- Cerebral Edema and its Management - (https://www.ncbi.nlm.nih.gov/pmc/articles/pmc4923559/)
What is Cerebral Edema?
Cerebral edema or brain swelling refers to increased amounts of fluid in the brain due to a variety of causes. It causes increased intracranial pressure and is a life-threatening condition requiring urgent management.
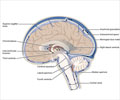
- Normally about 150 ml of cerebrospinal fluid (CSF) is present within the spaces of the brain which remains constant.
- The brain is enclosed within the bony skull and has little or no space to expand due to any cause.
- Thus, when the volume of fluid increases, the swollen brain tissue is compressed against the skull. If left untreated, it can reduce cerebral blood flow and lead to severe ischemic injury.
- If cerebral edema is allowed to progress, it can cause brain herniation (prolapse of the brain into adjacent spaces due to increased pressure) and death.
Therefore, unlike swelling in other tissues, brain swelling has to be diagnosed and treated urgently; else, it may result in irreversible damage to brain tissue resulting in permanent neurological deficits or death due to brain herniation. It is a medical emergency.
Epidemiology of Cerebral Edema
The frequency of cerebral edema is not clear, but it is a fairly common condition and often a secondary feature of several underlying disorders. Cerebral edema has an insidious presentation without specific signs or symptoms, and the diagnosis is often missed. There is no specific diagnostic test for cerebral edema. The diagnosis is often made at post-mortem.
What are the Causes of Cerebral Edema?
Cerebral edema may be caused by traumatic injury to the brain or non-traumatic lesions within the brain, as well as due to miscellaneous factors outside the brain.
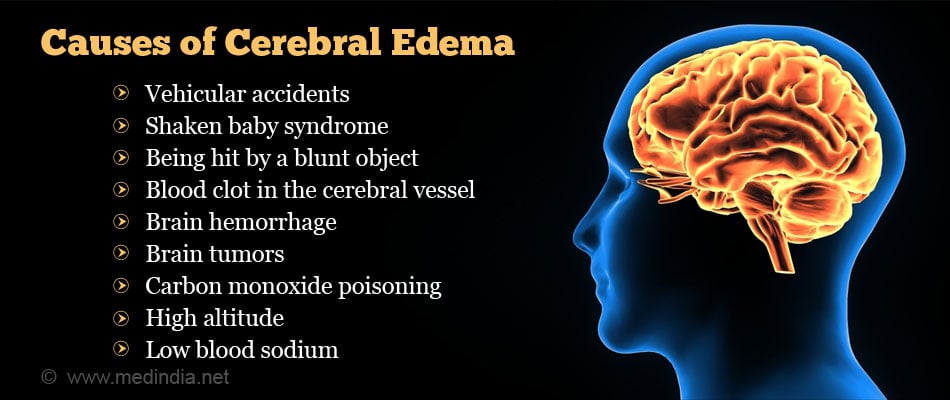
| Traumatic brain injury | Non-traumatic brain lesions | Other Causes |
|
|
|
What are the Types of Cerebral Edema?
The mechanism of development of cerebral edema is complex. It may be caused by a systemic disorder or a localized pathology in the brain.
Cerebral edema may be cytotoxic or vasogenic.
- Cytotoxic edema occurs following brain cell injuryor hypoxia (lack of oxygen) and is associated with swelling of brain cells. This type of swelling predominantly affects the gray matter (nerve cells and some supportive tissue found in the cortex of cerebrum, cerebellum and spinal cord core).
- Vasogenic cerebral edema is due to the influx of solutes and fluid into the brain cells from the blood vessels. The white matter (areas of the brain composed of nerve fibers and not nerve cells) of the brain is mainly affected by this type of edema.
What are the Signs and Symptoms of Cerebral Edema?
Cerebral edema is difficult to diagnose without proper tests and detailed evaluation. Some of the signs and symptoms to look for after a head injury or infection that could indicate brain swelling include
- Headache
- Nausea and vomiting
- Dizziness
- Lack of coordination
- Tingling and numbness
In severe cases or with progression, the following symptoms may be present
- Altered consciousness
- Tiredness and decreased motor activity
- Abnormal breathing pattern
- Elevated blood pressure and decreased pulse rate (Cushing reflex)
- Difficulty in speaking
- Mood disturbances
- Difficulty in walking
- Memory loss
- Visual disturbances
- Incontinence
- Seizures
- Limb or facial muscle weakness

How do you Diagnose Cerebral Edema?
