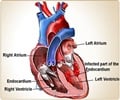
A new study has found that preventive placement of ICDs in patients with a less severe level of heart failure can significantly improve the survival chances.
Sana M. Al-Khatib, M.D., MH.S., of the Duke University Medical Center, Durham, N.C., and colleagues compared survival in Medicare beneficiaries in the National Cardiovascular Data Registry ICD registry with an LVEF between 30 percent and 35 percent who received an ICD during a heart failure hospitalization with similar patients in the Get With The Guidelines-Heart Failure database with no ICD. The analysis was repeated in patients with an LVEF less than 30 percent.
There were no significant differences in the baseline characteristics of the matched groups (n = 408 for both groups). At 1 year, 24.5 percent of ICD patients died vs 24.9 percent of non-ICD patients. At 3 years, 51.4 percent of the ICD patients died, compared with 55.0 percent of the non-ICD patients, a significantly lower risk of death among patients with an LVEF between 30 percent and 35 percent who received an ICD. Presence of an ICD also was associated with better survival in patients with an LVEF less than 30 percent (3-year mortality rates: 45.0 percent vs 57.6 percent).
The authors write that although the difference in absolute risk by 3 years was not large (3.6 percent), it was significant and close in magnitude to what was observed in other clinical trials of prophylactic ICDs. "These results support guidelines'' recommendations to implant a prophylactic ICD in eligible patients with an LVEF of 35 percent or less."
(doi:10.1001/jama.2014.5310; Available pre-embargo to the media atmedia.jamanetwork.com)
Editor's Note: This analysis was funded by a grant from the National Heart, Lung, and Blood Institute. Please see the article for additional information, including other authors, author contributions and affiliations, financial disclosures, funding and support, etc.
 MEDINDIA
MEDINDIA

 Email
Email