or dentist will take a complete history of your symptoms and examine the patches. Discuss your medical history and lifestyle factors with your doctor.
To confirm the diagnosis of leukoplakia based on initial clinical suspicion, and to rule out the possibility of oral cancer, a biopsy will be performed.
- Oral brush biopsy: In this test, cells from the surface of the lesion are taken for testing with the help of a small, spinning brush. It is a non-invasive procedure; however, it doesn’t always give a definitive diagnosis.
- Excision biopsy: This test involves surgically removing the leukoplakia patch (excision) and sending it for microscopic testing. An excision biopsy is more accurate and helps in giving a definitive diagnosis.
If you have oral hairy leukoplakia, you will be evaluated for conditions that can lead to a weakened immune system such as HIV/AIDS.
How do you Treat Leukoplakia?

- Treatment for leukoplakia is often successful when the lesion is found and tested early in the initial stage.
- In most cases, removing the source of irritation such as quitting tobacco chewing, alcohol consumption, or removing rough teeth, irregular denture surface, or fillings will help in clearing the condition.
- If the leukoplakia patches show early signs of the appearance of cancer, treatment may include removal of the patch either surgically, utilizing laser, or a cold probe that freezes and destroys cancer cells (cryoprobe). However, there are high chances of recurrence, hence frequent check-ups are very important.
- In cases of hairy leukoplakia, you may or may not be given treatment. The condition usually causes no symptoms and is not likely to develop cancer. If your doctor recommends treatment, it may include antiviral medication. These medications act on suppressing the Epstein-Barr virus that causes hairy leukoplakia.
How do you Prevent Leukoplakia?
Quitting alcohol and tobacco is a better way not just to prevent leukoplakia but also to avoid other health hazards. Talk to your doctor to help you quit such addictions. If you continue to indulge in tobacco chewing, smoking, and alcohol intake, remember to have regular dental check-ups to maintain good oral hygiene.