Brain swelling is difficult to diagnose clinically; the presence of one or more of the above symptoms, and the clinical history followed by a detailed neurological examination may raise a suspicion, which needs to be confirmed by the following tests.
Imaging Tests – CT Vs. MRI Scan (imaging of the head to determine the location and extent of the swelling)
- CT scan is the preferred imaging test in a patient with suspected brain swelling.
- The areas of edema appear as low-density lesions on an enhanced CT scan.
- The CT scan may be blurry and may be hard to assess due to the increased water accumulation.
- CT scan can detect the presence of any underlying lesion like an infection, tumor or an infarct that might be causing the cerebral edema.
- CT scan can also be used to follow patients following treatment to determine response to treatment.
- MRI is likely to be more sensitive than CT scan in detecting lymphomas and brain abscess.
- Unlike CT scan, MRI is not readily available and is also much more expensive.
Measurement of intracranial pressure
Intracranial pressure (ICP) is now routinely monitored in patients with suspected elevated intracranial pressure. The three methods to monitor ICP include using an intraventricular catheter, subdural (below the dural membrane covering the brain) sensor or epidural (between the dural membrane and skull) sensor.
Risks associated with these procedures include bleeding, infection, damage to brain tissue, and brain herniation.
Lumbar Puncture
In suspected meningitis, a lumbar puncture is necessary. However, it is important to remember that there is always the risk of herniation during lumbar puncture in the presence of raised intracranial pressure. A CT scan of the head should be done first before attempting a lumbar puncture.
Blood tests:
The following blood tests should be done to identify the possible cause of brain swelling.
- Complete blood count
- Coagulation profile
- Serum electrolytes (hyponatremia or low serum sodium can cause brain edema)
- Liver and renal function tests
- Blood sugar levels
- Arterial blood gas analysis
- Urinalysis for drugs and toxins
- Carbon monoxide levels in the blood
EEG (Electroencephalogram)
An EEG is done to measure brain activity in the presence of seizures. In this test, electrodes are attached to the patient’s scalp, and the electrical activity of the brain is measured that appears as a graph on moving paper or a computer screen.
How do you Treat Cerebral Edema?
Brain swelling is a life-threatening condition and should be treated immediately. Treatment options aim to restore blood flow and oxygen to the brain while at the same time reducing the swelling. Any underlying cause should also be simultaneously treated to prevent any further damage. The various treatment options include
Osmotherapy
Osmotherapy is a treatment meant to draw water out of the brain. This is done using osmotic agents such as mannitol, high-salt saline, glycerol, and drugs such as furosemide. Osmotherapy helps improve blood flow in the brain as well as reduce swelling and raised ICP in the skull.
Hypothermia
Hypothermia has been shown to protect the brain by decreasing metabolic rate and conserving energy. Hypothermia may be sustained for several days and reversed when organ function starts to improve.
Hyperventilation
Controlled hyperventilation may occasionally be resorted to, to help lower ICP. Hyperventilation reduces the amount of carbon dioxide in the bloodstream. The patient has to be intubated and mechanically ventilated. Optimal blood flow to the brain is dependent upon carbon dioxide and controlling this process reduces the blood flow to your brain and helps to decrease the ICP.
Ventriculostomy
This is an invasive procedure to drain fluid from the brain. A doctor will make a small incision in the skull and insert a tube into the space of the brain (ventricle) as a drain. This method will help to relieve ICP.
Surgery
In more severe cases of cerebral edema, surgery may be required to relieve ICP. This could mean removing part of the skull or removing the source of the swelling, such as a tumor.
Supportive Measures:
- Blood pressure control is critical in patients with cerebral edema as hypertension can be dangerous
- Other factors such as diabetes, hypoxia, hyperthermia, acidosis or low blood volume (hypovolemia) should be corrected
- Lumbar puncture has also been found to be useful in some patients to reduce cerebral edema, but extreme caution is required before performing a lumbar puncture in suspected cerebral edema
- Elevation of the head by 15-30 degrees to promote venous drainage and keeping the head in the midline to reduce venous compression in the neck
- Avoid giving glucose containing fluids and maintain blood volume with normal saline
How is Cerebral Edema Prevented?
Prevention of cerebral edema is not always easy. However, the following measures may at least reduce the incidence of cerebral edema in patients at risk.
- Keeping the blood pressure under control, taking anti-hypertensive medications regularly
- Checking blood sugars periodically and being compliant with medications
- Getting periodic follow-ups with the healthcare provider for any chronic illness
- Eating healthy foods and getting regular exercise
 MEDINDIA
MEDINDIA

 Email
Email