Tiny organisms in a child's nose could offer clues to improving the diagnosis and treatment of severe lung infections, shows a study.
TOP INSIGHT
The microbiome profile in child’s nose could help predict the length of hospital stay and also act as a marker of infection severity in the child.
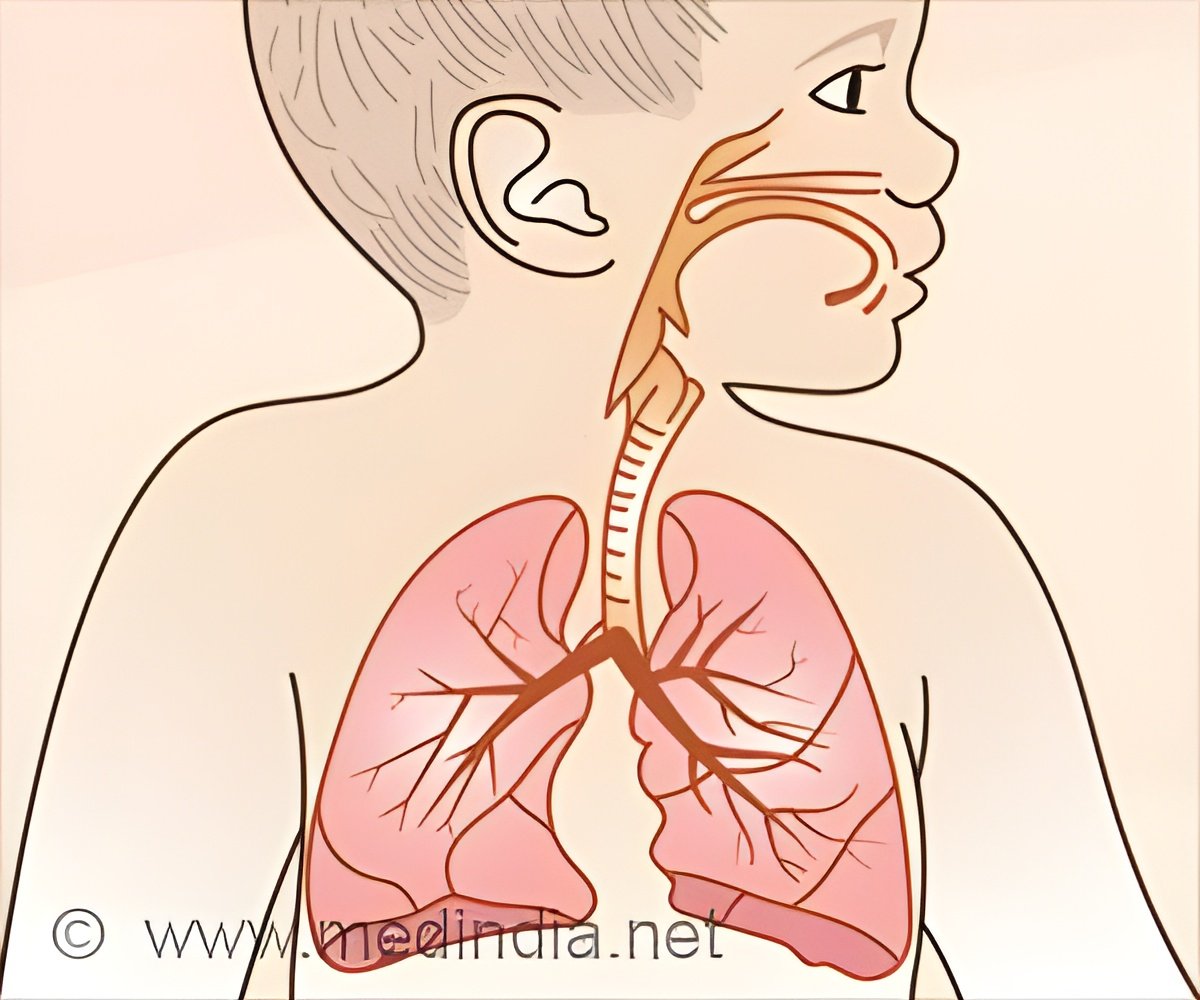
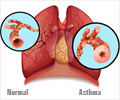
Lower respiratory tract infections (LRTIs), including pneumonia and bronchiolitis, are a leading cause of death in under-fives worldwide. Symptoms include shortness of breath, weakness and fever.
Doctors from the University of Edinburgh worked with teams in The Netherlands to take samples from more than 150 children under the age of six hospitalized with LRTI. They compared these with samples from 300 healthy children.
They found that the microbiome in the back of the nose and throat was related to that seen in the lungs, making it easier to understand and diagnose infections.
Children with LRTI had a different microbiome profile - including the types and amounts of individual viral and bacterial organisms - compared with the healthy children, experts found.
Experts say this breaks with traditional thinking that symptoms predict whether either a virus or bacteria is causing the illness and could impact on a decision of whether or not to use antibiotics.
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email







